Far Reaching Effects of Pituitary Disorders

Guest article by Linda M. Rio, M.A., Marriage and Family Therapist
Originally posted: July 19, 2018; updated Aug 7, 2024
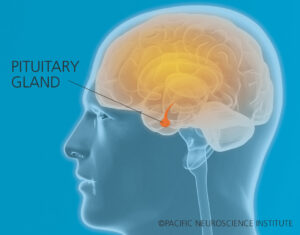
The broad influence of the pituitary gland
Progress is being made to help patients get accurate diagnoses of pituitary tumors and other disorders more quickly. Delays in finding underlying causes of disturbing symptoms have been documented but more and more people are getting to the right doctors. Those “lucky” patients have found top specialists in pituitary tumors and have a team of specialists at a Center of Excellence where innovative medical options and the most highly skilled surgeons offer the best available treatments.
But Western medicine still focuses on the identified patient, which means that others close to the patient often are ignored. The pituitary gland is often called the master gland because it has such a powerful influence throughout the entire body. Dysfunction of this important structure is known to affect many areas of the physical body but also, and lesser known, mental and emotional aspects as well. Any family who has a member dealing with such a powerful force knows that hormonal disruptions can cause family and other relationship disruptions as well.
Pituitary Gland Disorders: A family affair

How do disorders of the pituitary gland affect the family of the patient? Chronic and/or serious physical illness of any kind has far-reaching effects that go far beyond the actual physical symptoms of the disease. Anyone who has had a family member with cancer, physical disability or other serious and/or chronic issues knows that it is like a stranger has moved into the home and disturbed the entire family. The stress for family, especially caregivers, can be enormous. As a result, roles in the family can even become dislodged. Spouses who were once primary bread winners may have to reduce or change their employment or even stop work altogether. The spouse who is not the “patient” therefore may have to take on additional hours of work or go back to work when this was not the plan. Children become affected too. Sometimes kids need to do more chores and go without homework help or a parent to volunteer at school and after-school events. Kids often do not understand a parent’s illness and are sometimes kept in the dark due to mothers’ and fathers’ intentions of trying to protect their young ones. However, problems from this well-intended effort can backfire however.
As pituitary disease progresses
Often a serious physical illness comes on suddenly and is obvious by the outward changes seen in the patient. Other times the symptoms of the pituitary disorder are much more gradual so therefore harder for family members and the patient to detect as a part of an illness. Many of the physical and mental/emotional signs of pituitary disorders develop slowly. Patients often report having gone from doctor to doctor to doctor and even seeking psychological counseling all to no avail in finding the root cause. Not only do patients experience a lot of frustration, but also often doubt themselves even though they know something is very wrong but just feel like no one believes them. Many times patients are told “It is all in your head” to only much later discover that was actually true.
The tiny pituitary gland was responsible for most of the disturbing symptoms.
Hormonal, physical and emotional shifts with pituitary conditions
People who have raised a teenager know about the highs and lows of hormonal shifts. Women during childbearing years often feel how emotions can shift dramatically at certain times of the month. And, some women during menopause feel intense mood changes. These are normal moods that are influenced by the hormonal system in the body yet can be quite frustrating and difficult not only for the person suffering but for those around them. But when something goes really awry, like a tumor that grows on or around the master gland, the effects are felt far beyond the center of the head. And the availability of hormonal evaluations is not something families are aware of until much later.
Actual outward physical changes to the patient’s body can occur as can occur with Cushing’s disease and Acromegaly. The longer it takes to accurately detect and diagnose pituitary gland diseases the more physical changes can become apparent. Extreme weight gain, changes to facial structure and shape and other external manifestations are not only signs of the illness but frightening conditions for the person affected.
Weight shaming is commonly experienced by patients who have tried early on to get help. Sometimes even physicians have reportedly told patients to “just go on a diet and lose the weight”, inferring that it is easy. Months to years can go by for patients who often blame themselves for their out-of-control bodies. Family members can also be unsupportive, even cruel. This can be due to family members who care but feel helpless and lack knowledge about the complexity of such things as weight gain causality. Months to years to decades of feeling frustration and anger with the medical system and society in general can cause some patients to withdraw socially, become clinically depressed, or even hopeless and suicidal.
In addition to outward physical changes caused by some pituitary disorders other symptoms directly and indirectly affect not only the patient but their family and other relationships as well. It has been documented that clinical depression and anxiety are common with pituitary disorders. Some patients report memory and mental confusion, anger and/or rage and even changes in a patient’s overall sense and awareness of themselves.
These and other mental health conditions are often not linked by medical or mental health professionals as possibly due to a dysfunction with that tiny but important gland. Such symptoms as mood fluctuations can make everyone in a patient’s family ill at ease, even frightened. As a result, patients and families can pull away even more from one another in an effort to protect themselves and their loved ones. A downward spiral of a lack of trust and continued isolation can lead to the fracturing of family bonds and relationship connections.
Testing Levels of Hormones for Answers to Suspected Pituitary Gland Disorder Symptoms
Testing hormone levels is important for diagnosing suspected pituitary gland disorders. Doctors begin with a comprehensive evaluation of symptoms, such as unexplained fatigue, vision problems, or hormonal imbalances affecting growth, metabolism, or reproduction. Blood tests measure various hormone levels, including thyroid-stimulating hormone (TSH), adrenocorticotropic hormone (ACTH), growth hormone (GH), prolactin, and others regulated by the pituitary gland.
Steps:
- Initial consultation to discuss symptoms and medical history
- Blood sample collection for hormone level analysis
- Imaging studies, such as MRI or CT scans, to visualize the pituitary gland
Key Hormones Tested:
- TSH: Affects thyroid function, influencing metabolism and energy levels
- ACTH: Regulates cortisol production, impacting stress response and immune function
- GH: Controls growth and development, affecting muscle and bone health
- Prolactin: Influences reproductive health, including menstrual cycles and lactation
Interpretation:
- High or low hormone levels indicate potential pituitary dysfunction
- Abnormal results may necessitate further testing or referral to an endocrinologist
Treatment:
- Hormone replacement therapy
- Medications to regulate hormone production
- Possible surgery if a tumor is detected
Regular follow-up and monitoring ensure effective management of the disorder, helping to alleviate symptoms and improve overall health.
Finding expert treatment for pituitary tumors and other pituitary disorders
This all may sound pretty dismal so far. But, there is good news. First, with excellent and highly skilled physicians, pituitary disorders are being detected much quicker and treated better than ever. Centers of Excellence have been established in order to ensure that patients are offered an entire coordinated team of experts. More information is available today, especially with the help of the internet, for patients and their families to find help and such centers. And patients and their families can repair challenged relationships that have been threatened by the effects of the tumor or other hormonal disturbance.
Individual and family therapy can certainly assist patients and their families with the challenges of navigating the diagnostic and treatment process. It is especially helpful to find a mental health professional who has training in chronic and serious illnesses. Unfortunately, few mental health professionals today have expertise or much knowledge about the specifics of pituitary disorders. Hopefully, this will change soon. So, it is important to know how to find those professionals who are open-minded to learning enough to be helpful and having a willingness to consult with endocrinologists and others as necessary.
Psychotropic medications may also be helpful and necessary, and psychiatrists can work with the endocrine system especially immediately following surgery or other pituitary treatment. The stigma of mental health is hopefully diminishing as our society recognizes the interplay of the mind and the body. As mental health becomes demystified, seen as just another way to heal and repair, then more and more patients will feel comfortable seeking assistance.
Change can be difficult
Pituitary tumors and other disorders of the neuroendocrine system can certainly bring about change: physical, mental, emotional, and behavioral. And, such changes often disrupt and change family connections and relationships. It is important to understand the illness and its potential impact on all aspects of life. It is vital for patients, their doctors, family and others to communicate about expectations for physical as well as mental health recovery. And, it is also important for all family members to be informed at all steps of the process.
Children are often seen as being too young to understand but they are highly perceptive and intuitively know when something is off in the family. So even the young ones need to know about any medical challenges a parent or other family member may face. There are tender ways to approach children and even books for even the very young to help explain medical issues. Silence and secrets never improve situations or relationships. If it seems too difficult to find words or know how to discuss such things in the family, then the help of a professional can sensitively help all involved.
Getting a proper diagnosis and medical treatment is important but pituitary disorders involve a lot more. Patients and their family are also often surprised at the mental and emotional changes that occur for a while even following medical or surgical treatment. The ups and downs of hormonal shifts until things become stabilized can be disastrous without proper expectations and the support of close family members. The family must be considered part of the treatment team, perhaps the most important since they will hopefully be there for a lifetime that follows.
The process of healing can be lengthy and certainly scary but with a skilled treatment team it doesn’t have to be a lonely path.
What are the symptoms of a malfunctioning pituitary gland?
A malfunctioning pituitary gland can cause a wide range of symptoms due to its role in regulating various hormones. Common symptoms include persistent fatigue, unexplained weight gain or loss, and headaches. Vision problems, particularly loss of peripheral vision, often arise if a tumor compresses the optic nerves. Hormonal imbalances are also prevalent, leading to symptoms such as irregular menstrual cycles, infertility, or reduced libido.
Additional symptoms:
- Growth issues: Children may experience stunted growth or gigantism, while adults might develop acromegaly.
- Thyroid dysfunction: Hypothyroidism or hyperthyroidism can result from disrupted TSH levels.
- Adrenal insufficiency: Symptoms include low blood pressure, fatigue, and electrolyte imbalances due to insufficient cortisol production.
- Prolactin imbalances: High levels cause galactorrhea (milk production not associated with childbirth) and reproductive issues.
Diagnosis and monitoring:
- Blood tests: Measure hormone levels to identify imbalances.
- Imaging studies: MRI or CT scans detect structural abnormalities.
- Consultations: Regular visits with an endocrinologist for ongoing management.
What is the most common pituitary disorder?
The most common pituitary disorder is a pituitary adenoma, which is a benign tumor that can significantly impact hormone production. These adenomas can lead to either hypersecretion or hyposecretion of hormones, resulting in various clinical syndromes.
Types of pituitary adenomas:
- Prolactinomas: Overproduce prolactin, causing symptoms such as galactorrhea (milk production not related to childbirth), irregular menstrual cycles, and infertility.
- Growth hormone-secreting adenomas: Lead to acromegaly in adults or gigantism in children, characterized by abnormal growth of bones and tissues.
- ACTH-secreting adenomas: Cause Cushing’s disease, which includes weight gain, high blood pressure, and elevated blood sugar levels (CancerInfo) (Lab Tests Online-UK).
How do you test for pituitary gland problems?
Testing for pituitary gland problems involves a series of evaluations to determine hormonal imbalances and identify any structural abnormalities. The process typically begins with a detailed medical history and a physical examination to assess symptoms like persistent headaches, vision problems, or unexplained fatigue.
Key diagnostic steps:
- Blood tests: These measure hormone levels, such as thyroid-stimulating hormone (TSH), adrenocorticotropic hormone (ACTH), growth hormone (GH), and prolactin. Abnormal levels can indicate pituitary dysfunction.
- Urine tests: Used to measure cortisol levels, especially when suspecting conditions like Cushing’s disease.
- Imaging studies: MRI or CT scans are essential for visualizing the pituitary gland and detecting tumors or other structural anomalies.
- Stimulation or suppression tests: These assess the pituitary gland’s response to various stimuli or medications. For example, the insulin tolerance test evaluates growth hormone and cortisol responses by inducing hypoglycemia.
Specialist consultations:
- Endocrinologist: Manages hormonal disorders and interprets test results.
- Ophthalmologist: Conducts vision tests if a tumor may affect the optic nerves.
Early diagnosis through these comprehensive tests allows for targeted treatment, which may include medications, surgery, or radiation therapy. Regular follow-up is crucial to monitor hormone levels and adjust treatment plans as necessary.
What is the most reliable test for pituitary function?
The most reliable test for pituitary function is the dynamic hormone stimulation or suppression test. This test evaluates the pituitary gland’s response to specific stimuli, providing detailed insights into its functionality.
Key types of dynamic tests:
- Insulin tolerance test (ITT): Assesses the pituitary’s ability to produce growth hormone (GH) and adrenocorticotropic hormone (ACTH). It involves administering insulin to induce hypoglycemia, which should trigger the release of these hormones if the pituitary gland is functioning correctly.
- Glucose tolerance test: Used primarily for diagnosing acromegaly, it measures GH levels in response to glucose intake. Normally, GH levels should drop, but they remain high in individuals with acromegaly.
- ACTH stimulation test: Evaluates adrenal function by measuring cortisol levels before and after an ACTH injection. This test is crucial for diagnosing adrenal insufficiency, often linked to pituitary disorders.
Procedure:
- Preparation: Fasting and resting are typically required.
- Administration: The test involves administering a stimulus or suppressive agent and collecting blood samples at regular intervals to measure hormone levels.
- Monitoring: Continuous monitoring is essential to observe the body’s hormonal response.
These tests provide a comprehensive evaluation of the pituitary gland’s function, guiding accurate diagnosis and effective treatment plans. Regular follow-up ensures ongoing assessment and adjustment of therapies as needed.
2125 Arizona Ave, Santa Monica, CA 90404
310-582-7450
Doctors and Surgeons Who Treat Pituitary Disorders
Our Clinics
Given the complexities of diagnosis and treatment of acromegaly, it is critical that patients seek out a Pituitary Center of Excellence and use available patient and education resources. If you or a loved has symptoms of acromegaly see your physician or contact us at the Pacific Pituitary Disorders Center.
Pacific Neuroscience Institute – Santa Monica
2125 Arizona Ave., Santa Monica, CA 90404
310-582-7450
PNI-South Bay
5215 Torrance Blvd., #300, Torrance, CA 90503
424-212-5361
PNI-Burbank
501 S Buena Vista St., Burbank, CA 91505
818-748-4999
Useful Links
- Read what patients have to say about their experience in Part 2 of this two-part blog.
- Pituitary Network Association
- AcromegalyInfo.com
- Pituitary Society
- Hormones 411