Pituitary Function: The Resilient Pituitary Gland
by Garni Barkhoudarian
Originally published October 20, 2015. Updated September 3, 2024
The Pituitary Gland, Master Endocrine Gland
The pituitary gland is considered to be the “master endocrine gland” or simply “the master gland”. It is a pea-sized structure located at the base of the brain, important in controlling growth and development and the functioning of the other endocrine glands. Hormones secreted from the pituitary gland help control growth, blood pressure, certain functions of the sex organs, thyroid glands and metabolism as well as some aspects of pregnancy, childbirth, nursing, water/salt concentration and the kidneys, temperature regulation and pain relief.
What are the main functions of the pituitary gland?
The pituitary gland consists of two lobes, the anterior and posterior, each responsible for different tasks. The anterior lobe produces several essential hormones, including growth hormone, which controls growth, and thyroid-stimulating hormone, which regulates the thyroid gland.
In addition, the pituitary gland produces hormones that affect the adrenal glands, reproductive organs, and overall metabolism. It also releases prolactin, which helps with milk production after childbirth, and luteinizing hormone, which is vital for reproductive function. Meanwhile, the posterior lobe stores and releases hormones like oxytocin and vasopressin, which control uterine contractions during childbirth and regulate water balance in the body.
The pituitary also controls the involuntary (vegetative) nervous system, influencing functions like blood pressure, digestion, and heart rate. Any disruption, such as a pituitary tumor, can impact these critical processes, leading to various symptoms.
- Main functions include:
- Regulating growth and metabolism
- Influencing thyroid and adrenal glands
- Controlling reproductive hormones
- Managing water balance and blood pressure
Removing Pituitary Gland Tumors
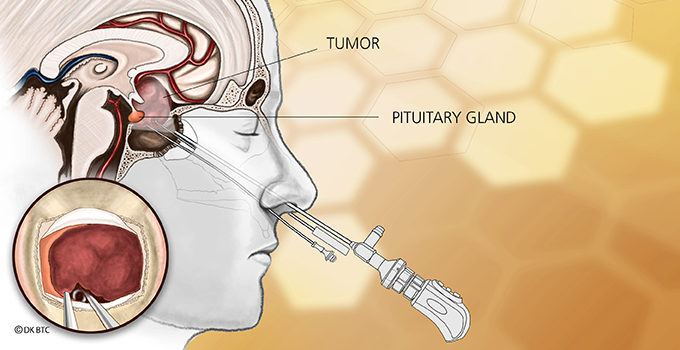
Pituitary tumors are the third most common intracranial tumor. For the majority of symptomatic pituitary adenomas, Rathke’s Cleft Cysts (RCCs) and craniopharyngiomas, transsphenoidal surgical removal (via the nose) performing endonasal endoscopic surgery is the treatment of choice.
Health Issues Due to Pituitary Gland Tumors
Given their location, tumors in and around the pituitary gland can cause significant health problems and disability including abnormal pituitary hormone over-production, hormonal underproduction (hypopituitarism), loss of vision, headaches and bleeding.
The four most common diseases caused by pituitary dysfunction are:
- Acromegaly: This occurs when the pituitary produces too much growth hormone, causing abnormal growth of bones and tissues, particularly in the hands, feet, and face. It develops slowly and may go unnoticed for years.
- Cushing’s Disease: This disorder happens when the pituitary releases excess adrenocorticotropic hormone (ACTH), leading to increased cortisol levels. Symptoms include weight gain, particularly in the face and abdomen, high blood pressure, and muscle weakness.
- Hypopituitarism: A condition where the pituitary fails to produce enough hormones, leading to deficiencies in the thyroid, adrenal glands, or reproductive hormones. Patients may experience fatigue, weight changes, and reduced libido.
- Prolactinoma: This is a benign pituitary tumor that produces excessive prolactin, causing menstrual irregularities in women, reduced testosterone in men, and infertility in both.
Considerations for Pituitary Gland Tumors
Because of their location in the brain, operating on pituitary tumors can be challenging as presenting symptoms can be quite diverse. A patient with headaches and vision loss has different goals than a patient with Cushing’s disease.
Nevertheless, the preservation of pituitary gland function is preferred, despite readily available medications to replace most of its hormones. Only a patient on life-long hormone replacement for cortisol or vasopressin (anti-diuretic hormone – ADH) can tell you the challenges of stress hormone dosing and maintenance of fluid balance. Women attempting to conceive have additional challenges when their glands are not working, often requiring the assistance of fertility specialists to prime their ovaries. So, whenever there is a concern about damaging the pituitary gland during surgery, we consider the reason seriously and think twice about the overall goals.
A primary example of this is when surgeons need to deliberately incise or resect the normal pituitary gland in order to reach pituitary tumors behind the gland. The purported concept for such a maneuver is to prevent excessive traction on the pituitary gland – and in turn, the pituitary stalk and hypothalamus. However, this theory had never been supported by data until our publication in the journal Pituitary. By analyzing our patients who had surgery for common pituitary tumors (adenomas) and cysts (372 patients over 4 years), we found that there was no significant increase in pituitary dysfunction and the rate of temporary dysfunction with ADH secretion actually decreased. Interestingly, patients who underwent hemihypophysectomies (removing half the normal gland for Cushing’s disease) had no new pituitary hormone dysfunction at all.
Though we utilize technology to improve our ability to safely remove pituitary tumors using the endoscopic endonasal approach with high definition visualization, neuronavigation and Doppler ultrasonography, the technical goals of surgery remain in-line with this philosophy.
What is the most common cause of pituitary dysfunction?
The most common cause of pituitary dysfunction is a pituitary adenoma, a benign tumor that grows in the pituitary gland, which is found in your brain. These tumors account for the majority of pituitary disorders and can interfere with the gland’s ability to produce a number of hormones that regulate other endocrine glands. Depending on their size and whether they produce excess hormones, these tumors can lead to various symptoms.
For instance, a functioning adenoma may produce too much growth hormone, resulting in conditions like acromegaly. Alternatively, non-functioning adenomas do not produce hormones but can press on surrounding structures in the brain, leading to headaches, vision changes, or hormone deficiencies by compressing the normal pituitary tissue. In either case, pituitary dysfunction occurs due to the tumor’s disruption of normal hormone production and regulation.
Other less common causes of pituitary dysfunction include traumatic brain injury, radiation treatments affecting the pituitary, or inflammation from autoimmune diseases. However, pituitary adenomas remain the primary reason for these dysfunctions.
What is the most common indicator of a pituitary tumor?
The most common indicator of a pituitary tumor is unexplained changes in hormone levels, as the pituitary gland, found in your brain, produces a number of hormones that regulate various bodily functions. Depending on whether the tumor is functioning (producing hormones) or non-functioning, symptoms can vary. For functioning tumors, an overproduction of specific hormones often leads to noticeable signs. For example, an excess of growth hormone can result in abnormal growth of hands and feet, while too much thyroid-stimulating hormone can cause hyperthyroidism, leading to weight loss, nervousness, and rapid heartbeat.
Non-functioning tumors may not produce hormones but can still cause symptoms by pressing on surrounding structures in the brain. A common indicator is vision changes, especially loss of peripheral vision, as the tumor may press on the optic nerves. Headaches, fatigue, and unexplained changes in mood or energy levels can also signal a pituitary tumor.
What are the symptoms of a malfunctioning hypothalamus?
A malfunctioning hypothalamus, which works closely with the pituitary gland, can lead to a variety of symptoms since it plays a crucial role in regulating the functions of other endocrine glands and controls the involuntary (vegetative) nervous system. The hypothalamus is found in your brain and produces hormones that influence essential processes like body temperature, hunger, thirst, sleep, and emotional behavior. When it malfunctions, these processes are disrupted.
One key symptom is abnormal body temperature regulation, leading to frequent feelings of being too hot or too cold. Another common sign involves appetite changes, with either excessive hunger or lack of interest in food. Disturbed sleep patterns, such as insomnia or excessive sleepiness, often occur as the hypothalamus affects sleep-wake cycles. Additionally, hormonal imbalances can result, affecting the thyroid, adrenal glands, or growth hormone production, causing fatigue, weight changes, or mood swings.
If your pituitary tumor affects the hypothalamus, these symptoms may be more pronounced. Early treatment can minimize symptoms and restore hormonal balance.
Clinic Locations
2125 Arizona Ave.
Santa Monica, CA 90404
310-582-7450
5215 Torrance Blvd., #300,
Torrance, CA 90503
424-212-5361
501 S Buena Vista St.,
Burbank, CA 91505
818-748-4999
Pituitary disorders specialist team at PNI
Articles related to pituitary disorders
About the Author

Garni Barkhoudarian
Dr. Garni Barkhoudarian is an expert neurosurgeon and director of the Facial Pain and Adult Hydrocephalus Centers, and Co-director of the Pituitary Disorders Center at Pacific Neuroscience Institute. His philosophy for virtually all intracranial procedures is to apply the keyhole concept of minimizing disturbance to the brain and its supporting structures.
Last updated: April 14th, 2025