15 Early Warning Signs of Multiple Sclerosis All Women Need to Know
by Guest Author
Neurologist and Multiple Sclerosis (MS) Specialist Barbara Giesser, MD, of PNI’s Pacific Brain Health Center, discusses the signs, symptoms, and treatment options for MS.
Maybe your fingers have been tingling for a few days. Or you suddenly can’t see out of your left eye. Perhaps you’re super tired and can’t figure out why. The last thing you might think these feelings could be are early signs of Multiple Sclerosis (MS). But it’s not out of the realm of possibility, especially if you’re a woman under the age of 50.
“We think there are over a million people in the United States that currently carry a diagnosis of MS and it’s three times more common in women.
Barbara S. Giesser, MD, Neurologist and MS Specialist, Pacific Brain Health Center, Pacific Neuroscience Institute
What is Multiple Sclerosis (MS)?
Multiple Sclerosis is generally believed to be an autoimmune disease. Normally, the immune system, which is composed of different types of immune cells and proteins, recognizes an individual’s body as “Self’ and protects it from outside or “non-self” entities, such as germs.
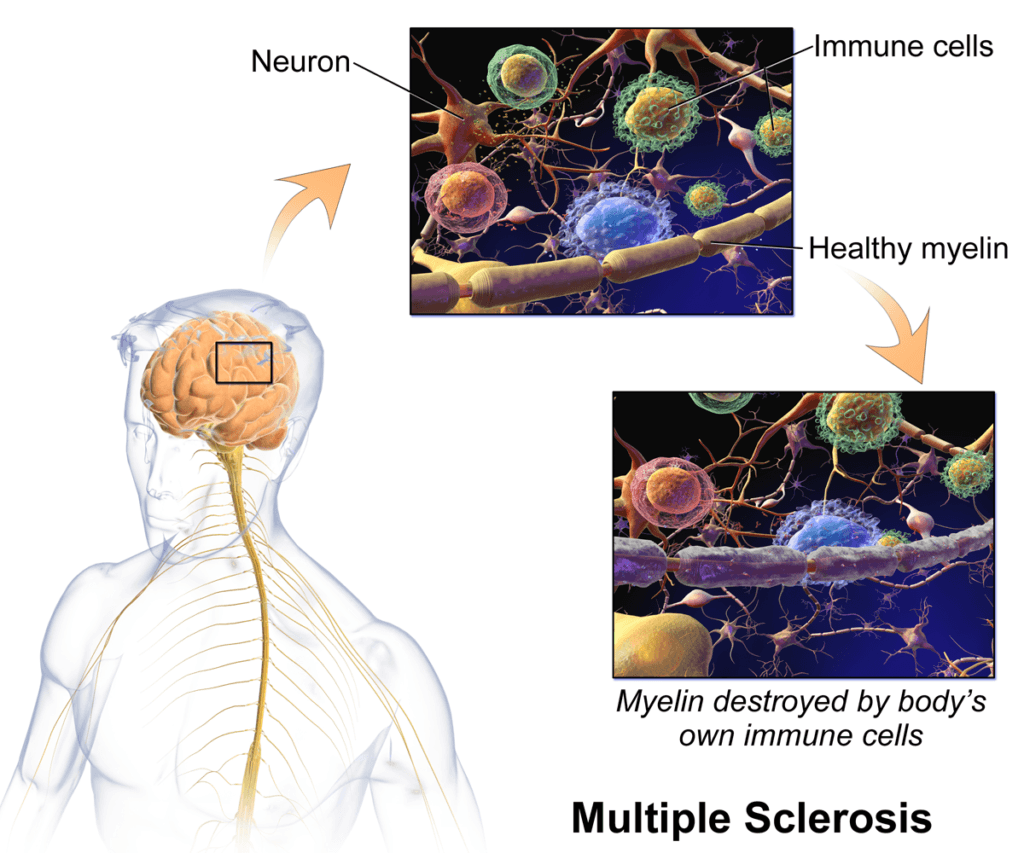
the central nervous system (also called plaques),
inflammation and the destruction of myelin sheaths of neurons.
By BruceBlaus. Own work, CC BY-SA 4.0,
The central nervous system or CNS ( brain, optic nerve, and spinal cord) usually does not allow most immune cells and proteins to enter. In MS, the immune system no longer recognizes parts of the central nervous system as “Self’ and gains the ability to get into the CNS and to attack the nerves.
Unfortunately, no one knows exactly what causes this immune system betrayal. “What we’ve thought for a while is, is that in order for somebody to develop MS, you have a combination of genetics and environment,” says Neurologist and MS Specialist Barbara Giesser, MD, at Pacific Neuroscience Institute. Potential environmental factors include the Epstein-Barr virus and low sunlight exposure (which may result in low vitamin D levels).
What are the symptoms of Multiple Sclerosis (MS)?
“MS can produce many, many symptoms because as the disease suggests, it strikes multiple parts of the nervous system,” says Dr. Giesser. “The most common form of MS — the kind that roughly 75 to 85% of people present with — is what we call relapsing-remitting.”
An official “relapse,” attack, or exacerbation is the occurrence of a new symptom or a reappearance of a previous symptom that lasts for more than 24 hours and is not due to a known cause such as a fever, infection, or being overheated. “Most relapses last days to weeks,” says Dr. Giesser. “When the symptoms subside, this is called a remission.”
MS can affect your entire body from your brain to your toes, and symptoms can vary from one person to the next, depending on what part of your central nervous system is damaged by the condition. It’s always smart to pay attention to your body and let your doctor know if anything feels off, but especially if you experience any of the neurologic symptoms detailed below, which can be signs of MS.
Here are the most common early signs to look out for:

- Fatigue: “The most common symptom of MS is actually fatigue,” says Dr. Giesser. “Obviously MS is not the only thing that causes fatigue, but fatigue is a very common symptom.” MS is primarily a disease of young women and Dr. Giesser says it’s not uncommon for a young woman to complain of being incredibly tired and their doctor shrugs it off blaming the woman’s many responsibilities (such as work and/or kids). It’s a good reminder to pay attention to your body and advocate for yourself if you’re not being taken seriously.
- Numbness or tingling: “Numbness and tingling — especially that comes and goes in the hands or feet — is a common symptom,” says Dr. Giesser. “Again, clearly MS is not the only thing that causes that.”
- Vision problems: One of the most common early symptoms of MS are visual problems. Pain, when you move your eyes, is another red flag.
- Weakness: Many people may have numbness or body weakness on one side of the body. In cases like that, sometimes MS is mistaken for a stroke, but stroke symptoms don’t come and go the way MS symptoms do.
- Muscle spasms and stiffness: Formally called spasticity, this symptom can range from mild feelings of muscle tightness to severe and painful spasms, according to the National MS Society, and it most commonly affects the legs.
- Balance problems: MS can directly impact a person’s equilibrium and ability to balance. On top of that, weakness, vision loss, and sensory issues triggered by MS can also throw you off kilter.
- Torso tightness: “Some people with MS may experience a sensation as though they have a tight band or belt around their torso,” says Dr. Giesser. “This is due to nerve damage in the thoracic spinal cord and is called the ‘MS hug.’”
- Pain: Pain can manifest in different ways. You could have painful muscle spasms, nerve pain, or even numbness and tingling that hurts.

- Change in bladder habits: Frequency, or going to the restroom a lot, is one of the most common bladder symptoms. You may experience hesitancy, where you feel like you have to go to the restroom, but don’t fully empty your bladder and need to go again.
- Sexual problems: “MS may affect sexual function in a number of ways,” says Dr. Giesser. Women may experience anorgasmia (delayed, infrequent or absent orgasms) or dyspareunia (pain with intercourse) while men may have erectile dysfunction. “Both sexes may have decreased libido, not only due to the MS, but also secondary to other symptoms such as fatigue or medication effects,” adds Dr. Giesser.
- Constipation: Yes, MS can interfere with bowel movements.
- Depression: If you’re not feeling well mentally, mention it to your doctor so they can address it as part of your treatment plan.
- Cognitive changes: The most common cognitive changes related to MS tend to be things like slowed processing (when you need to read things a few times to let them sink in), difficulty finding words, loss of short-term memory, and multitasking problems.
- Tremor: “The most common form of tremor due to MS is what is called an action tremor,” says Dr. Giesser. “The limb or hand shakes when the person tries to do something with it. Rehabilitative techniques and sometimes medications can help with this.” When MS causes increased muscle tone or spasticity, that can also lead to shaking which medication and physical therapy can help with.
- Difficulty swallowing or speaking: Sometimes MS will make it hard to swallow or talk properly. If someone has MS, they will likely have other symptoms as well (such as numbness or tingling), but it’s helpful to be aware of all the ways the condition can manifest.
When should you see a doctor?
If you experience any of the symptoms mentioned above and it either doesn’t go away or it goes away and comes back repeatedly, see your primary care doctor. They should refer you to a neurologist for a more in-depth evaluation. Remember, MS can be diagnosed in otherwise-healthy people so don’t just dismiss your symptoms and assume they’ll go away on their own.
“As with almost any disease, certainly with MS, we do want to find out about it early because we can treat it,” adds Dr. Giesser, who notes that MS damage accumulates in the majority of people who have the disease but aren’t treated for it.
How is Multiple Sclerosis (MS) diagnosed?
“It would be nice if we had something for MS that was definitively negative or positive like a pregnancy test,” says Dr. Giesser. Alas, that’s not the case. “We don’t have a surefire test — what we call a pathognomonic test — so we have rules,” says Dr. Giesser. These are the rules that must be met for a diagnosis of multiple sclerosis:

- There must be objective evidence of damage in more than one area of the central nervous system (hence the term “multiple”).
- “There used to be a rule that you had to have more than one episode — what we call dissemination or multiplicity in time or space — more than one spot and more than one attack,” says Dr. Giesser. “We have some updated criteria which say even if somebody’s only had one attack, if they show simultaneously inflamed and non-inflamed spots on an MRI or if they have certain abnormalities in their spinal fluid, that counts for having a second attack.”
- Other reasonable diagnoses must be ruled out.
There isn’t a single test that will tell you if you have MS, but there are blood tests that can pinpoint other conditions or vitamin deficiencies, explained Dr. Giesser. Additionally, you’ll likely get an MRI of the brain and/or spine to look for internal signs of MS.
How is Multiple Sclerosis (MS) treated?
“The reason it’s important to go see a doctor is that this is a very, very treatable condition,” says Dr. Giesser. Disease-modifying medication combined with exercise, following a healthy diet, and not smoking can help to control multiple sclerosis. Some of these treatments can actually slow the progression of MS and prevent future damage.
Who gets Multiple Sclerosis (MS)?
Most people are between age 20 and 50 when symptoms start, although MS can affect folks who are older or younger than that.
Does Multiple Sclerosis (MS) affect fertility?
“MS does not affect or interfere with a woman’s ability to conceive,” says Dr. Giesser. “In fact, during pregnancy, women with MS are relatively protected.” That’s because a baby gets half of its genetic material from its father — an organism that is separate and different from the mother.

“Normally the immune system would think part of this thing growing inside the woman is foreign and it would attack it,” explains Dr. Giesser. “But in all women, our immune systems are turned down when we’re pregnant so this actually turns out to be a good thing for women with MS.” Since MS is an autoimmune condition, women tend to experience a respite from MS exacerbations during pregnancy because their immune systems are directed to stand down.
Does Multiple Sclerosis (MS) affect menstruation?
“MS does not interfere with people’s menstrual cycle, but some women will notice symptom variation during their cycle,” says Dr. Giesser. For instance, some research has found that women with MS may experience a worsening of MS symptoms right before their periods.
Original article written by Kaitlyn Pirie for Good Housekeeping.
About Dr. Barbara Giesser

Dr. Barbara S. Giesser, FAAN, FANA, is an internationally recognized clinician and award-winning educator who has specialized in the care of persons with Multiple Sclerosis since 1982. Dr. Giesser’s approach to the diagnosis & management of persons with MS combines state-of-the-art diagnostics and a personalized medication plan for each patient with an emphasis on integrating lifestyle and wellness strategies into the neurologic treatment plan.
Related Links:
- Pacific Brain Health Center
- Multiple Sclerosis | 310-582-7613
- MS Treatment & Care Sheet
- Q&A with the American Neurological Association
- Pacific Brain Health Center
Videos about Multiple Sclerosis (MS)
Last updated: November 7th, 2022