

PHYSICIAN SPOTLIGHT: Dr. Chester Griffiths’ Legacy of Care
by Zara Jethani
Dr. Chester Griffiths has a knack for making people feel at ease right away. His easy-going manner and friendly disposition complement his considerable surgical experience and expertise. Along with Dr. Daniel Kelly at the Pacific Neuroscience Institute, he is co-surgeon in endoscopic endonasal pituitary and skull base surgeries, and provides post-operative sinus care to patients at the Pacific Brain Tumor and Pacific Pituitary Disorders Centers.
Rated among the top ENT surgeons in Los Angeles, Dr. Griffiths’ private practice focuses on treatment of facial and nasal trauma, cosmetic deformities, sinus infections, and disorders of smell and taste. He is the official team maxillofacial plastic surgeon for the Los Angeles Kings and is a long-time volunteer with the Venice Family Clinic where he received the Irma Cohen Leadership Award in 2012 in recognition of his services.
The following interview is adapted from an April 2016 article by the Pituitary Network Association (PNA).
Chester F. Griffiths, MD, FACS, is a professor of surgery at the Saint John’s Cancer Institute in Santa Monica, California and is chief of endoscopic sinonasal and skull base surgery at the Pacific Brain Tumor Center at Providence Saint John’s Health Center. He was born in New York City and attended medical school at Thomas Jefferson University in Philadelphia, where he went on to complete a residency in general surgery and otolaryngology-head and neck surgery. Double board certified in Otolaryngology-Head and Neck Surgery and Facial Plastic and Reconstructive Surgery, Dr. Griffiths is an Assistant Clinical Professor at Geffen School of Medicine at UCLA.
PNA: What inspired you to choose your career path?
CG: My father, Dr. Cadvan Owen Griffiths Jr, is a great inspiration, mentor and friend to me. He is a renaissance man with accomplishments beyond medicine and surgery as a lawyer, screenwriter, Naval flight surgeon, Korean War Veteran with the U.S. Marine Corps and a philanthropist supporting plastic surgery clinics at the Christian College of Vellore in India.
 As a researcher, he had a bench lab at Columbia University and the Rockefeller Institute in New York, where he participated in early cancer immunologic research. He was co-research developer of Rho-D immune globulin (RHO-GAM) to prevent erythroblastosis fetalis (a hemolytic disease of newborns). He was particularly interested in homograft stimulation of the immune system in cancer patients. He was an early pioneer in breast reconstruction, having published submuscular implantation of silicone breast implants for both immediate cancer reconstruction and for cosmetic enhancement in the mid 1960’s, contrary to the practice norm of radical mastectomy as the definitive treatment for breast cancer. With his example, I have been inspired to continue in his footsteps.
As a researcher, he had a bench lab at Columbia University and the Rockefeller Institute in New York, where he participated in early cancer immunologic research. He was co-research developer of Rho-D immune globulin (RHO-GAM) to prevent erythroblastosis fetalis (a hemolytic disease of newborns). He was particularly interested in homograft stimulation of the immune system in cancer patients. He was an early pioneer in breast reconstruction, having published submuscular implantation of silicone breast implants for both immediate cancer reconstruction and for cosmetic enhancement in the mid 1960’s, contrary to the practice norm of radical mastectomy as the definitive treatment for breast cancer. With his example, I have been inspired to continue in his footsteps.
Why did you devote your career to cancer research?
I suffered from an undiagnosed aliment as a child and was treated by the doctors of Providence Saint John’s for 3 years between the ages of 6 and 9. Although a diagnosis was never made, I did recover and decided that I would become a physician to care for those in need. To fulfill that promise, I was licensed to practice medicine by the age of 21. The physicians and nurses who cared for me during those difficult times made a lasting impact on me and were the catalyst for my desire to become a physician.
What is the focus of your current research and/or practice?
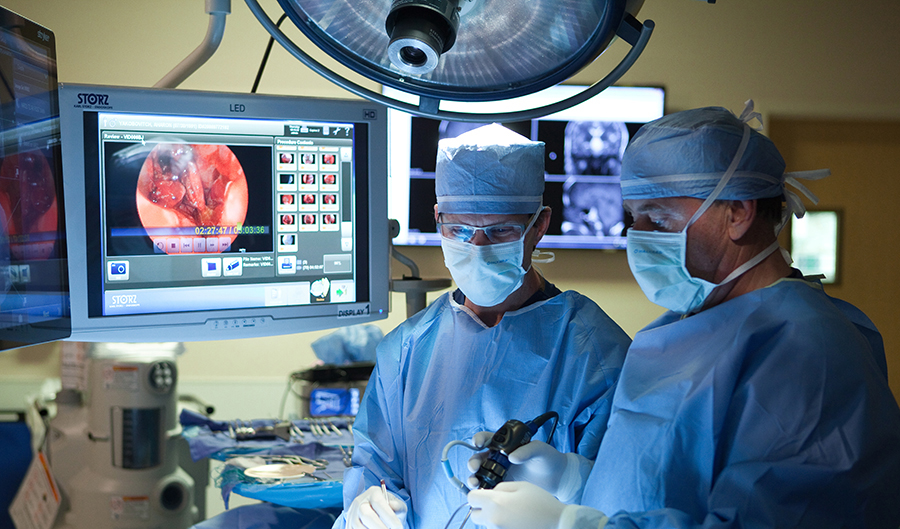
1. Study and practice of the anatomic basis of minimally invasive endoscopic endonasal skull base tumor removal with Dr. Garni Barkhoudarian and Dr. Daniel Kelly. In collaboration with Dr. Howard Krauss, neuro-ophthalmologist, we were the first to successfully remove an orbital (eye) apex tumor through the nose utilizing endoscopic techniques in 2001. Since that time, we have utilized these techniques on many patients.
2. Preservation of olfactory function (smell) following nasal-skull base surgery.
3. Assessment of viral impact on the development of head and neck cancer, principally that of Human Papilloma Virus.
4. Packing-less nasal surgical procedures.
5. Centers of Excellence development with emphasis on expertise team building, financial efficiency and patient clinical outcome data analysis.
What brought you to Saint John’s Cancer Institute?
 Dr. Kelly and I collaborated together at UCLA, developing techniques of minimally invasive endoscopic endonasal skull base surgery prior to his joining Saint John’s Cancer Institute. We have continued this innovative collaboration at the Pacific Brain Tumor Center at the Pacific Neuroscience Institute where have performed more than 300 such excisions of skull base brain tumors. I currently hold a faculty position at the Institute as a Professor of Surgery for the neurosurgical fellowship training program.
Dr. Kelly and I collaborated together at UCLA, developing techniques of minimally invasive endoscopic endonasal skull base surgery prior to his joining Saint John’s Cancer Institute. We have continued this innovative collaboration at the Pacific Brain Tumor Center at the Pacific Neuroscience Institute where have performed more than 300 such excisions of skull base brain tumors. I currently hold a faculty position at the Institute as a Professor of Surgery for the neurosurgical fellowship training program.
Tell us about your volunteer work.
Aside from my clinical, teaching and research endeavors, I am on the Board of Directors of the Venice Family Clinic, the largest free clinic in America, treating over 106,000 patient visits a year at 10 clinic locations. I have been treating the patients (children and adults) of the clinic for 23 years for aliments involving the ear, nose and throat. Providence Saint John’s has been a strong supporter of the Venice Family Clinic, donating in-kind services for more than 40 years.
 In addition to medically treating the Venice Family Clinic patients, I and my associate, Dr. Kian Karimi, perform surgical procedures in our operating room at Pacific Eye and Ear Specialists. My colleague, Dr Gregory Frazer, offers free hearing aids to hard-of-hearing patients and Dr. Howard Krauss and Dr. Jeremy Levenson provide vision and eye care. I am so proud to be part of a committed, selfless group of volunteers, corporate and community members, and physicians who believe that it is important to care for those in need. This is truly unique.
In addition to medically treating the Venice Family Clinic patients, I and my associate, Dr. Kian Karimi, perform surgical procedures in our operating room at Pacific Eye and Ear Specialists. My colleague, Dr Gregory Frazer, offers free hearing aids to hard-of-hearing patients and Dr. Howard Krauss and Dr. Jeremy Levenson provide vision and eye care. I am so proud to be part of a committed, selfless group of volunteers, corporate and community members, and physicians who believe that it is important to care for those in need. This is truly unique.
Although research is a very important mission of a physician-scientist, treating all members of our community trumps that mission as the primary purpose of being a physician. I am very grateful for the healthcare community on the Westside and the philanthropic support from donors. They provide a great example of compassionate caring with attention to scientific breakthroughs for the benefit of our citizens.
What do you see as the future of your field?
I believe that stem cell application in regenerative therapeutics and molecular genomic-driven targeted therapies are the forefront of medical discovery. Along with the collaborative energy of neuro-oncologist, Dr. Santosh Kesari, Drs. Kelly, Krauss and I created the Pacific Neuroscience Institute (PNI). The evolution of treatment for patients at PNI is the driver of innovation and discovery. Compassion and care are the first hallmark of our mission, followed by dedication to study, discovery and innovation.
Why are you involved with the PNA?
As an associate of Dr. Kelly, it was a natural to become a supporter of the PNA. I appreciate the PNA’s dedication to raising public awareness of pituitary disorders.
Dr. Griffiths is the director of the Pacific Eye, Ear and Skull Base Center. To schedule a consultation, please contact his office.
About the Author

Zara Jethani
Zara is the marketing director at Pacific Neuroscience Institute. Her background is in molecular genetics research and healthcare marketing. In addition, she is a graphic designer with more than 20 years experience in the healthcare, education and entertainment industries.
Last updated: July 29th, 2020