

The Pituitary Tumor That Changed A Life: Cushing’s Disease
by Guest Author
A former patient joins forces with the Pacific Pituitary Disorders Center to bring awareness to Cushing’s disease and other pituitary tumor-related syndromes.
More than 25 years ago, Sharmyn McGraw began having problems with her pituitary gland, though she didn’t know it—and remarkably—neither did her doctors. Throughout her 20s, McGraw was trim, fit and muscular; she wore a size 2. But at 31 she began gaining weight.
The downward spiral
When she put on 15 pounds in three weeks, she went to a doctor who told her it was normal for people to gain weight as they aged. Although she trained with a personal fitness trainer and worked out five days a week, the doctors simply recommended diet and exercise.
McGraw hit the treadmill, pounded the pavement and dieted. However, the weight continued to pile on. At one point she ate only chicken and broccoli for breakfast and dinner and an undressed salad for lunch.
She continued to gain: 85 pounds in six months— as much as 11 pounds in four days—until finally by the end of a year she’d gained more than 100 pounds. Her long, blond hair began falling out in clumps. She had a moon face covered with a red rash and a buffalo hump lodged at the back of her neck.
McGraw sank into despair as doctor after doctor failed to diagnose the problem. She was ashamed about having to wear maternity clothes. She felt angry and frustrated by the doctors, especially by the one who told her, “I bet if we locked you in a closet with nothing but water, you’d lose weight.”
She burst into tears in the supermarket after seeing the shock on the face of a friend she hadn’t seen for a while.

Ultimately McGraw diagnosed herself and eventually she was steered to endocrinologists who confirmed the diagnosis of an ACTH-secreting pituitary adenoma (a benign tumor on the pituitary gland), which causes excessive production of the adrenal hormone cortisol and resulted in Cushing’s disease and all her related symptoms. Finally, on the recommendation of an acquaintance, she was referred to neurosurgeon Daniel F. Kelly, MD, who is founder and director of Pacific Neuroscience Institute (PNI), the Brain Tumor Center and the Pituitary Disorders Center at Providence Saint John’s Health Center.
In April 2000, McGraw underwent pituitary tumor surgery, where Dr. Kelly removed the tiny, difficult tumor through her nostrils, using a minimally invasive endonasal microscopic surgical approach, and helped McGraw regain her health and quality of life. At that time, Dr. Kelly and most other pituitary surgeons around the world had not transitioned to the fully endoscopic approach that he now uses.
How common are pituitary tumors?
More common than most people think. Pituitary tumors (also known as pituitary adenomas) are the third most common brain tumor. About 10,000 are diagnosed each year in the United States, according to the American Cancer Society. Very few are cancers although a significant minority behave aggressively and invade the surrounding skull base area below the brain, making a cure challenging.
The pituitary gland function is a mystery to most people, Dr. Kelly says, explaining that as the “master gland” it’s responsible for coordinating all the body’s hormonal functions. Situated in a critical spot at the base of the brain, the pea-sized gland is close to the optic nerves and tucked between the paired carotid arteries.
Symptoms of pituitary tumors can include the release of too many or too few hormones, nausea, weakness, sexual dysfunction and unexplained weight gain or loss. While those are a few common symptoms, the pituitary gland, which is less than 1 centimeter in size, is complex. Many small tumors require hormonal testing to confirm the diagnosis. However, many larger pituitary tumors are diagnosed because of worsening headaches or vision loss as the tumor expands and compresses the surrounding structures of the skull base and encroaches on the optic nerves.
“It’s very common for someone with Cushing’s disease to go undiagnosed or perhaps never diagnosed for many years because no one thinks to measure their cortisol and ACTH production,” Dr. Kelly says. “Sharmyn’s case was unfortunately quite typical of someone who, in retrospect, had all the signs and symptoms of Cushing’s disease for years—going from skinny to quite heavy from excess cortisol and ACTH in her body. Fortunately, we were able to find her pituitary tumor and remove it completely.”

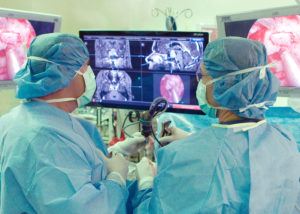
The great majority of symptomatic pituitary adenomas require surgical removal. The goal of surgery is always safe removal with preservation of the normal pituitary gland. At PNI, based on years of published data, neurosurgeons are able to preserve or restore gland function in approximately 95 percent of cases. Nearly all surgeries are done with a highly experienced neurosurgical and ENT team working together with a high-definition endoscope through both nasal passages, micro-instruments, surgical navigation (which is like GPS for the brain) and Doppler ultrasound to precisely locate the carotid arteries. In McGraw’s case, almost 20 years ago, Dr. Kelly was able to remove the tumor through the nose using an older microscopic approach without navigation or the Doppler, which make the surgery today even more accurate and safe.
Dr. Kelly describes these technologies as “game changers over the last 15 to 20 years in pituitary and skull base surgery.” Some tumors may also require medication or radiation.
Leading expertise under one roof
The benefit of the Pacific Pituitary Disorders Center is that it offers one-stop shopping with world-renowned endocrinologists, ENT surgeons, neurosurgeons, neuro- ophthalmologists and other specialists all in one place. The center provides comprehensive care to patients with all types of pituitary disorders using a multidisciplinary approach that tailors a treatment plan to each individual’s specific needs.
“We’re considered one of the leading centers in the world for managing pituitary disorders,” says Dr. Kelly, who himself has operated on more than 2,000 pituitary tumors in his 25 years of practice. “We are always striving to advance expertise in this area through research, fellowship training, as well as hands-on courses and symposia in endoscopic and keyhole surgical techniques.”
Just this year, Dr. Kelly and his colleagues published a landmark study on their experience with more than 500 patients in the Journal of Neurosurgery on repair of cerebrospinal fluid leaks, which are one of the most common post-operative complications of this type of surgery.
The center is also home to the longest-running support group in the country for people with pituitary tumors. McGraw started the support group under the direction of Dr. Kelly in 2001—a year after her surgery.
Cushing’s disease was life-changing
Adding 100 pounds to her small frame in a culture that prizes thinness gave McGraw a chance to think about what life is really about. That led her to turn one of the most devastating experiences of her life into a blessing. Out of her illness, she developed a passion to educate and help people in the same situation, with Dr. Kelly as a teammate.
“I was mistreated in an environment that was supposed to help me. Many medical professionals, as well as the public, lack education about the subject,” McGraw explains. “I had to use my platform to change how people are being diagnosed and treated.”
Today the 56-year-old salesperson from Newport Beach continues to lead the Pituitary Disorders Patient Support Group and serves as a patient advocate worldwide for those affected by a pituitary disorder. People from as far as Australia and India tune into the live-streamed support group and mini-seminar sessions that are held several times a year. “Sharmyn has been so instrumental to so many patients around the globe over the last 19 years since she started our pituitary support group,” Dr. Kelly says. “Her infectious enthusiasm, sunny outlook and focus on education and empowerment is always uplifting and helpful to patients, many of whom are really struggling with their pituitary and hormonal health issues. Her broader efforts nationally and internationally, through her website, social media and emails, have also been tremendously beneficial for pituitary patients around the globe, helping them get the information they need and finding the right specialists. She is indeed a force of nature, and we are so thankful for what she has done and continues to do.”
Facing Cushing’s disease has also helped McGraw make another transition by encouraging her to become a spokesperson for the disorder. Growing up dyslexic and humiliated by her lack of spelling and grammar skills, she once “wouldn’t even write a Post-it note.” Now she’s a published author. Her writing career began when Women’s Day published her story and continues through a wide range of other publications and television appearances. She’s also working on a mystery book series, which she hopes to dedicate to pituitary disorders.
“Cushing’s disease has turned out to be a blessing—the doctors and the patients are the best part of my life,” she says. “I wouldn’t change it because of all the wonderful things that have come out of it for myself and for so many patients.”
As to the team at PNI, McGraw says, “There’s no one better. These doctors care about their patients. That’s what is important and why I love working with my friends at PNI. That’s why I wish every patient could see doctors like the team here. They set the bar really high.”
Pituitary Disorders Patient Support Group
Taking care of the whole patient and family members is what McGraw and her guest speakers do best. The free pituitary disorders patient support group provides education, support and empowerment for those dealing with challenges of pituitary tumors. For more information on the meeting dates and times contact Sharmyn McGraw at 888-410-3334 or pituitarybuddy@hotmail.com.
THE PACIFIC PITUITARY DISORDERS CENTER
About 10,000 Americans each year are diagnosed with pituitary tumors. The physicians at the Pacific Pituitary Disorders Center are among the most experienced in the world at endoscopic endonasal surgery for pituitary tumors. In addition, the team has advanced the care of patients with pituitary disorders with major publications, courses and symposiums.
The center treats many pituitary conditions including:
– Pituitary adenoma
– Craniopharyngioma
– Rathke’s cleft cyst
– Other related tumors and cysts, such as chordomas and meningiomas
– Pituitary failure
– Pituitary inflammation
– Cerebrospinal fluid leakFor more information about the Pacific Pituitary Disorders Center, contact the clinic at 310-582-7540 or schedule a consultation at PacificPituitary.org.
Adapted from the article by NANCY BRANDS WARD / photographed by KRISTIN ANDERSON in the Spring 2019 issue of Saint John’s Magazine.
Last updated: April 3rd, 2019