

What You Should Know About Stroke and Aneurysm Treatment
by Zara Jethani
When a stroke strikes
Blood vessels that supply blood to the brain can sometimes become damaged over time leading to what is called cerebrovascular disease. The artery walls become thickened, blood flow is more difficult and most commonly this leads to ischemic stroke (also referred to just as stroke), TIA (transient ischemic attack, mini-stroke) or hemorrhagic stroke.
All three conditions can be life threatening where stroke and mini-strokes are caused by blood clots and hemorrhagic strokes are the result of a burst blood vessel that pours blood into the brain.
Any of these conditions is an emergency and a patient should be rushed to the ER for immediate treatment.
“Time is Brain”
You may have heard the phrase “Time is Brain”. What it means is that for every minute in which a stroke is untreated, the average patient loses almost 2 million neurons.
That’s a huge amount of brainpower that can never be replaced.
Stroke is the 5th cause of death and a leading cause of disability in the United States so in order to avoid its complications and achieve good outcomes, a stroke should be treated right away. Lingering effects of stroke included paralysis, difficulty speaking and impaired cognitive function.
Stroke team to the rescue
A stroke or vascular neurologist is the first person to respond to the emergency and is responsible for the diagnosis, imaging and management of the patient. At Pacific Stroke & Aneurysm Center, vascular and interventional neurologist and director of the center Dr. Jason Tarpley, administers non-surgical treatments such as clot-busting drugs, for example tPA. Typically, the stoke neurologist works in collaboration with an endovascular neurosurgeon (also called an interventional neuroradiologist or neurointerventional radiologist) who uses real-time radiological imagery and catheters to further treat the patient as necessary.
Since late 2014, the use of Endovascular Therapy (EVT) has increased significantly with very good results. Using minimally invasive techniques, regional director of neurointerventional surgery for Providence, California, Dr. George Teitelbaum or expert interventional neuroradiologist, Dr. Samuel Hou can perform a thrombectomy (removal of a blood clot). A skinny tube called a microcatheter is threaded through arteries from other parts of the body such as the groin or arm to the blood clot in the brain. A fine wire with a clot-capturing cage at its end is threaded through the catheter and the endovascular surgeon deploys this stent retriever to remove the blood clot by pulling it back through the catheter. The tube is removed and the patient’s blood flow is restored.
What if it’s a hemorrhagic stroke?
In most cases hemorrhagic stroke is caused by high blood pressure. Medications to control this are administered and the patient is assessed for surgery. Sometimes a small swelling in the blood vessel called an aneurysm bursts in which case surgery is recommended.
Aneurysm is an emergency
In general aneurysms are only detected after they have burst although they may sometimes be detected during the course of other tests.
Operating on the arteries of the brain may feel scary but there have been tremendous advances in the way that aneurysms are surgically treated. The interventional neuroradiologist has several options for treating the aneurysm from the inside of the blood vessel based on the patient’s status. These kinds of surgery, called endovascular neurosurgery or embolization, are performed using the minimally invasive microcatheter-based approach mentioned earlier. In this way, aneurysms can be treated by coiling, stent coiling, flow diversion, or balloon remodeling. In all these methods, the aim is to prevent blood from pooling in the aneurysm and causing blood clots. The deposited wire coils or cages help to cut off the blood’s access to the aneurysm so that it can flow normally through the blood vessel.
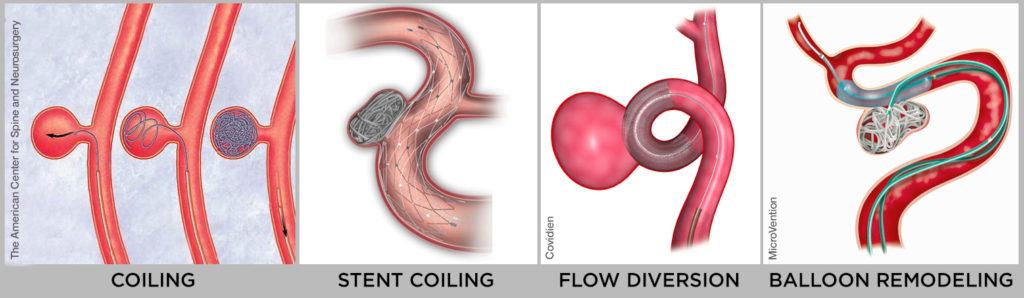
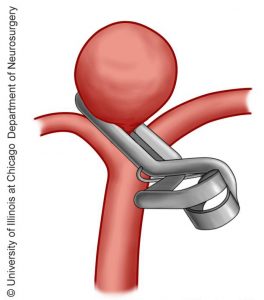
In some cases, the best approach may be to put a clip around the outside of the aneurysm’s neck. A vascular neurosurgeon performs minimally invasive microsurgery using an operating microscope. Dr. Achal Singh Achrol places a specialized metal clip around the aneurysm to completely isolate it from blood flow in order to protect against the risk of future rupture.
Advances in stroke and aneurysm treatment
Continuing research and technological advances in the fields of stroke and aneurysm treatment provide insight into what we know about these diseases and how we can improve treating them. Our doctors ongoingly participate in conferences and clinical trials to expand what they can offer patients.
At the 2017 annual International Stroke Conference, one of the big pieces of news was that in certain instances, patients can have a thrombectomy up to 6 hours after an ischemic stroke and still achieve significant benefit from EVT. Dr. Tarpley’s research showed that patients treated at a comprehensive stroke center such as ours are much more likely to succeed than those first taken to a stroke center without thrombectomy capability and then transferred.
In addition, results from the DAWN thrombectomy trial showed that benefits of EVT can be seen in a greater number of patients namely late-window and wake-up stroke patients. The study showed that 1 in 2.8 patients treated with the Trevo Retriever device to remove blood clots within 24 hours of a stroke was saved from severe disability.
Patient support leads to better outcomes
Patients report that they find it beneficial to receive ongoing information and support from medical professionals dedicated to stroke recovery and care. Patients and their families are able to interact with each other as well as learn about ways to move forward from their stroke at our free monthly patient support group meetings.
For more information, please visit the pacificstroke.org or contact one of our specialists at 310-829-8319 or stroke.center@providence.org.
Related article:
Reversing the Effects of Stroke: Clinical trial for ischemic stroke

Zara Jethani, MS, MBA, is the marketing director for the Pacific Neuroscience Institute. Her background is in graphic design, molecular genetics research and healthcare marketing.
About the Author

Zara Jethani
Zara is the marketing director at Pacific Neuroscience Institute. Her background is in molecular genetics research and healthcare marketing. In addition, she is a graphic designer with more than 20 years experience in the healthcare, education and entertainment industries.
Last updated: July 11th, 2025