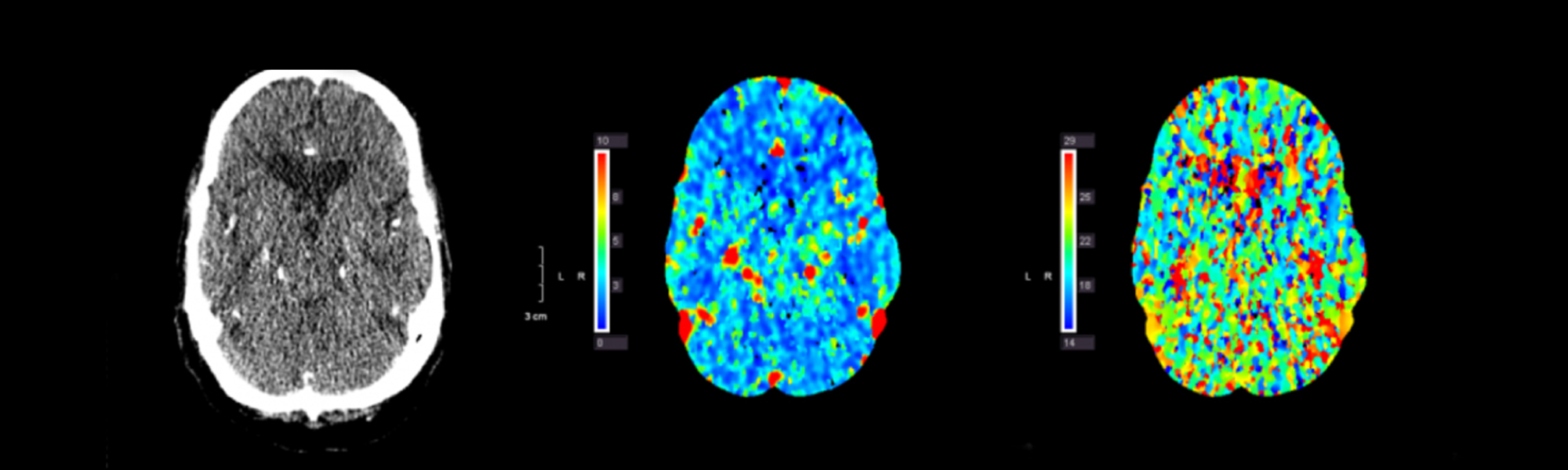
Dural arteriovenous fistula (DAVF)
Dural arteriovenous fistula (DAVF) is a rare vascular condition where abnormal connections (fistulas) are made between branches of arteries and veins in the brain covering (dura mater).
The dural arteries bring high pressure oxygen-rich blood to the brain and the dural veins take the oxygen-depleted (deoxygenated) low pressure blood back to the heart. A DAVF causes the high-pressure arterial blood to enter into the veins or sinuses that normally handle low-pressure blood returning to the heart. This can result in ruptures leading to bleeding and brain hemorrhage as well as other neurological issues.
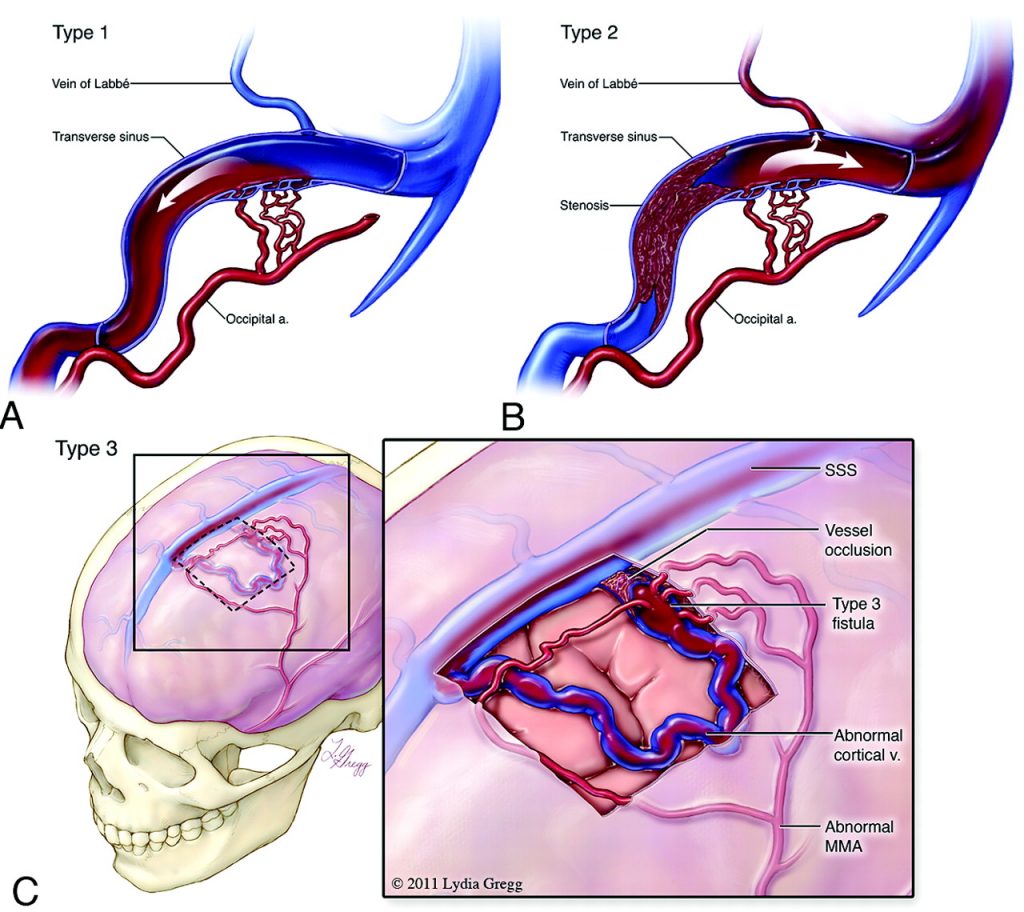
Symptoms
Patients with DAVFs may be completely asymptomatic. Symptoms, when present, may range from mild symptoms to severe hemorrhage. The symptoms depend on the location and drainage pattern of the DAVF. Neurological symptoms include:
- Bruit (sound heard due to unusual blood flow)
- Headache
- Pulsatile tinnitus (ringing in the ears)
- Visual difficulty
- Seizures
Diagnosis
Diagnosis is typically made by imaging using CT, CT angiography (CTA), MRI, or angiography. In general, DAVFs appear in both men and women in their 50’s to 60’s with hemorrhage due to DAVF being more common in men. It is unclear why DAVFs develop although there is a correlation with trauma, surgery, tumors and infection.
Treatment
First line treatment options include the use of endovascular surgical techniques and depends on the drainage pattern of the DAVF and the patient’s symptoms. Endovascular embolization is a minimally invasive procedure commonly used to treat dural arteriovenous fistulas. A catheter is threaded through an artery in the groin up to the DAVF and the fistula is sealed off using glue, a metal coil, or a balloon thus stabilizing the blood flow.
In some cases, stent placement using a microsurgical approach may be used in combination with embolization.
Contact Us
The Pacific Stroke and Neurovascular Center’s state-of-the-art facilities are located at:
Providence Saint John’s Health Center
2125 Arizona Ave., Santa Monica, CA 90404
310-829-8319
Providence Little Company of Mary Medical Center Torrance
4201 Torrance Blvd., Suite 520, Torrance, CA 90503
424-212-5340
Providence Saint Joseph Medical Center
501 S. Buena Vista Ave., Burbank, CA 90505
818-847-6049
Providence Holy Cross Medical Center
15031 Rinaldi St, Mission Hills, CA 91345
818-847-6570