Dural Arteriovenous Fistula
What is a Dural Arteriovenous Fistula?
Overview
A dural arteriovenous fistula (DAVF) is a rare vascular condition where abnormal connections (fistulas) are made between branches of arteries and veins in the brain covering (dura mater).
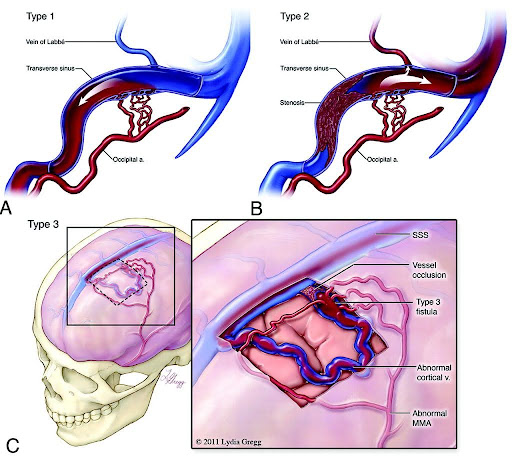
The dural arteries bring high pressure oxygen-rich blood to the brain and the dural veins take the oxygen-depleted (deoxygenated) low pressure blood back to the heart. A DAVF causes the high-pressure arterial blood to enter into the veins or sinuses that normally handle low-pressure blood returning to the heart. This can result in ruptures leading to bleeding and brain hemorrhage as well as other neurological issues.
Who is Affected?
In general, DAVFs appear in both men and women in their 50’s to 60’s with hemorrhage due to DAVF being more common in men. It is unclear why DAVFs develop although there is a correlation with trauma, surgery, tumors and infection.
Dural Arteriovenous Fistula Symptomsrn& Causes
Symptoms
Patients with DAVFs may be completely asymptomatic. Symptoms, when present, may range from mild symptoms to severe hemorrhage. The symptoms depend on the location and drainage pattern of the DAVF. Common neurological symptoms include:
- Bruit: An audible whooshing sound due to abnormal turbulent blood flow near the skull, sometimes heard by the patient or a physician with a stethoscope.
- Headache: Often persistent and sometimes severe.
- Pulsatile tinnitus: A rhythmic whooshing or ringing in the ears synchronized with the heartbeat.
- Visual disturbances: Blurred vision, double vision, or other visual impairments.
- Seizures: Sudden abnormal electrical activity in the brain.
- Neurological deficits: Weakness, numbness, or difficulties with speech, depending on location and complications such as hemorrhage or venous congestion.
Causes
DAVFs can develop spontaneously or secondary to:
- Trauma or head injury
- Prior neurosurgical procedures
- Tumors involving the dura
- Infections causing dural inflammation
- Venous sinus thrombosis, which disrupts normal venous drainage and may promote fistula formation
The exact pathophysiological mechanism of DAVFs is thought to involve abnormal angiogenesis and remodeling in response to venous hypertension or injury.
When to See a Doctor
Early diagnosis and treatment are essential to prevent serious complications such as brain hemorrhage or permanent neurological damage. Seek immediate medical attention if you experience any of the following:
- Sudden, severe headache often described as “thunderclap” headache.
- New or worsening neurological symptoms such as weakness, numbness, vision changes, or difficulty speaking.
- Pulsatile tinnitus or hearing a whooshing sound in the ears.
- Seizures.
Dural Arteriovenous Fistula Diagnosis
DAVF is typically diagnosed with advanced imaging techniques. Initial evaluation may include:
CT Scan or MRI
CT (Computed Tomography) scan or MRI (Magnetic Resonance Imaging) to detect brain abnormalities, hemorrhage, or venous congestion.
CTA or MRA
CT Angiography (CTA) or MR Angiography (MRA) to visualize blood vessels and identify abnormal connections.
Digital Subtraction Angiography (DSA)
The gold standard for diagnosing DAVF, providing detailed images of the vascular anatomy and blood flow patterns essential for treatment planning.
Additional blood tests or neurological evaluations may be performed to assess the patient’s overall condition and rule out other causes.
Dural Arteriovenous Fistula Treatmentrn& Outcomes
Treatment Options
Treatment choice depends on the DAVF’s location, drainage pattern, symptoms, and patient health. The primary goal is to eliminate abnormal blood flow and prevent complications. Early treatment greatly reduces the risk of hemorrhage and neurological decline. Options include:
Endovascular Embolization
This is a minimally invasive procedure commonly used to treat dural arteriovenous fistulas. A catheter is threaded through an artery in the groin up to the DAVF and the fistula is sealed off using glue, a metal coil, or a balloon thus stabilizing the blood flow.
Microsurgical Intervention
In cases where embolization is insufficient or inaccessible, open surgery may be performed to disconnect the fistula or decompress affected veins.
Combination Therapy
In some cases, stent placement using a microsurgical approach may be used in combination with embolization.
Radiosurgery
Targeted radiation may be used for small or difficult-to-access fistulas, though its effects take months to years.
Patient Outcomes
With appropriate treatment, many patients achieve complete closure of the DAVF and symptom resolution. Outcomes depend on factors such as fistula complexity, presence of brain injury, and timing of intervention. Delays in diagnosis or treatment increase the risk of hemorrhage, stroke, and permanent neurological damage. Close follow-up with imaging and clinical assessment is essential to detect any recurrence.
Managing A Dural Arteriovenous Fistula
- Follow your treatment and follow-up schedule closely.
- Report any new or worsening symptoms immediately.
- Manage associated conditions such as hypertension or clotting disorders.
- Maintain a healthy lifestyle including balanced diet and avoiding smoking, which can impact vascular health.
- Adhere to medications or recommendations from your care team.
Meet our Expert Specialists & Surgeons
Experience Compassionate, Expert Care

Our multidisciplinary team includes neurointerventional radiologists, neurosurgeons, neurologists, and specialized nursing staff experienced in managing DAVFs. At Pacific Neuroscience Institute, we combine leading-edge technology with compassionate care to diagnose and treat DAVF effectively. Our team performs advanced imaging and utilizes minimally invasive techniques to ensure the best outcomes with the least risk. Our center is equipped with state-of-the-art angiography suites and dedicated neurocritical care units. Patients benefit from personalized treatment plans and supportive rehabilitation services.
Learn More About a DuralrnArteriovenous Fistula
With timely and appropriate treatment, many patients have excellent outcomes, with complete fistula closure and symptom resolution. Untreated DAVFs, especially those with aggressive venous drainage, carry a significant risk of hemorrhage and neurological damage.
DAVFs vary in severity. Some are asymptomatic and low risk, while others can cause life-threatening hemorrhages or neurological deficits. Early diagnosis and treatment are critical.
Most patients recover within days to weeks following embolization, though some may require longer rehabilitation depending on the severity of symptoms or complications.
A DAVF is an abnormal connection between arteries and veins in the brain’s dura mater that disrupts normal blood flow.
With successful treatment, life expectancy is generally normal. Untreated, complicated fistulas may reduce life expectancy due to risk of hemorrhage.
Currently, there is no known hereditary link for DAVFs.
Surgical procedures vary but typically last several hours depending on complexity.
Symptoms may include headaches, seizures, vision changes, neurological deficits, and signs of increased intracranial pressure.
Resources

Get Expert Care from Leading Specialists
If you or a loved one are diagnosed with or suspect a dural arteriovenous fistula, timely evaluation and treatment are essential. Our expert team at Pacific Neuroscience Institute offers advanced diagnostic and therapeutic options tailored to your needs.
Written and reviewed by:
The Pacific Neuroscience medical and editorial team
We are a highly specialized team of medical professionals with extensive neurological and cranial disorder knowledge, expertise and writing experience.
Last Updated:






