Cavernoma
What is a Cavernous Malformation?
Overview
A cavernous malformation has many names that are all interchangeable and refer to the same diagnosis. Synonyms that refer to the same diagnosis include:
- Cavernoma
- Cavernous malformation
- Cavernous angioma
- Cavernous hemangioma
- Cerebral cavernous malformation (CCM)
Cavernous malformations are a vascular mass made up of abnormal dilated blood vessels characterized by distended blood-filled “caverns.” Vessels of a cavernous malformation mass have a tendency to leak and bleed because they lack the proper junctions between neighboring cells as well as the necessary structural support from smooth muscle and the stretchable material (elastin) that normally supports regular blood vessels.
Cavernous malformations are dynamic structures, changing in size and number over time and can range in size from a few millimeters to several centimeters.
Who is Affected?
Cavernous malformations are present in up to 0.5% of the general population, and they account for a large proportion (8-15%) of all brain and spinal vascular malformations. While more common in adults, people of all ages may be affected by them, and approximately 25% of all diagnosed cavernous malformations are found in children.
The majority of cavernous malformations that are diagnosed occur in individuals with only a single lesion and no family history of the disease. These cases are termed sporadic meaning they are not caused by an inherited genetic mutation.
Individuals with the familial (genetic) form of cavernous malformations are likely to have multiple lesions and may be more likely to experience symptoms associated with the disorder.
Cavernous Malformation Symptomsrn& Causes
Symptoms
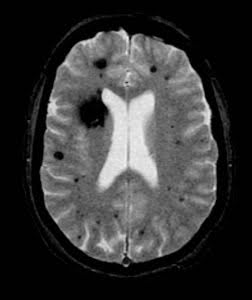
In many cases, a cavernous malformation causes no symptoms and can go unnoticed.
Leakage and bleeding from cavernous malformations is the underlying cause of clinical symptoms. Depending on the size and location of the cavernous malformation, this bleeding can cause brain damage and even in rare cases death. However, bleeding from cavernous malformations is often less severe than bleeding from aneurysms or arteriovenous malformations (AVMs) because they do not contain high-pressure arterial blood flow.
Symptoms of a ruptured cavernous malformation often come on suddenly and include a sudden, severe headache that is different from past headaches, nausea and vomiting, sensitivity to light, fainting or loss of consciousness and seizures.
Causes
Cavernous malformations are commonly associated with developmental venous anomalies (DVA) also called venous malformations or venous angiomas. A DVA is a type of vascular malformation that, on its own, does not cause any clinical symptoms.
At least 40% of sporadic cavernous malformations may develop within the vicinity of a DVA. The significance of DVA association with sporadic lesions is unclear. Perhaps this observation may suggest a difference in developmental mechanisms between sporadic and familial cavernous malformations.
When to See a Doctor
You should seek medical attention immediately if you experience sudden neurological symptoms such as:
- Sudden, severe headache unlike previous headaches
- Seizures or unexplained loss of consciousness
- Weakness or numbness affecting one side of the body
- Sudden vision changes or double vision
- Difficulty speaking, understanding speech, or problems with coordination
Even if symptoms resolve quickly, they may indicate a bleed or other neurological event that requires prompt evaluation. For individuals already diagnosed with a cavernous malformation, any new or worsening symptoms should be reported to your doctor as soon as possible.
Cavernous Malformation Diagnosis
While a new diagnosis of brain cavernous malformation can produce natural anxious responses in many patients, the most important thing to remember is that you are not alone. cavernous malformations can occur in as many as 1 out of every 200 people and our team of experts is here to help you understand your condition and determine an optimal, personalized treatment plan for your needs.
Many cavernous malformations are found incidentally during brain imaging for unrelated reasons, such as headaches or after a minor head injury. Others are diagnosed following symptoms like seizures, neurological changes, or signs of bleeding in the brain.
Cavernous malformations are usually detected through an MRI scan, which provides detailed images of the brain and can reveal the size, location, and characteristics of the lesion. Special MRI sequences such as susceptibility-weighted imaging (SWI) and gradient echo improve the ability to detect even small cavernous malformations or multiple lesions.
In some cases, a CT scan or neurological examination may be used to evaluate symptoms or rule out bleeding. For patients with multiple cavernous malformations or a family history, genetic testing may be recommended to identify hereditary forms of the condition.
If surgery or treatment is not immediately needed, your care team will recommend regular follow-up visits and imaging to monitor the cavernous malformation over time, ensuring that any changes are detected early.
Cavernous Malformation Treatmentrn& Outcomes
Treatment Options
Treatment for cavernous malformations depends on factors such as the size and location of the lesion, whether symptoms are present, history of bleeding, and the patient’s overall health. Many cavernous malformations are discovered incidentally and can be safely monitored without intervention.
If a cavernous malformation is small, located in an area where surgery would be risky, or not causing symptoms, careful observation is often recommended. This typically includes periodic MRI scans and neurological exams to detect any changes. Patients are also advised to avoid medications that may increase bleeding risk unless medically necessary.
Microsurgical resection may be considered when a cavernous malformation is:
- Causing recurrent symptomatic hemorrhage
- Producing progressive neurological deficits
- Responsible for seizures that do not respond to medication
- Located in an accessible brain area where surgical risks are acceptable
Modern surgical approaches often use minimally invasive keyhole techniques with high-powered microscopes and intraoperative monitoring to maximize tumor removal while protecting surrounding brain tissue.
For cavernous malformations that are deep in the brain or otherwise difficult to reach surgically, stereotactic radiosurgery (such as Gamma Knife) may be considered. This focused radiation treatment aims to reduce the risk of future bleeding, but its role remains controversial and is evaluated on a case-by-case basis.
If a cavernous malformation causes seizures, treatment usually begins with anti-seizure medications. If seizures remain uncontrolled despite optimized therapy, surgical removal of the cavernous malformation — along with any hemosiderin-stained brain tissue around it — may help improve seizure control.
Patient Outcomes
The outlook for someone with a cavernous malformation varies depending on factors such as size, location, number of lesions, and whether bleeding has occurred.
- Asymptomatic cavernous malformations often remain stable for years and may never cause problems.
- Cavernous malformations that have bled carry a higher risk of future bleeds, especially within the first two years after the initial event.
- Surgery, when needed, can often be curative for accessible lesions, with many patients experiencing resolution or significant improvement of symptoms.
- Long-term monitoring is important, as cavernous malformations can change in size or number over time.
Managing A Cavernous Malformation
Management of cavernous malformations often involves a team of specialists, including neurosurgeons, neurologists, neuroradiologists, and genetic counselors. Patients with multiple cavernous malformations may have a familial form of the condition linked to gene changes and could benefit from genetic counseling and testing.
Living with a cavernous malformation requires a proactive approach:
- Attend all scheduled follow-up appointments and imaging studies.
- Take prescribed medications as directed, particularly anti-seizure medications if you have had seizures.
- Avoid activities that carry a high risk of head injury.
- Discuss with your doctor any new medications, as some may affect bleeding risk.
- Maintain a healthy lifestyle, including regular exercise, balanced diet, and stress management.
Meet our Expert Specialists & Surgeons
Experience Compassionate, Expert Care
At Pacific Neuroscience Institute and our partner Providence hospitals across Southern California, our multidisciplinary team focuses on personalized treatment plans combining advanced technology with a patient-first approach. Our specialists work together to design personalized treatment plans. From diagnosis through long-term follow-up, our goal is to help you live your life to the fullest while minimizing risks and symptoms.
Learn More About a Cavernous Malformation
Many people live normal lives without ever having symptoms. Prognosis depends on size, location, and history of bleeding.
It can be, especially if it bleeds or is located in a critical brain area. However, many cavernous malformations are harmless and require only monitoring.
Most people with cavernous malformations have a normal life expectancy, particularly if they do not experience significant bleeding or other complications.
Observation with periodic MRI scans is common for stable, asymptomatic cavernous malformations. Surgery may be recommended for lesions causing symptoms or repeated bleeding.
Avoid activities with a high risk of head trauma. Discuss with your doctor before taking blood-thinning medications.
Cavernous malformations do not “heal” in the traditional sense, but some can shrink or remain stable over time without intervention.
It can be if it bleeds or causes significant neurological symptoms, but many are benign in their course.
Growth can be due to small repeated hemorrhages or genetic factors, particularly in the familial form.
There is no direct evidence linking stress to cavernous malformation bleeding, though stress can exacerbate symptoms like headaches or seizures.
No, cavernous malformations are not tumors—they are clusters of abnormal blood vessels.
Resources

Get Expert Care from Leading Specialists
If you have been diagnosed with a cavernous malformation or suspect you may have one, our multidisciplinary team can provide a thorough evaluation and discuss the most appropriate treatment options.
Contact Us
The Pacific Stroke and Neurovascular Center’s state-of-the-art facilities are located at:
Providence Saint John’s Health Center
2125 Arizona Ave., Santa Monica, CA 90404
310-829-8319
Providence Little Company of Mary Medical Center Torrance
4201 Torrance Blvd., Suite 520, Torrance, CA 90503
424-212-5340
Providence Saint Joseph Medical Center
501 S. Buena Vista Ave., Burbank, CA 90505
818-847-6049
Providence Holy Cross Medical Center
15031 Rinaldi St, Mission Hills, CA 91345
818-847-6570
Written and reviewed by:
The Pacific Neuroscience medical and editorial team
We are a highly specialized team of medical professionals with extensive neurological and cranial disorder knowledge, expertise and writing experience.
Last Updated:





