

What Is the Difference Between Ischemic stroke and Hemorrhagic Stroke?
by PNI Experts
Sandra Narayanan, MD, Vascular Neurologist and Neurointerventional Surgeon at the Pacific Stroke and Neurovascular Center at Pacific Neuroscience Institute, explains the difference between hemorrhagic and ischemic stroke.
The main difference between the two types of stroke is the underlying cause of the brain damage. In ischemic stroke, the damage is caused by a lack of blood supply, while in hemorrhagic stroke, it is caused by bleeding into the brain tissue. Both types of stroke are medical emergencies and require immediate medical attention to prevent further damage and improve outcomes.
What is a hemorrhagic stroke?
Also called cerebral hemorrhage or brain hemorrhage, a hemorrhagic stroke is a neurological emergency caused by a ruptured blood vessel in the brain. This accounts for 13% of all strokes but can present more dramatically due to blood released under pressure. Symptoms include sudden, severe headache, vomiting, seizure, weakness on one side of the face or body, and/or rapid deterioration in neurological function or consciousness. This can be particularly devastating in the case of subarachnoid hemorrhage (SAH). 5% of all strokes are due to SAH, which is most commonly caused by a ruptured brain aneurysm.
What is an ischemic stroke?
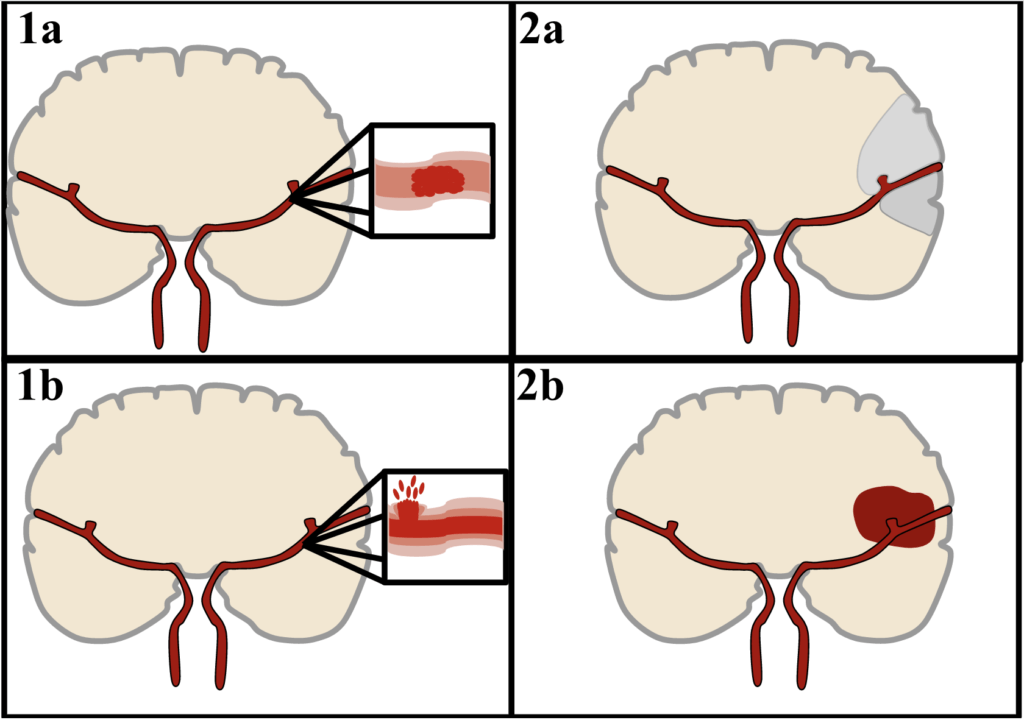
87% of all strokes are the ischemic type. Ischemia means a lack of blood supply. Ischemic strokes are usually caused by a clot, narrowing (stenosis), or blockage in a brain or neck artery, resulting in insufficient oxygen delivery to the brain. The gold standard treatment for ischemic stroke, especially within the first 3 hours, is a thrombolytic or clot-busting medication (e.g. tissue plasminogen activator [tPA/alteplase] or tenecteplase). However, up to 45% of strokes are caused by large-vessel occlusions (LVOs). The clot may not dissolve with the thrombolytic, or the patient may not arrive soon enough to receive the medication. The gold standard treatment for a Large-Vessel Occlusion stroke is mechanical thrombectomy or removing the clot from the brain circulation. For every minute that an LVO stroke goes untreated, 1.9 million neurons (brain cells) are permanently lost.
Identifying the signs of a stroke
You can increase the probability of you or your loved one obtaining timely, life-saving therapies and optimizing the recovery from an ischemic or hemorrhagic stroke by calling 911. Activating emergency medical services is key to starting early interventions prior to emergency department arrival and to minimizing any treatment delay.

Watch for these stroke signs or symptoms:
B: Balance – Is there a loss of balance or change in walking?
E: Eyes – Is there blurry vision in one or both eyes? Is there double vision?
F: Face – Is one side of the face drooping? Is the smile uneven?
A: Arms – Lift both arms; is one arm weak or drifting downwards? Is one arm numb?
S: Speech – Is speech garbled? Is he or she having difficulty getting the words out or understanding you?
T: Time – Time to call 911
About Pacific Stroke & Neurovascular Center
Pacific Stroke and Neurovascular Center offers leading-edge treatments and nationally recognized care for all types of neurovascular disorders at four locations in southern California. Our comprehensive stroke centers are staffed by highly qualified and seasoned experts. Every stroke and neurovascular patient is seen by fellowship-trained neurovascular stroke specialists rather than generalists. You can be confident of your care in the experienced and capable hands of our team of neurointerventional surgeons, vascular neurologists and neurosurgeons.
Stroke Center & Neurovascular Locations
The Pacific Stroke and Neurovascular Center’s state-of-the-art facilities are located at:
Providence Saint John’s Health Center
2125 Arizona Ave, Santa Monica, CA 90404
310-829-8319
Providence Little Company of Mary Medical Center Torrance
4201 Torrance Blvd, Suite 520, Torrance, CA 90503
424-212-5340
Providence Saint Joseph Medical Center
501 S. Buena Vista Ave, Burbank, CA 90505
818-847-6049
Providence Holy Cross Medical Center
15031 Rinaldi St, Mission Hills, CA 91345
818-847-6570
About Dr. Sandra Narayanan

Sandra Narayanan, MD, FAHA, FANA, FSVIN, is board-certified in neurology and vascular neurology by the American Board of Psychiatry and Neurology and CAST (Committee on Advanced Subspecialty Training)-certified in neuroendovascular surgery. She is a vascular neurologist and neurointerventional surgeon at Pacific Stroke & Neurovascular Center, Pacific Neuroscience Institute. Dr. Narayanan’s professional and research interests include stroke systems of care, cerebral venous sinus stenosis, quality improvement in neurointervention, and radiation safety.
About the Author
PNI Experts
Last updated: March 3rd, 2023

