
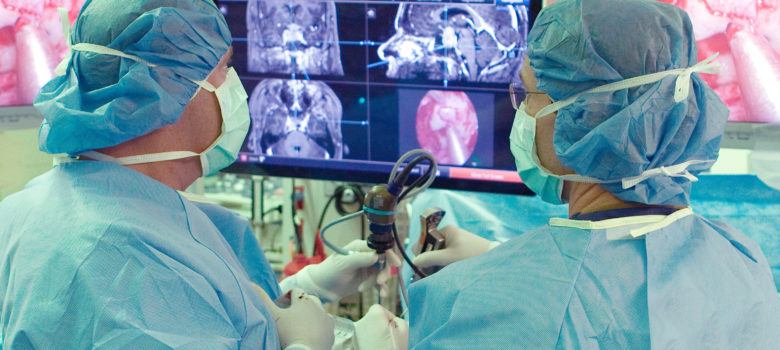
Achieving Better Outcomes in Endoscopic Pituitary Adenoma Surgery
by PNI Experts
Pacific Neuroscience Institute at Providence Saint John’s Strives to Set a New Standard in Landmark 10-year Study in over 500 Patients with Focus on Complication Avoidance. Findings published in this month’s “Pituitary” journal
SANTA MONICA, Calif., July 8, 2021— Intense focus on avoiding complications in a very delicate brain procedure has shown remarkable success among 514 patients treated over the past decade at Providence Saint John’s Health Center. An advanced minimally invasive surgical approach through the nostrils was used to remove pituitary adenomas.
More than 98 percent of patients in this landmark study at the hospital’s Pacific Neuroscience Institute were discharged to home after tumor removal, spending an average of only two days in the hospital. Hospital stay decreased over time with many patients going home one day post-surgery. Less than one percent of all patients sustained any permanent neurological injuries.
The findings were published in this month’s journal “Pituitary” and highlight the importance of protocols to avoid complications in patients undergoing endoscopic endonasal surgery for pituitary adenomas. Developed in large part at PNI and several other pituitary centers of excellence, these protocols set new standards for achieving the best possible outcomes for pituitary adenoma surgery. Over the 10-year study, the surgical team focused on consistent measures to avoid complications such as loss of sense of smell, nasal bleeding, carotid artery injury, pituitary gland damage, cerebrospinal fluid leaks and meningitis.

“Surgeons should continually strive to improve their results for their patients,” said neurosurgeon Daniel Kelly, M.D., director of PNI and senior author of the study. “Endoscopic pituitary surgery, which really started just over 25 years ago, is technically demanding and anatomically challenging given the location of the vital pituitary gland nestled in the skull base, surrounded by critical structures such as the optic nerves and carotid arteries. The operative corridor through the nostrils also contains the olfactory nerves for our sense of smell.”
Pituitary adenomas make up approximately 15 percent of primary brain tumors requiring surgery and are almost always benign. They can cause pituitary gland failure, vision loss, headaches and in some cases, over-secretion of hormones leading to conditions such as acromegaly (excess growth hormone) and Cushing’s disease (excel cortisol. “Our surgical goal is always to ‘sneak in and sneak out’, removing the tumor as completely as possible while leaving all these vital structures intact,” Dr. Kelly said.
Over 90% of patients with preoperative vision loss, partially or completely regained their vision with no cases of permanent vision decline after surgery. There were no carotid artery injuries and no complete loss of sense of smell. The most common surgical complication was a post-operative cerebrospinal fluid leak occurring in 1.7 percent of patients, which fell to 1.2 percent in the second half of the study. Worsening pituitary gland function occurred in 4.7 percent, while more than 50 percent saw gland function improve.
The results, Dr. Kelly said, suggest that collaborative team surgery with neurosurgeons and ENT surgeons applying consistent safety protocols, hugely benefits patients, and compared to prior large series, these results are among the best and most extensive published.
“We believe these results set a new standard for complication avoidance and optimizing outcomes for pituitary adenoma surgery and are happy to share this experience with colleagues who manage these patients,” he said.
About Dr. Daniel Kelly

Dr. Daniel Kelly, a board-certified neurosurgeon, is the Director and one of the founders of the Pacific Neuroscience Institute, Director of the Pacific Brain Tumor Center and Pacific Pituitary Disorders Center, and is Professor of Neurosurgery at Saint John’s Cancer Institute at Providence Saint John’s Health Center. Considered to be one of the top neurosurgeons in the US, he has one of the world’s largest series in endonasal surgery with over 2000 procedures performed including over 900 endoscopic endonasal surgeries, and almost 2000 craniotomies for brain and skull base tumors. In practice for over 25 years, he is a multiple recipient of the Patients’ Choice Award, and has been awarded the Southern California SuperDoctors distinction 15 years in a row.
Useful Links
About the Author
PNI Experts
Last updated: August 30th, 2021