

October is Facial Pain Awareness Month
by Zara Jethani
Facial Pain Syndromes
For most of us Halloween is a day of fun where the terror is pretend and an excuse to dress up in the macabre. But for some people, the horror is real every day. Imagine one side of your face being constantly stabbed by nails. That is how patients who suffer from facial pain such as trigeminal neuralgia describe this terribly painful condition. Epidemiologists estimate that approximately 39 million adult Americans have some degree of ongoing chronic craniofacial pain1. Our doctors at the Pacific Facial Pain Center treat a wide spectrum of facial pain syndromes which are caused due to issues arising in the temporomandibular joint (TMJ), the muscles or the nerves.
Temporomandibular Joint (TMJ) Dysfunction
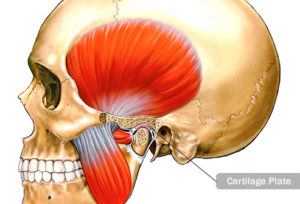
Temporomandibular dysfunction (TMD) refers to dysfunction of the joint resulting in joint clicking, joint locking or arthritis. Depending on the diagnosis, the condition is managed using various treatments. Typical findings include intermittent locking and/or painful clicking of the joint. In severe cases, the mouth can become unable to open or close.
Treatment of TMJ ranges from supportive therapy (eating soft foods, applying ice or moist heat, and NSAIDS) to repositioning splint therapy. In some cases, physical therapy, arthrocentesis (joint aspiration) or injections may be necessary.
Pain Caused by Muscle
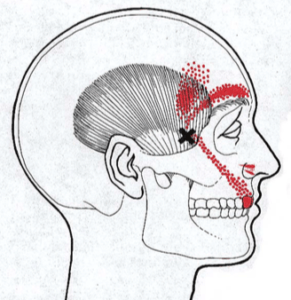
Facial pain caused due to muscle dysfunction occurs when sensitive areas of a muscle (trigger points) generate pain in a seemingly unrelated distant location, called referred pain or myofascial pain. Treatment options include eliminating the provoking factors, incorporating a myofascial protocol and/or trigger point injections.
Facial Pain Caused by Nerves
There are many facial pain syndromes caused by nerve dysfunction including trigeminal neuralgia and hemifacial spasm.
Trigeminal Neuralgia

Trigeminal neuralgia (TN) is probably the most well known and notorious of the facial pain syndromes caused by nerve dysfunction and is particularly traumatic, warranting it’s own awareness day on October 7th.
Often called the Suicide Disease, trigeminal neuralgia pain may range from sudden, severe, and stabbing to a more constant, aching, burning sensation. Any light or normal touch can act as a trigger for an episode of intense facial pain such as shaving, washing the face, putting on makeup, brushing teeth, eating, drinking, talking, or even the feeling of cold air on the face. The pain may be seasonal with a peak in the fall and spring.
As stated by the National Institute of Health (NIH), TN is typified by attacks that stop for a period of time and then return, but the condition can be progressive. The attacks often worsen over time, with fewer and shorter pain-free periods before they recur. Eventually, the pain-free intervals disappear and medication to control the pain becomes less effective. The disorder is not fatal, but can be debilitating.
Often, diagnosis is delayed due to conflicting diagnoses. TN and its variants can be caused by multiple sclerosis, benign tumors, prior inflammation, herpes zoster (shingles) and post-herpetic neuralgia and trauma. The most common cause of classic Trigeminal Neuralgia (TN1) is due to a blood vessel pulsating against the trigeminal nerve at the brainstem.
There are many types of treatment options, ranging from medical therapy to surgical or radiosurgical options. At the Pacific Facial Pain Center, we offer a complete approach to each patient, offering treatments tailored to the patient’s underlying symptoms, medical background and treatment expectations.
Medical therapies include various anti-epileptic medications such as carbamazepine or gabapentin; or tricyclic antidepressants for the treatment of pain. Normal pain medications like non-steroidal anti-inflammatory drugs (NSAIDs) or opioid narcotics are typically not effective. These medications are effective in many patients, but some patients either do not respond or cannot tolerate the side-effects. Hence, they may be candidates for procedural intervention.
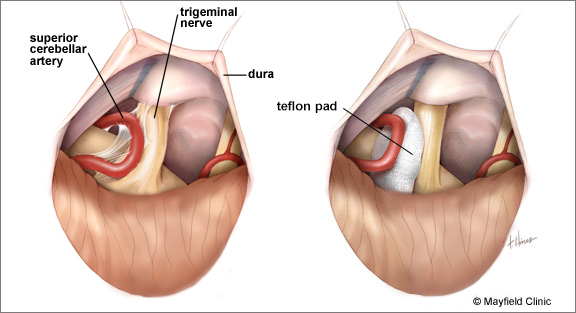
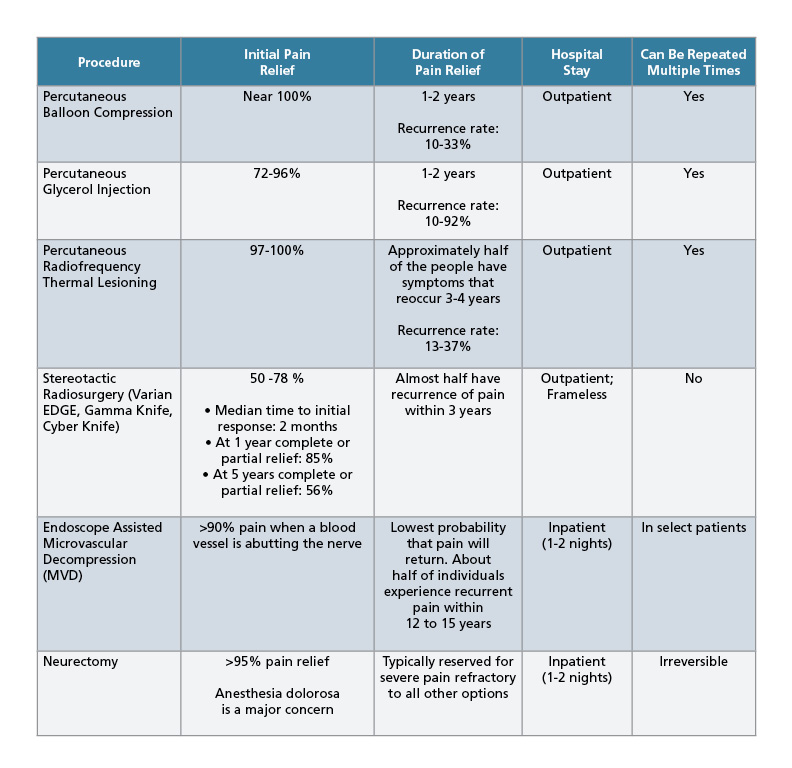
Minimally invasive surgical procedures are performed by neurosurgeon Dr. Garni Barkhoudarian. Generally, these treatments can be divided into percutaneous treatments or nerve damaging (rhizotomy) procedures and nerve decompression (microvascular decompression – MVD). Each has some rate of success and durability and side effects can vary. In very select patients, deep brain stimulation (DBS) may be considered as a treatment option for refractory facial pain.
For more information about facial pain syndromes, please visit PacificFacialPain.org or call us at 310-582-7640.
About Dr. Barkhoudarian

Garni Barkhoudarian, MD, is a neurosurgeon with a focus on skull base and minimally invasive endoscopic surgery. He has particular interest and expertise in pituitary and parasellar tumors, brain tumors, skull-base tumors, intra-ventricular brain tumors, colloid cysts, trigeminal neuralgia and other vascular compression syndromes. He is an investigator in a number of clinical trials evaluating the efficacy of various medical or chemotherapies for pituitary tumors and malignant brain tumors. For virtually all tumors and intracranial procedures, Dr. Barkhoudarian applies the keyhole concept of minimizing collateral damage to the brain and its supporting structures using advanced neuroimaging and neuro-navigation techniques along with endoscopy to improve targeting and lesion visualization.
Reference
1 Pain Management, An Issue of Neurosurgery Clinics of North America. Ashwini Sharan. November 22, 2014. Elsevier Health Sciences
Banner image: The Scream, Edvard Munch
About the Author

Zara Jethani
Zara is the marketing director at Pacific Neuroscience Institute. Her background is in molecular genetics research and healthcare marketing. In addition, she is a graphic designer with more than 20 years experience in the healthcare, education and entertainment industries.
Last updated: November 6th, 2024