

Dealing with Hemifacial Spasm
by Mahyar Pakizegee
When Michael Watkins came to see neurosurgeon, Garni Barkhoudarian, MD, in 2014, he had been experiencing facial spasms for over two years.
In 2012, Michael Watkins began noticing unusual spasms and twitching on the left side of his face. Initially the spasms improved spontaneously, only to recur one year later, and this time much more noticeably.
Michael, an entertainment executive, has always been in front of people working in various roles throughout his career including that of disc jockey, event manager, agent and minor league baseball team owner. Now as partner of 3 Point Productions and the company’s business director developing new business and creating relationships with sports business professionals, Michael found increasingly that the facial spasms were affecting his ability to work. “I had to miss many meetings with clients due to my worsening facial spasms,” remembers Michael.
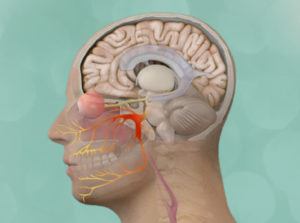 Many patients like Michael, suffer from hemifacial spasm, a medical condition characterized by involuntary twitching of the muscles of facial expression affecting one side of the face. Patients suffering from this condition often note inappropriate winking and facial tics that are easily observed by their peers. Social interactions can become problematic and the patient becomes self-conscious. The condition affects quality of life and in some cases, can lead to psychological disorders such as depression and anxiety.
Many patients like Michael, suffer from hemifacial spasm, a medical condition characterized by involuntary twitching of the muscles of facial expression affecting one side of the face. Patients suffering from this condition often note inappropriate winking and facial tics that are easily observed by their peers. Social interactions can become problematic and the patient becomes self-conscious. The condition affects quality of life and in some cases, can lead to psychological disorders such as depression and anxiety.
Hemifacial spasm is caused by the misfiring of the facial nerve, also known as the 7th nerve cranial nerve, when it becomes compressed by a nearby blood vessel. These nerves are present on both side of the face but typically only one side of the face is affected in this condition. The facial nerve performs a multitude of functions – primarily controlling the muscles of facial expression which include closing one’s eye, smiling, chewing and expressing emotion. In addition, the facial nerve regulates the lacrimal and salivary glands – which produce tears and saliva respectively, and also controls select muscles modulating hearing. Some patients with hemifacial spasm report changes in their hearing, including tinnitus (ringing in the ears) and sometimes mild hearing loss. The sensation of taste in the front two-thirds of the tongue is also mediated by the facial nerve.
Generally, hemifacial spasm starts by affecting the eyelids – also called blepharospasm – and then progresses to the forehead, cheek and/or mouth. Many patients have blepharospasm but never progress to hemifacial spasm. Of note, there is no pain associated with this type of spasm. Facial pain syndromes like trigeminal neuralgia, can also have facial spasms or tics, but pain is the predominant symptom.
Affecting women more than men, hemifacial spasm is quite a rare medical condition, affecting approximately 8 in 100,000 people in the United States, and often presenting during middle age. The disease can be associated with a number of conditions including tardive dyskinesia, tics, myokymia, cranial dystonia, facial nerve injury (due to direct trauma) and delayed effects of Bell’s palsy.
However, the most common cause of hemifacial spasm remains vascular compression of the facial nerve as it exits the brainstem in the skull. The best test to evaluate for this vascular compression is a high-resolution magnetic resonance image (MRI) as well as MR angiogram (MRA) of the brainstem.
Addressing the underlying cause of the facial nerve compression can relieve the symptoms of hemifacial spasm completely. In approximately 80 percent of patients botulinum toxin (Botox®) injections can be successfully used to regulate nerve transmission and stop the facial spasm.
As Michel’s condition persisted impacting both his business and social interactions, he sought advice from local physicians, who recommended he consider botulinum toxin injections to manage these spasms. However, Michael was concerned about this treatment strategy, “I didn’t feel comfortable and I knew I could find a better answer,” he says.
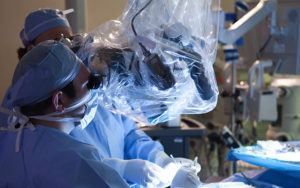
When injections fail, surgery is often recommended. This surgery, called endoscope-assisted microvascular decompression (MVD) of the facial nerve, is a minimally invasive procedure that stops the hemifacial spasms.
 Michael visited Dr. Garni Barkhoudarian, where both Botox® injections and minimally invasive surgery were discussed. Recent studies have demonstrated that there are better outcomes when surgical intervention is performed early in the disease course, typically less than 5 years after disease onset. As Michael was an ideal candidate for the MVD surgery, he decided to proceed with surgery even though this would be the first surgical procedure of his life!
Michael visited Dr. Garni Barkhoudarian, where both Botox® injections and minimally invasive surgery were discussed. Recent studies have demonstrated that there are better outcomes when surgical intervention is performed early in the disease course, typically less than 5 years after disease onset. As Michael was an ideal candidate for the MVD surgery, he decided to proceed with surgery even though this would be the first surgical procedure of his life!
Carefully moving aside the blood vessel that was compressing the facial nerve, Dr. Barkhoudarian placed a non-reactive miniature teflon pad between the vessel and the nerve. With the blood vessel no longer impinging upon the nerve, the muscular spasms caused by the misfiring facial nerve would stop.
Michael’s surgery was successful and he was able to go home after two days. He returned to his daily activities immediately much to the amazement of his family, and has not experienced any further facial spasms. He is able to confidently conduct business and enjoy social occasions again. “Dr. Barkhoudarian is more than just a doctor,” Michael adds.”It felt like I’ve known him for several years. I trust him completely.”
For more information about hemifacial spasm and facial pain syndromes, please contact us at 310-829-8265 or visit the website at PacificFacialPain.org.
Mahyar Pakizegee is a fourth year baccalaureate student at the University of California, Los Angeles majoring in History. His goal is to attend medical school and pursue his dream of being an inspiring physician. He is a contributing author under the guidance of Dr. Garni Barkhoudarian, neurosurgeon at Pacific Neuroscience Institute.
Zara Jethani, MS, MBA, is the marketing director for the Pacific Neuroscience Institute. Her background is in graphic design, molecular genetics research and healthcare marketing.
About the Author

Mahyar Pakizegee
Mahyar Pakizegee is a fourth year baccalaureate student at the University of California, Los Angeles majoring in History. His goal is to attend medical school and pursue his dream of being an inspiring physician. He is a contributing author under the guidance of Dr. Garni Barkhoudarian, neurosurgeon at Pacific Neuroscience Institute.
Last updated: October 5th, 2018