Stroke Treatment & Prevention

Jason Tarpley, MD, PhD, Director of the Stroke and Neurovascular Center at Pacific Neuroscience Institute (PNI) explains how to identify and treat stroke, and reviews lifestyle changes you can make to lower your risk of stroke today.

At Pacific Neuroscience Institute (PNI), we are recognized for our commitment and success in implementing the highest standard of stroke care. This past year alone, the expertise of PNI specialists resulted in affiliate hospitals Providence Saint John’s Health Center (Santa Monica) and Providence Little Company of Mary (Torrance) receiving multiple national recognitions from the American Heart Association, including the Get With The Guidelines® Stroke Gold Plus Quality Achievement Award for proven dedication to ensure that all patients have access to best practices and life-saving care.
What is a stroke?
When it comes to stroke, it’s easiest to think of it as “brain plumbing.” There are “clogged pipes” and “burst pipes,” each with a different treatment procedure.
Ischemic Stroke
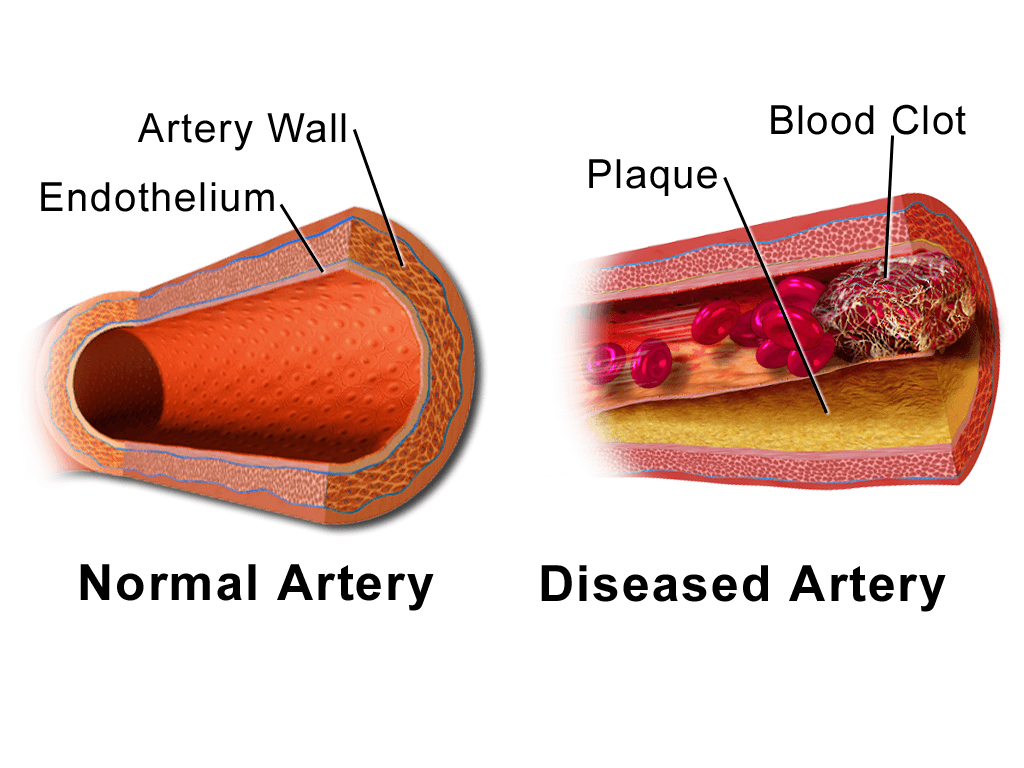
- “Clogged pipes” are known as ischemic strokes. Ischemic stroke happens when a blood vessel in the brain is blocked, preventing blood flow to the brain. When this happens, a portion of the brain is at risk. Ischemic strokes, or “clogged pipes,” are the most common type of stroke, attributing to 80% of all stroke cases.
Hemorrhagic Stroke
- “Burst pipes” are known as hemorrhagic strokes. A hemorrhagic stroke happens when a blood vessel in the brain bursts. This can happen from an aneurysm, which is a bubble on the surface of an artery, as well as hypertension and high blood pressure. Aneurysms account for 3-5% of all stroke cases.
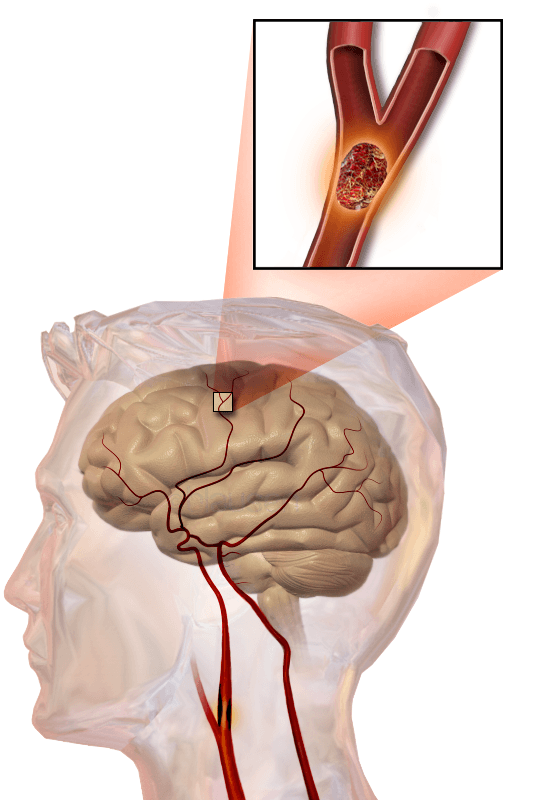
What treatment is available for ischemic stroke?
Treatment for ischemic stroke is very effective and available, but it is also time-dependent. It is very important to act quickly if you or a loved one is experiencing stroke symptoms.
When you have an ischemic stroke, you lose brain cells at a staggering rate. It is estimated that two-million brain cells are lost per minute during an ischemic stroke. However, there are two highly effective therapies for ischemic stroke. One treatment for ischemic stroke isTenecteplase, a clot-busting medication that is administered by experts after it is determined that you are having an ischemic stroke.
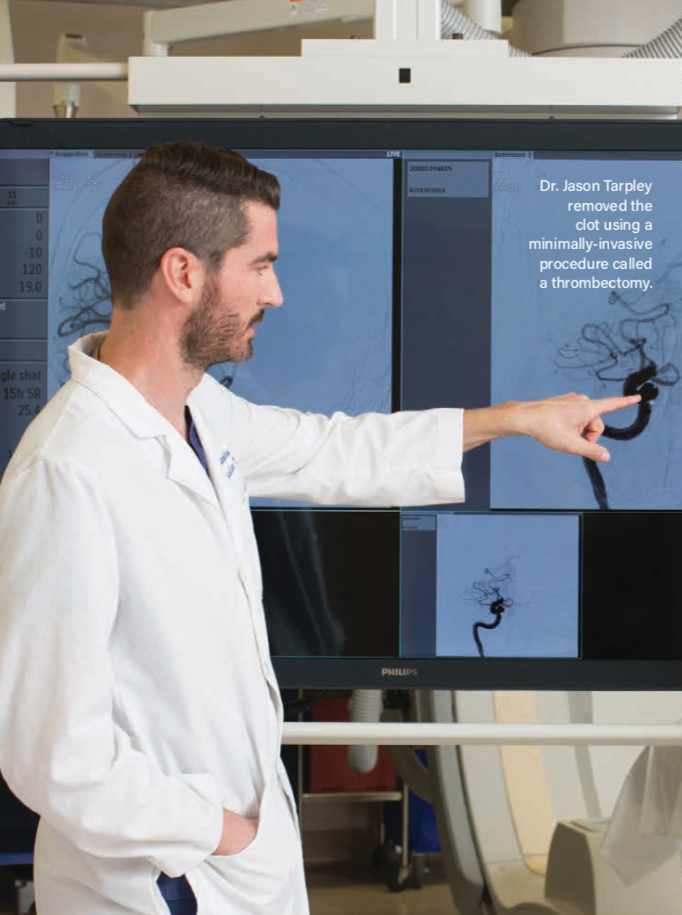
Another treatment for ischemic stroke is a thrombectomy, which is a procedure for large blockages in the blood vessels of the brain. During a thrombectomy, experts navigate a catheter into the brain to locate the blood clot and pull it out.
6 symptoms of stroke
Stroke causes sudden neurological change. A patient may appear normal for one second, and then suddenly undergo a neurological change that may present in various ways physically. Using the acronym known as BE FAST helps people remember the physical symptoms of a stroke.
- “B” stands for balance. If you suddenly have difficulties with your gait, such as walking or balance, you may be experiencing a stroke.
- “E” stands for eyes. If you have sudden visual difficulties, such as vision loss or blurring, this can be a sign of a stroke.
- “F” stands for facial droop. This symptom is one that lots of people may know, but if you or a loved one is experiencing a facial droop, this is a sign of a stroke. A quick check for facial droop is to smile. Smiling allows us to see proper excursion on both sides of the face. If only one side of the face has an excursion, you may be experiencing a stroke.
- “A” stands for arm weakness. Again, we are talking about symptoms that happen on one side of the body. If you or a loved one extends their arms in front of them, and one arm drops suddenly, this is a sign of stroke.
- “S” stands for speech. If you are experiencing sudden speech difficulty, this is a telltale sign of a stroke. Speech difficulty can present as sudden garbled speech, loss of words, or inability to speak at all.
- “T” stands for time. If you or a loved one is experiencing any of the symptoms in the BE FAST acronym, it is time to call 911.
When do I call 911 for stroke symptoms?
If you or a loved one are experiencing any BE FAST symptoms of stroke, call 911 right away. You may think it is more effective to drive to the hospital, but calling 911 gives you the best chance of recovery. Emergency Medical Services (EMS) work directly with comprehensive stroke centers. In Los Angeles County, stroke specialists at PNI train EMS to ensure stroke evaluation and treatment. As soon as you call 911, EMS is already on the phone with PNI specialists going over your symptoms to apply the appropriate treatment.
What is the difference between a primary and comprehensive stroke center?
In Los Angeles County, there are more than sixty (60) primary stroke centers. Every primary stroke center has the ability to give clot-busting medication to treat ischemic strokes. However, if you have a large vessel occlusion (or LVO), that could require a thrombectomy, you need to be treated at a higher-level comprehensive stroke center.
Both PNI affiliate hospitals Providence Saint John’s Health Center (Santa Monica) and Providence Little Company of Mary (Torrance) met specific rigorous guidelines as a Primary Stroke Center/Comprehensive Stroke Center, featuring a comprehensive system for rapid diagnosis and treatment of stroke patients admitted to the emergency department.
What is endovascular thrombectomy?
Unlike smaller blood clots, which can be broken by a clot-busting medication such as Tenecteplase, larger occlusions in the blood vessels of the brain require more advanced treatment.
Endovascular thrombectomy is a type of thrombectomy used to treat larger blood clots in a larger artery. This intra-arterial procedure involves putting in a catheter about the size of an iPhone charging cable into the artery of the leg or wrist, through which we can navigate a smaller catheter into the artery of the neck, and an even smaller one into the artery of the brain. From there, we use an even smaller catheter through the clot.
Using this technique, an endovascular thrombectomy allows navigation all the way up into the brain to pull out blood clots of large vessel occlusion. In the case of aneurysms, which are a bubble on the surface of an artery, we can navigate a small catheter into that aneurysm and actually fill the aneurysm, plug it up, and prevent it from re-rupturing.
How do experts identify stroke treatment?
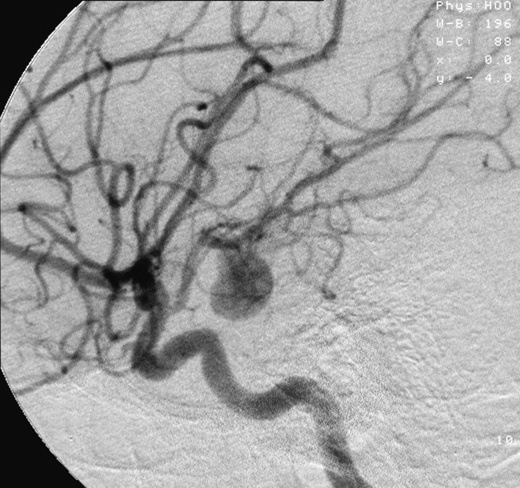
When someone has a stroke, they receive a very standardized expedited workup, including a non-contrast head CT. A non-contrast head CT is a scan that stroke experts use to quickly identify the type of stroke.
After a patient receives a non-contrast head CT, they receive two additional scans. The first is a CT angiogram, which takes a look at the blood vessels. The second is advanced perfusion imaging, which detects and identifies occlusion (LVO or medium vessel occlusion), allowing specialists to determine if a patient might benefit from a thrombectomy.
What is the recovery time after a stroke?
After a patient receives stroke treatment at a comprehensive stroke center, we prioritize their full recovery. A patient can expect to be seen by numerous rehab therapists, including speech and language pathologists, physical therapists, and occupational therapists. These services will serve to assist in rehabilitation for the patient. The typical timeframe for recovery is 90 days.
What is an aneurysm?
A brain aneurysm, or cerebral aneurysm, is a bubble on the surface of the artery in the brain. Aneurysms can occur anywhere in the body, but when talking about stroke, these are aneurysms of the brain.
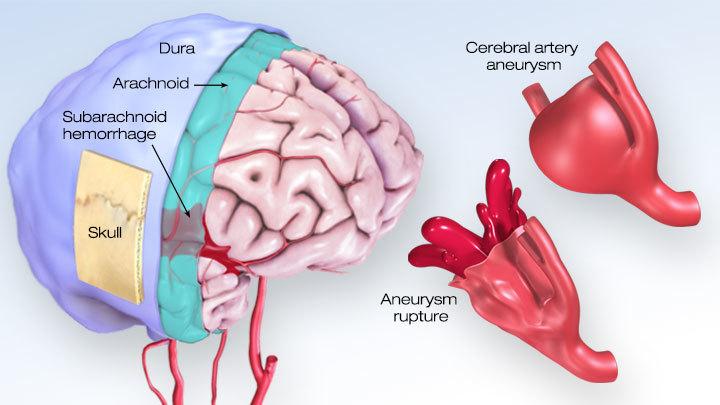
Roughly two-percent (2%) of the world’s population has an unruptured brain aneurysm, according to the Brain Aneurysm Foundation. However, these are typically non-life-threatening as long as they remain small and do not cause pressure. Unruptured brain aneurysms do not always cause symptoms and are typically discovered accidentally for another procedure.
However, if the brain aneurysm bursts, this is a life-threatening medical emergency condition called a subarachnoid hemorrhage. A subarachnoid hemorrhage is a ruptured brain aneurysm that causes blood to pool into the space around the brain creating pressure. A subarachnoid hemorrhage can lead to permanent brain damage or death. The main symptom of a subarachnoid hemorrhage is a sudden headache.
How likely is an aneurysm?
In the United States, it is estimated that 6.7 million people (1 in 50) have an unruptured brain aneurysm. Globally, it is estimated that two to three percent (2-3%) of the population has an unruptured brain aneurysm.
What are the risk factors for aneurysm?

Brain aneurysms occur more in women than in men, particularly women over the age of fifty five. Modifiable risk factors for a brain aneurysm include smoking, high blood pressure, and cocaine use.
If you have a first-degree relative with an aneurysm, it is important to get screened. Genetics are a risk factor component for aneurysms.
What is the treatment for an aneurysm?
Most brain aneurysms are treated by endovascular thrombectomy. A catheter the size of an iPhone charging cable is inserted into the artery of the leg or arm, through which a series of smaller catheters between 0.035 inches and 0.074 inches are inserted through navigate all the way up to the brain to plug the aneurysm and prevent rupture or re-rupture.
Can strokes be prevented?
Up to 90% of strokes are preventable by adopting healthy lifestyle choices. These include engaging in regular exercise, avoiding smoking, and adopting a healthy diet.
How can I prevent stroke if I have diabetes?

If you have diabetes, ensure that your hemoglobin A1C (HbA1C) levels are below 6.5. Elevated levels of HbA1C are associated with increased stroke risk. High levels of cholesterol and blood pressure are also associated with stroke.
Regularly check your HbA1C, cholesterol, and blood pressure levels to ensure that they are not elevated to prevent stroke risk.
What foods prevent stroke?
When it comes to diet, the Mediterranean diet is the single most “powerful pill” for preventing stroke. Eating the Mediterranean diet can prevent your risk of stroke by twenty percent (20%). This is because the Mediterranean diet avoids three main food groups that are known to increase your risk of stroke, including red meat, dairy, and concentrated sweets and sugar.
Instead, the Mediterranean diet focuses on increasing healthy food groups, such as legumes, fruits, vegetables, nuts, poultry, and fish.
What exercise prevents stroke?
Exercise is critical for preventing stroke. Although there is no amount of exercise that is considered too much for preventing stroke, consistent exercise is key. Pick an exercise that you enjoy doing on a regular basis. This may look like running, swimming, or weight training.
If you are new to exercise, walking is a great option. Tai chi is also a great alternative for patients with a tendency to fall.
What are the risk factors for stroke?
There are modifiable and non-modifiable risk factors for stroke. Modifiable risk factors include exercise, diet, and smoking. High cholesterol and high blood pressure are also modifiable risk factors for stroke. If you have diabetes, having high cholesterol and high blood pressure increases your risk of having a stroke.
Non-modifiable risk factors for stroke include age. The older you get, the more likely you are to have a stroke.
What is the future treatment for stroke?
In the past ten years, stroke treatment has grown exponentially. It is an exciting time to be in the neurosciences. We are accomplishing milestones that we did not think were possible for ischemic stroke treatment, and our endovascular techniques for an aneurysm are getting better and better. What we can offer stroke patients today are the most innovative treatments, backed by years of research and clinical trials.
Pacific Stroke & Neurovascular Center
At the Pacific Stroke & Neurovascular Center, our multidisciplinary experts are leaders in their field and contribute to the advancement of knowledge and understanding of neurovascular disease. PNI holds the Get With The Guidelines® Gold Plus Quality Achievement Award and Target Stroke Elite Plus Honor Roll. This award recognizes our commitment and success in implementing a high standard of stroke care by ensuring that our stroke patients receive treatment that meets nationally accepted, evidence-based standards and recommendations.

Providence Saint John’s Health Center and Providence Saint Joseph Medical Center are both Advanced Primary Stroke Centers designated by The Joint Commission and nationally recognized by the American Heart Association for their commitment and success in the rapid diagnosis and treatment of stroke patients. This external certification emphasizes timely diagnosis, treatment, and prevention of future strokes and identifies excellence in stroke care.
For more information, please contact us at stroke.center@providence.org or call 310-582-7640.
Our Stroke Team
Contact Us
The Pacific Stroke and Neurovascular Center’s state-of-the-art facilities are located at:
Providence Saint John’s Health Center
2125 Arizona Ave., Santa Monica, CA 90404
310-829-8319
Providence Little Company of Mary Medical Center Torrance
4201 Torrance Blvd., Suite 520, Torrance, CA 90503
424-212-5340
Providence Saint Joseph Medical Center
501 S. Buena Vista Ave., Burbank, CA 90505
818-847-6049
Providence Holy Cross Medical Center
15031 Rinaldi St, Mission Hills, CA 91345
818-847-6570

