

Cancer and Survivorship
by Zara Jethani
The ever-expanding scope of medicine has radically transformed our lives.
Our significant medical advances go hand in hand with longer life and since 1900 the global average life expectancy has more than doubled and is now approaching 70 years, with the average person in the United States living up to almost 79 years old. However, with longer lifespans comes more disease, often related to aging. Among these, cancer ranks as the leading cause of death in the United States after heart disease, and is projected to account for over 600,000 estimated deaths in 2017 and approaching 1.7 million new cases of cancer in the United States.

On the positive side, cancer survival continues to improve, with the overall cancer death rate falling by 13% since the beginning of the decade. As a result, there are a lot of cancer survivors that are living for long survivorship periods.
What does cancer survivorship mean?
“In the past, we used to begin counting survivorship after treatment when the patient was in remission,” says neuro-oncologist Santosh Kesari, MD, PhD. “Today, we think of cancer survivorship beginning at the time of diagnosis.”

Dr. Kesari is director of neuro-oncology, Providence Saint John’s Health Center and chair of the department of translational neurosciences and neurotherapeutics at Saint John’s Cancer Institute and Pacific Neuroscience Institute in Santa Monica, CA. His practice and research specializes in brain cancers such as glioblastoma and cancers that have metastasized to the brain from other sites such as breast or lung. He says that after such a devastating diagnosis, personalizing information for each patient is a key component in their journey of survivorship.
It is important to have a support network. Patients and their loved ones are thrown into having to deal with not only the diagnosis but also the convoluted path of treatment and its aftermath. There are so many questions that come up. How can I adjust my work schedule? Who will look after the kids? Does my insurance pay? What treatment options will be best for me? Should I get a second opinion? How will I respond to therapy? Will I get better?
“As treatments have become more successful, patients are living longer and longer. But there are many factors that come into play such as managing the long-term side effects from initial cancer therapy sometimes called ‘chemobrain’,” says Dr. Kesari. “At our clinics we deal with the issues of survivorship on a daily basis and at our Center for Quality & Outcomes Research we specifically focus on measures and initiatives for improving patients’ quality of life.”

Melanie Goldfarb, MD, MS, endocrine surgeon at the Providence Saint John’s Health Center, is the Medical Director of the Survivorship Program, which was rolled out over the summer. Patients can expect a number of supports to aid them in their fight against cancer, she says.
“All new cancer patients are seen by a multidisciplinary team of an oncology social worker and specialized survivorship Nurse Practitioner (NP) who work together with the medical team to coordinate and support all of the ‘non-medical’ aspects of being a cancer survivor and/or a caregiver. They complete a distress screening and needs assessment which helps us tailor personalized referrals and support for each patient. At the end of treatment, each patient and their primary care provider are given a survivorship care plan which details their individualized treatment and all of their follow-up recommendations, including which doctor is responsible for each aspect of follow-up care,” she says. Some of the resources include patient support and caregiver groups, yoga classes, nutrition, and the American Cancer Society’s “Look Good, Feel Better” program.
Sister hospital Providence St. Joseph’s Medical Center in Burbank, CA offers dietary guidelines for living well, physical therapy consultations to help getting back to normal activity levels, stress reduction techniques through mind-body programs and alleviation of residual side effects from treatment, through acupuncture or massage as part of their survivorship program. “Many studies have now shown the positive impact of various activities not only for quality of life, but also improved survival for many cancer patients,” Dr. Goldfarb adds. In addition, there are several online resources that help patients navigate their disease. For example, LIVESTRONG provides free, personalized support for the practical, physical and emotional concerns that people face when dealing with a cancer diagnosis.
Jump, Jive & Thrive
As part of a growing community of survivors, past and present patients want supportive forums where they can discuss topics and issues particular to their experience. The Jump, Jive & Thrive Cancer Survivorship Summit held in early October was a unique star-studded weekend long event in Los Angeles combining music, gymnastics and dance to celebrate cancer survivorship. Artists and athletes gathered together to highlight their stories and raise awareness of cancer survivorship.

To kick off the event, Kauser Ahmed, PhD, Associate Director & Training Director at Simms/Mann-UCLA Center For Integrative Oncology moderated a panel of oncology experts and cancer survivors facilitating an open and candid discussion about what it means to be a cancer survivor and thriver. The event was produced in association with the Breast Cancer Research Foundation, The Leukemia & Lymphoma Society (LLS), and the Pediatric Cancer Research Foundation (PCRF) and was broadcast on CBS.
“In any competition, you want to win,” says Scott Hamilton. “Whether in cancer or competition, you want to have the tools to be successful.” In his new book called “Finish First: Winning Changes Everything“, he breaks down the recipe for success, and he encourages the hidden potential, the champion within all of us, to come out.
Maslow’s Hierarchy of Needs
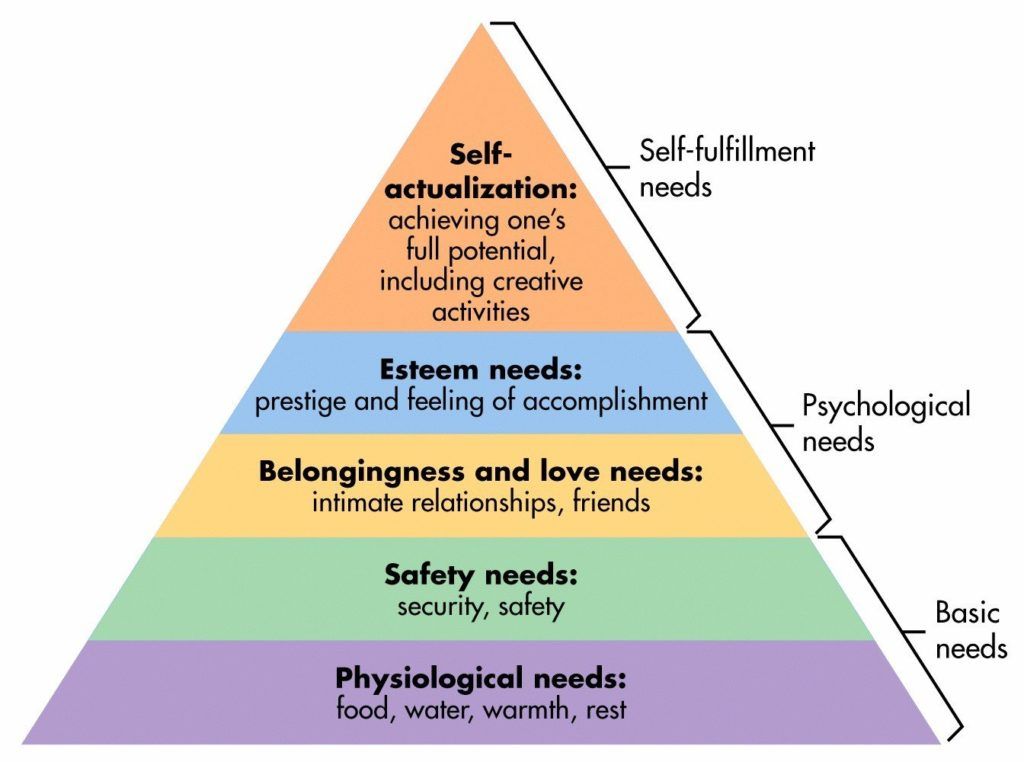
Survivorship and thrivership are possible and sustainable. In the 1940s and ‘50s Abraham Maslow proposed a revolutionary structure outlining our human needs in order to survive and ultimately thrive. Flexible in its design, the basic premise says that each of us has a set of needs that fall into five different categories: physiological including the need for sleep; safety needs; need to belong; esteem needs; and eventually self-actualization. Patients and families can look at this as a guideline to help rebuild quality of life after disease strikes.
The Long Term
As the population ages and because of shifts in so many aspects of our environment including the food we eat, it is more and more likely that we will run into people who have experience with cancer. It is estimated that the burden of cancer in the United States will be such that almost 40% of men and women will be diagnosed with cancer at some point during their lifetimes.

“Cancer is a family disease,” says Marlon Garzo Saria, PhD, RN, director of the Center of Quality & Outcomes Research at Pacific Neuroscience Institute. “I am not referring to the small percentage of cancers that can be passed on from one generation to the next. What I mean is that a diagnosis of cancer affects the whole family.” Caregiving research reveals a huge gap is the care that family caregivers receive and need, he says. “For family caregivers, not only are standardized assessment tools not integrated into usual care practice, the structures and processes around caregiver assessment have not yet been developed. One of the aims of our program is to integrate systematic family caregiver assessment into practice. Studies have shown that family caregivers and healthcare providers report improved outcomes in areas such as depression and anxiety, caregiver burden, quality of patient-caregiver relationship and quality of life, when caregiver needs are assessed.” Dr. Saria and his team continue to evaluate technologies such as mobile-based apps that can provide ongoing support.
As technology and medicine continue to evolve, there are more opportunities for these two fields of science to come together. One area that appears to be lacking is the preventive management of side effects of treatment, says Dr. Kesari. “We are trying to be proactive by figuring out the exact issues that effect each patient and monitoring the symptoms from Day 1 of treatment.” Technology such as the LivingWith app from Pfizer, FitBits, CancerLife, and more are making it easier for patients to document what they are going through, he says, and that is data that can be used to understand the burden of disease and treatment, which in turn has a direct impact on the quality of survivorship both for the patient and their families.
For more information about the Cancer Survivorship Program, please contact Dr. Goldfarb at 310-829-8751.
About the Author

Zara Jethani
Zara is the marketing director at Pacific Neuroscience Institute. Her background is in molecular genetics research and healthcare marketing. In addition, she is a graphic designer with more than 20 years experience in the healthcare, education and entertainment industries.
Last updated: April 16th, 2021