

Patient Story: Malia’s Brain AVM Changed the Course of her Life
by Robin Banuelos
MEET MALIA
Malia’s life changed in 2017 while on a college tour with her mother in Seattle, Washington.
They were preparing for her next chapter in life as a 17-year-old junior in high school. This is a time when parents hope their healthy children can focus on prom preparation, college applications, and visions of their future. Meanwhile, Malia’s mother awoke one night to witness her daughter violently shaking in her sleep. Malia was affected by a grand mal seizure which, in this occurrence, included loss of consciousness and rapid involuntary muscle contractions.

Upon returning to their home in Los Angeles, California, Malia’s family received the foundational diagnosis of an arteriovenous malformation (AVM) in her brain. Her neurologist immediately referred her family to Dr. Walavan Sivakumar, Director of Neurovascular Surgery. They entrusted Pacific Neuroscience Institute – South Bay in Torrance, California to provide the highest quality and care. Her treatment was complex yet ultimately successful. Approximately 4 years later, the impact of this life-altering experience influenced Malia to join Dr. Sivakumar’s research team as they currently work to improve outcomes for future patients.
“I was not conscious during the seizure and have no memory of it. I didn’t know what to think when I heard the diagnosis for the first time. It was daunting but Dr. Sivakumar reassured me that I was in good and experienced hands.“
Malia
WHAT IS AN AVM?
Time is of the essence.
AVMs are a vascular malformation in which arteries and veins, the vessels that circulate oxygenated nutrient-rich blood throughout the heart and body, become entangled within the brain’s tissue. Thus, Malia’s seizure was likely provoked by a circulatory blood disruption.
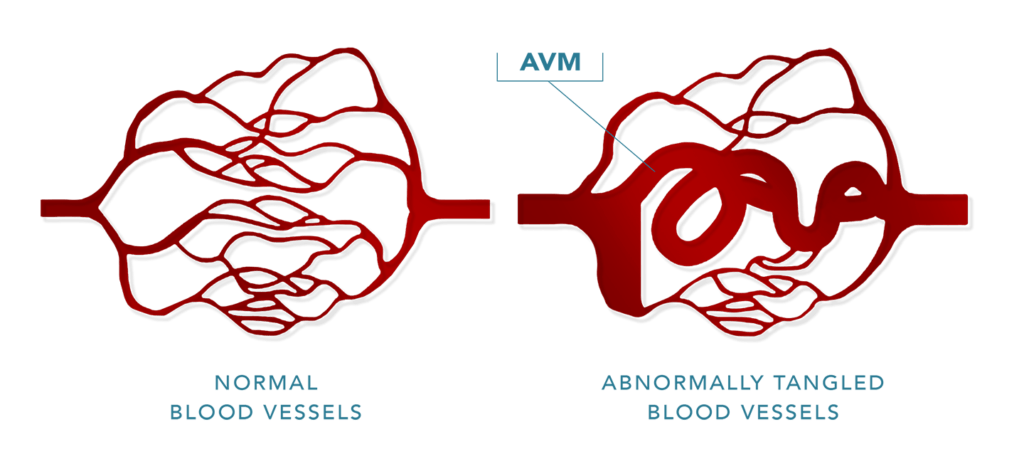
This unusual abnormality generally affects less than 1% of the population and most people who have AVMs are asymptomatic (experiencing no symptoms) throughout their lifetime. However, 12% of these individuals experience symptomatic problems, such as Malia.
Her parents, who are physicians themselves, understood the urgency of this diagnosis. Delayed treatment could progress toward permanent brain damage or become life-threatening in the emergence of other conditions:
- Brain Hemorrhaging: While there are several types of strokes, a hemorrhagic stroke occurs when weakened blood vessels rupture causing localized bleeding in the brain. Healthy blood supply becomes interrupted and brain cells rapidly die within minutes.
- Hydrocephalus: Significant pressure becomes placed on the skull and ventricles, the brain’s cavities, due to fluid-accumulation of blood causing hydrocephalus. Excessive pressure potentially leads to long-term problems such as learning disabilities, vision problems, and declining physical coordination.
AVM TREATMENT
Dr. Sivakumar promptly called an interdisciplinary cerebrovascular conference of PNI’s Stroke and Neurovascular Team.

All aneurysms, arteriovenous malformations, and cavernous malformations are presented to PNI’s interdisciplinary neurovascular group to formulate the best treatment plan for each unique patient.
Malia’s personal team of experts, led by Dr. Sivakumar, understood that her pediatric age required additional measures in approaching treatment options. Further, her team conducted extensive research and consulted with their vast network of expert colleagues from around the world before a surgical treatment was properly selected.
In spite of this comprehensive process, Dr. Sivakumar compassionately coordinated around Malia’s school schedule to reduce interruption. He additionally provided her family with current educational literature regarding AVM. He and his team left no stone unturned in their operative preparation.
To make surgery safer, Malia’s team began by performing a series of embolizations, a minimally invasive treatment which blocks abnormal vascular channels – thereby reducing blood flow to the malformation. During the second of 3 embolizations, the AVM unexpectedly bled and Malia was urgently rushed to the dedicated Neuro-Critical Care Unit at Providence Little Company of Mary Medical Center Torrance. Now considered an urgent case, Dr. Sivakumar carefully worked for 5 hours meticulously disconnecting and entirely removing the AVM. Dr. Garni Barkhoudarian, co-surgeon with Dr. Sivakumar, described the surgery as highly complex due to firmly interweaving blood vessels.
Malia returned home 3 days later, neurologically intact and on her way to a complete recovery.
The encompassing empathy and warmth expressed by every member of PNI – South Bay’s medical and administrative team, from beginning to end, astounded Malia and her family. They remain forever grateful to Dr. Sivakumar for saving Malia’s life.
SUCCESSFUL AVM RESULTS
“The team made sure I understood everything in detail with the best care. This experience showed me how much I can actually handle in life. I am thankful for Dr. Sivakumar, his team, access to good healthcare, and the fact that this condition did not debilitate me. I don’t even have social repercussions because no one can see the scar. Life has returned to normal!”
Malia

Her recovery was extraordinary immediately following the surgery. She was cleared to drive within weeks and has experienced no recurring seizures nor signs of long-term learning disabilities. Malia’s follow-up imaging studies continually present complete eradication of the AVM with no indication of return. Furthermore, she has successfully stopped related medications. Malia has resumed the next chapter of life as an independent young woman.
She is now attending Dr. Sivakumar’s alma mater, University of California, Los Angeles (UCLA), one of the most competitive universities in the United States. Moreover, Malia’s experience with PNI inspired her to assist Dr. Sivakumar in research focused on the improvement of patient outcomes after brain surgery. She spends her spare time with loved ones and volunteering among special needs communities.

“Malia has always been an intelligent, kind, and dedicated young woman – but this experience changed her life and she has decided to pursue a future that helps others in the way that our team did for her. We are proud of her.”
Dr. Walavan Sivakumar
About Dr. Walavan Sivakumar

Dr. Walavan Sivakumar, is a fellowship-trained neurosurgeon with a focus on skull base and minimally invasive and endoscopic neursosurgery. A multiple Super Doctor award recipient, Dr. Sivakumar has a particular interest and expertise in brain tumors, skull base tumors, pituitary/parasellar tumors, and intraventricular brain tumors, and he applies the keyhole concept, utilizing advanced neuroimaging and microsurgical techniques to minimize collateral damage to the brain. Dr. Sivakumar’s practice includes treating patients with brain, skull base, and pituitary tumors, aneurysms, cavernous malformations, arteriovenous malformations, carotid stenosis and spine issues. He has clinics at both Providence Little Company of Mary Medical Center Torrance and Providence Saint John’s Health Center in Santa Monica.
Useful Links
- Arteriovenous Malformation (AVM)
- Pacific Stroke & Neurovascular Center
- Providence Little Company of Mary
Clinic Information
Pacific Neuroscience Institute – South Bay
Providence Little Company of Mary Medical Center Torrance
5215 Torrance Blvd., #300,
Torrance, CA 90503
424-212-5361
4201 Torrance Blvd., #520,
Torrance, CA 90503
424-212-5340
About the Author

Robin Banuelos
Robin Banuelos is an administrative coordinator at Pacific Neuroscience Institute South Bay, located at Providence Little Company of Mary Torrance. A skilled project manager and graphic designer, she works with Dr. Walavan Sivakumar providing a wide array of support to the Neurovascular and Neurosurgical teams.
Last updated: November 19th, 2021