Glioblastoma Awareness Day: Confronting the Challenges of a Devastating Brain Tumor
Updated July 1, 2025
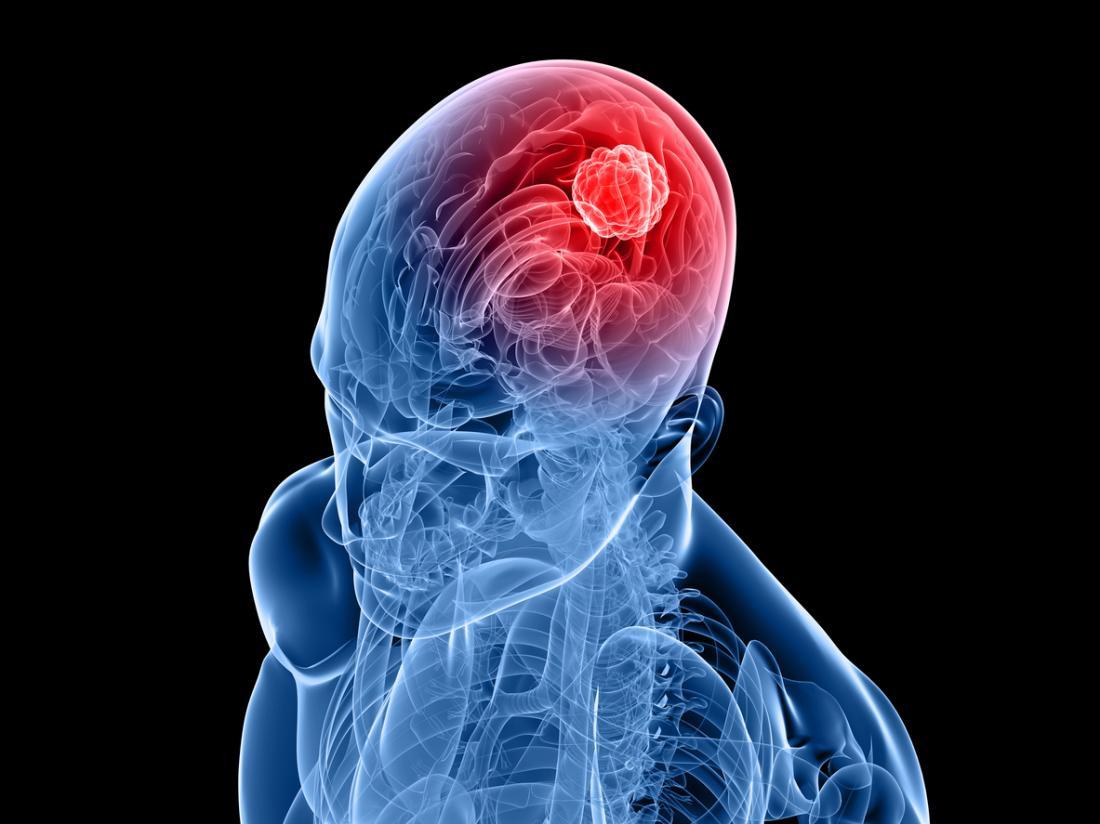
The third Wednesday of each July is Glioblastoma Awareness Day. Glioblastoma (GBM) is a complex and invasive form of brain cancer, presenting difficulties in its treatment. Notably, it has come to public attention in the past years with Beau Biden, Ted Kennedy, and John McCain, succumbing to the disease shortly after diagnosis.
In this article, we explore this complex brain tumor.
What is Glioblastoma?
Types of GBM
According to PNI neuro-oncology specialists, there are two types of glioblastomas: primary, originating de novo, and secondary, evolving from lower-grade gliomas. Patients diagnosed with these tumors generally have a difficult prognosis and poor quality of life as the disease progresses. In the United States, an estimated 13,000 patients are diagnosed with GBM annually, with a life expectancy of about 14 months, and a 5-year survival rate of 5%. The incidence increases significantly after the age of 54 and reaches a peak incidence at age 75-84 years.
Symptoms of GBM
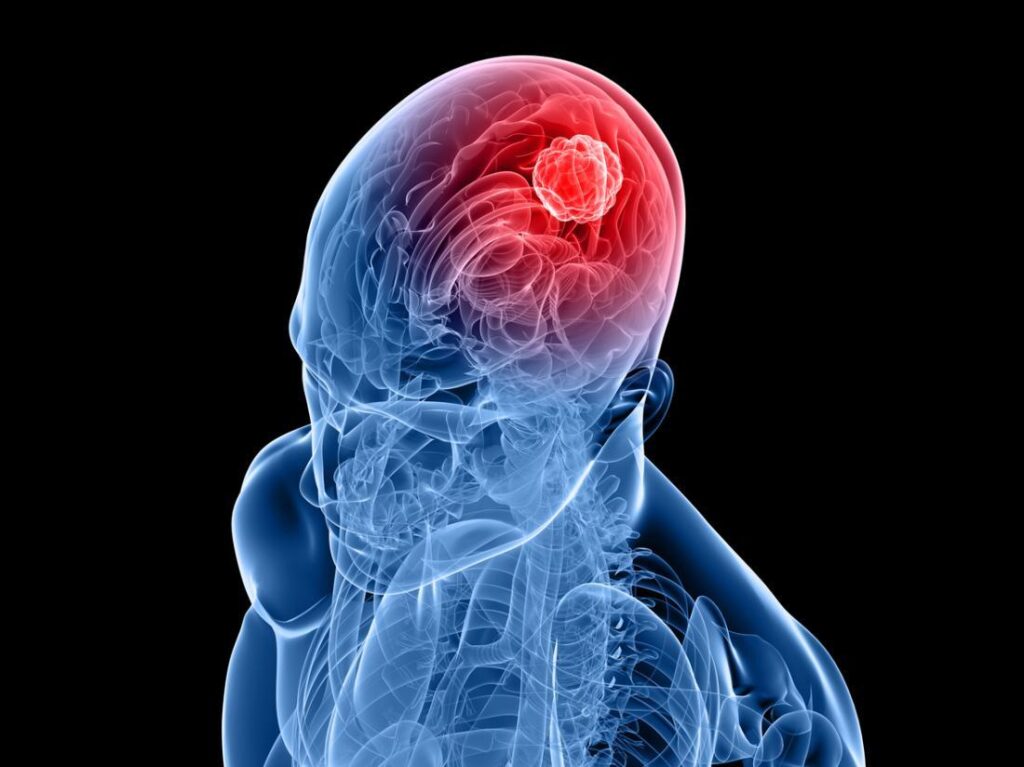
One of the most common symptoms is a headache, which differs from a typical tension or migraine headache. Other symptoms which may occur alone or in combination include persistent weakness, numbness, blurred vision, balance issues, seizure, changes in memory, or alteration of language.
In a vast majority of patients, there is no cause of the disease, but we presume there is an initial molecular event in a cell that starts to become cancerous. The only well-established causative factor for GBM is exposure to ionizing radiation, but this accounts for only a small minority of cranial tumors. Currently, MRI imaging provides the most sensitive tool for the initial detection of GBM; however once a GBM is identified, the tumor is already at an advanced state.
The standard of care therapy consists of debulking surgery, followed by radiation and temozolomide chemotherapy. The radiation and chemotherapy agent damages the DNA in tumor cells that are actively dividing.
Why is glioblastoma difficult to treat?
- Heterogeneity: There is a high degree of variation (heterogeneity) within the same tumor cells that makes each individual glioblastoma molecularly distinct. This can be challenging when predicting prognosis and treatment
- Location of tumor: If the tumor is located in a region that is hard to reach, or too near vital blood vessels or crucial brain regions, it can render surgery high-risk or impossible.
- Recurrence: GBM tumors have a tendency to come back aggressively.
Our experts explain that the challenge in treating brain tumors lies in addressing inactive tumor cells, which are dormant. These cells, known as cancer stem cells, evade radiation and chemotherapy by remaining inactive.
Coping with a Glioblastoma Diagnosis
Few cancers are as challenging as glioblastomas. Although no cure currently exists for these brain tumors, patients and care partners can take steps to enhance their quality of life after receiving a diagnosis.
Palliative care physicians possess extensive knowledge in this area. Everything happens very fast, and it can be very overwhelming. Neuro-oncology specialists say for example that patients may feel fine when suddenly they experience a seizure and are told that they have a big mass in their brain. They are rushed into surgery and there is a lot of information to process. There are many different aspects to consider with a diagnosis and the realities of glioblastoma.
With the objective to create an open and safe environment where patients can engage in meaningful conversations, PNI experts try to facilitate candid dialogue between patients and their loved ones. The goal is for patients to cherish and create new memories while maximizing their time. Furthermore, the doctors strive to align treatment with patient goals and provide comprehensive care, which encompasses thorough symptom assessment and management, as well as support for the patient’s family and friends.
Clinical Trials and Research for Glioblastoma
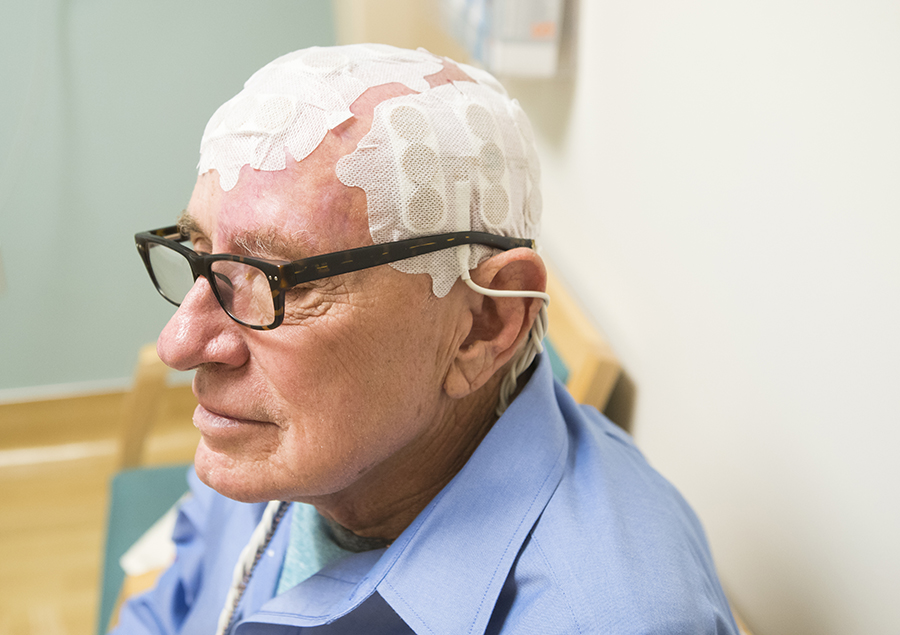
Our team has significantly advanced research and treatment for glioblastoma by developing methods that target and destroy cancer cells. Clinical trials are conducted at Saint John’s Cancer Institute and Pacific Neuroscience Institute. These are new treatment approaches for those who are newly diagnosed with glioblastoma, and those who have recurrent disease.
There is a need for better therapies in brain cancer patients, and by studying the molecular genetic of patients, I believe we are on the verge of getting there. Many of these challenges are currently being studied in clinical trials and by having an understanding of glioblastoma we hope to soon have a cure. There is a need for better therapies in brain cancer patients, and by studying the molecular genetic of patients, our experts believe we are on the verge of getting there. Many of these challenges are currently being studied in clinical trials and by having an understanding of glioblastoma we hope to soon have a cure. There is a need for better therapies in brain cancer patients, and by studying the molecular genetic of patients, our experts believe we are on the verge of getting there. Many of these challenges are currently being studied in clinical trials and by having an understanding of glioblastoma we hope to soon have a cure.
The Cancer Moonshot
The Cancer Moonshot was launched in 2016 by National Cancer Institute to accelerate scientific discovery in cancer research, foster greater collaboration, and improve the sharing of cancer data. It has brought together a large community of patients, advocates, researchers, and clinicians who are dedicated to advancing research to end cancer as we know it.
GBM Awareness Day
The aim of Glioblastoma Awareness Day is to honor those who live with glioblastoma and showcase the fortitude of patients and caregivers. Additionally, it is an opportunity to support and acknowledge the tireless efforts of medical professionals and researchers in seeking a cure.
For GBM Awareness Day, we encourage you to use the #GBMAwareness hashtag to amplify the need for increased research funding.

