
Case Study: Meningioma Brain Surgery Restores Patient’s Vision
by Amelia Garrison
Progressive Vision Loss Leads to a Brain Tumor Diagnosis

When a 52-year-old woman from New York began experiencing progressive vision loss in her left eye, she knew she needed medical help. After seeing both an optometrist, she underwent MRI imaging and was referred to Pacific Neuroscience Institute (PNI) for specialized care.
“That MRI showed an approximately two-and-a-half by two centimeters, extra-axial brain tumor situated at the tuberculum sellae, which is a very common location for meningiomas,” explained Dr. Daniel F. Kelly, Director and one of the founders of PNI.
Understanding Meningiomas
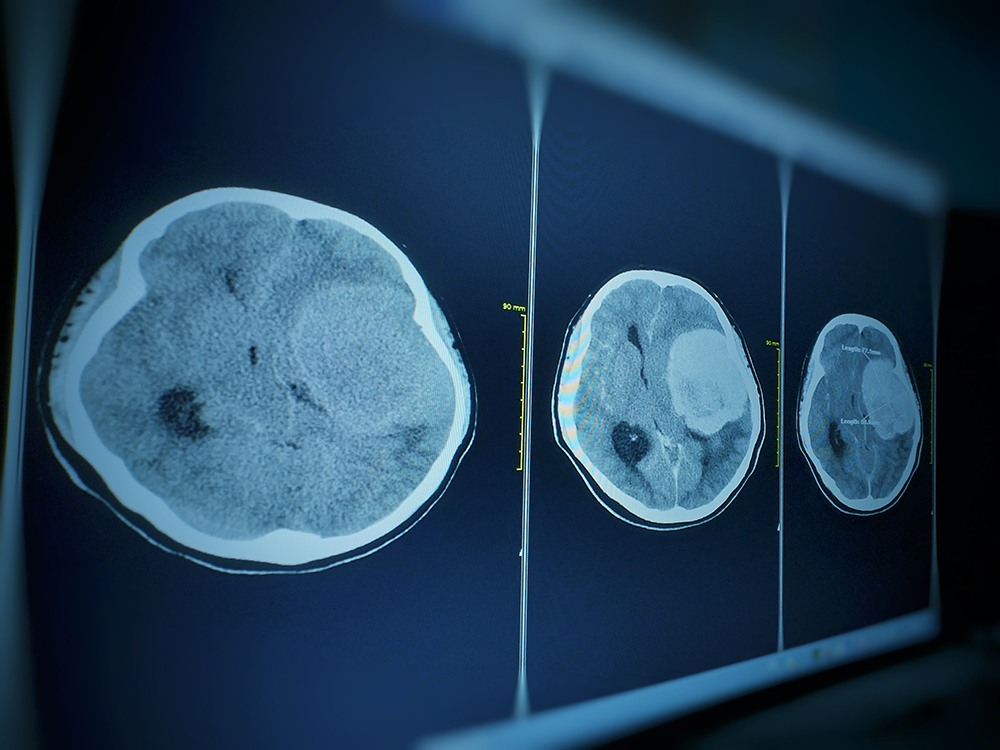
Meningiomas are typically benign (noncancerous) brain tumors that arise from the membrane (the “meninges”) surrounding the brain and spinal cord. They occur most commonly in adults between the ages of 40 and 70 and are more frequently diagnosed in women.
Although meningiomas are typically benign, they can compress vital brain structures, leading to significant symptoms such as vision loss, double vision, facial pain, difficulty swallowing, and hearing loss.
Depending on their size and location, meningiomas may also cause personality changes, seizures, motor weakness in the arms or legs, loss of sensation, spatial disorientation, and visual field deficits. These symptoms occur when the tumor places progressive pressure on surrounding brain tissue.
Meningiomas are often diagnosed incidentally by patients who receive an MRI for headaches or dizziness. First-line treatment for symptomatic meningiomas is maximal safe surgical removal, while second-line treatment may include focused radiotherapy or radiosurgery.
Removing the Meningioma & Restoring Vision
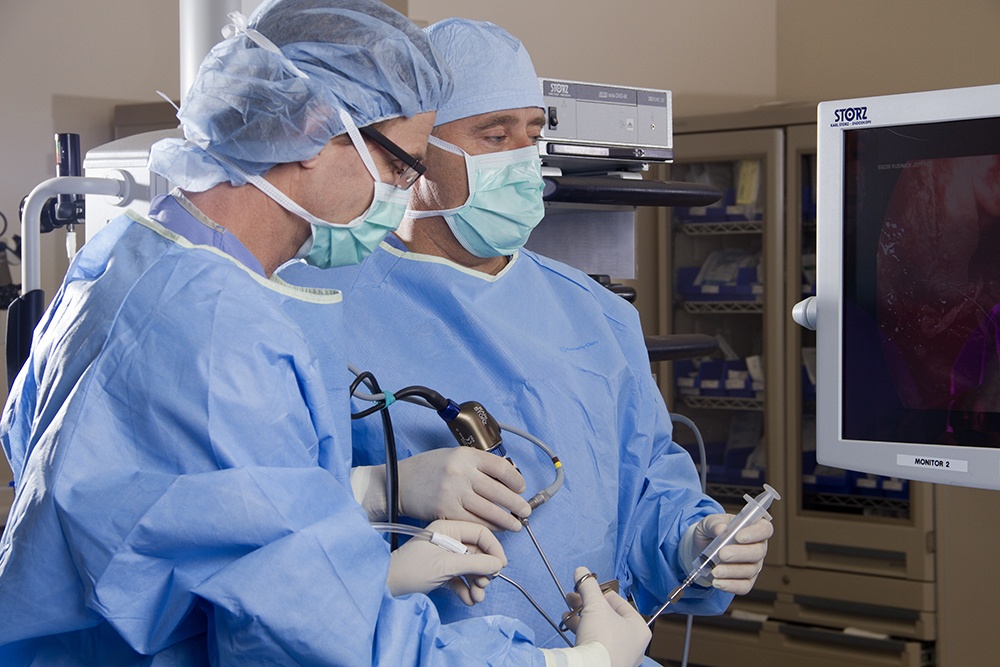
In this particular case, the meningioma was located in the patient’s left optic canal, causing progressive vision loss. Dr. Kelly and Dr. Chester F. Griffiths, Director of the Eye, Ear & Skull Base Center and Co-Founder of PNI, performed minimally invasive surgery to remove the tumor.
“Given the optic canal invasion and her primary complaint being also vision in the left eye, we approached this tumor through the endoscopic endonasal route,” recalled Dr. Kelly. “With my partner in ENT, Dr. Chester Griffiths, we were able to achieve a gross total tumor removal.”
The successful removal of the tumor restored the patient’s vision, and she recovered in just two days at Providence Saint John’s Medical Center.
A Rapid Recovery With Minimally Invasive Brain Surgery

At PNI, minimally invasive surgery enables patients to leave the hospital sooner and recover more comfortably.
“The goal here is to limit collateral damage to the surrounding tissues and to allow the patient to have a rapid recovery with less brain exposure, less manipulation, smaller incisions, our patients seem to have less pain,” explained Dr. Kelly.
He continued, “Our typical hospital stay for some brain tumors is one night in the hospital. Most are out by two days and rarely do they go a little bit beyond that. These [minimally invasive] approaches have multiple benefits for the patient, so we will continue to try and push the envelope on these approaches and make them even more safe and effective than they are now.”
Long-Term Follow-Up and Ongoing Monitoring
Drs. Kelly and Griffiths have followed the patient closely since her surgery.
“She’s doing great with no evidence of recurrence of the tumor and her vision is normal. And her pituitary gland function is normal and she has a normal sense of taste and smell,” Dr. Kelly explained.
To learn more about meningioma surgery, or to get a second opinion about a newly diagnosed or recurrent meningioma, visit the meningioma page on the Pacific Brain Tumor Center, or call 310-582-7450.
Frequently Asked Questions About Meningioma Surgery and Vision Loss
Can a brain tumor cause vision loss?
Yes. Brain tumors such as meningiomas, especially those located near the optic nerves or optic canal, can compress the visual pathways and cause progressive vision loss, double vision, or visual field defects. Early diagnosis and treatment are critical to preserving or restoring vision.
Can vision be restored after meningioma surgery?
In many cases, vision can improve or fully recover after surgical removal of a meningioma, particularly when the tumor is treated before permanent optic nerve damage occurs. Outcomes depend on tumor size, location, and duration of symptoms prior to surgery.
What is minimally invasive endoscopic brain surgery?
Minimally invasive endoscopic brain surgery uses small natural openings, such as the nasal passages (endonasal approach), along with high-definition cameras and specialized instruments to access and remove tumors. This approach reduces brain manipulation, shortens recovery time, and often results in less pain and fewer complications compared to traditional open surgery.
How long is recovery after minimally invasive meningioma surgery?
Many patients undergoing minimally invasive meningioma surgery are discharged within one to two days and return to normal activities sooner than with traditional surgery. Recovery time varies depending on the tumor and individual patient factors.
Can meningiomas come back after surgery?
While many meningiomas are successfully removed, long-term follow-up with periodic MRI scans is important. Recurrence risk depends on the tumor’s grade, location, and extent of removal. Regular monitoring helps detect any regrowth early.
When should I seek a second opinion for a meningioma?
A second opinion is recommended if you have been newly diagnosed, if your tumor has recurred, or if you are experiencing symptoms such as vision loss or neurological changes. Specialized centers like Pacific Neuroscience Institute can offer advanced surgical options and multidisciplinary evaluation.
About Dr. Daniel Kelly

Daniel F. Kelly, MD, is the Director of the Pacific Brain Tumor and Pituitary Disorders Centers at Pacific Neuroscience Institute. Considered to be one of the top neurosurgeons in the U.S., Dr. Kelly is internationally recognized in the field of minimally invasive keyhole surgery for brain, pituitary, and skull base tumors. He continues to focus his efforts on advancing innovative treatments for patients, providing fellowship training in minimally invasive neurosurgery, and patient education and support.
About Dr. Chester Griffiths

Chester F. Griffiths, MD, FACS, is board certified in Otolaryngology, Head and Neck Surgery, and Facial Plastic and Reconstructive Surgery. He has 30 years of experience in endoscopic endonasal sinus surgery for skull base tumors and pituitary tumors, sinonasal cancers including mucosal melanomas, and in the treatment of facial and nasal trauma, cosmetic deformities, sinus infections, and disorders of smell and taste. His practice treats sleep apnea, snoring, difficulty breathing, disorders of the larynx, thyroid tumors, and other head and neck cancers with an emphasis on viral HPV-related cancers.
Related Links:
About the Author

Amelia Garrison
Amelia Garrison is the Marketing Specialist at Pacific Neuroscience Institute (PNI). Well versed in community outreach strategy and implementation, she leads the PNI blog, newsletter, and digital communications. Amelia oversees PNI's reputation management and community sponsorships.
Last updated: February 25th, 2026