Intracranial Meningioma: Understanding the Most Common Type of Brain Tumor
Learn about the symptoms, diagnosis, and treatment for intracranial meningiomas, the most common type of benign brain tumor.
With more than 120 different types of brain tumors, it can be difficult to differentiate between benign and malignant brain tumors. At Pacific Brain Tumor Center at Pacific Neuroscience Institute (PNI) our team of highly-skilled radiation oncologists, neuro-oncologists, medical oncologists, and neurosurgeons, are experts in diagnosing and treating both benign and malignant brain tumors.
Brain tumors are masses of abnormal growth in the tissues of the brain. Brain tumors can be benign (non-cancerous) or malignant, meaning that they have cancer cells that grow rapidly. Brain tumors that start in the brain are called primary brain tumors, while tumors that start elsewhere in the body and move to the brain are called metastatic brain tumors.
What is an intracranial meningioma?
There are many manifestations of meningioma. Intracranial meningiomas are primary brain tumors, meaning that they originate within start in the brain rather than spreading from another area of the body. They are the most common type of benign brain tumor that develops or arises from any meningeal surface of the brain. Intracranial meningiomas are typically attached to the dura (outer layer of the meninges), but can also occur in the cerebral ventricles.
What are the symptoms of an intracranial meningioma?
Because intracranial meningiomas can form in different areas of the brain, the resulting symptoms vary depending on their size and location. Common symptoms include:
- Vision loss
- Double vision
- Headache
- Seizure
- Problems with balance or coordination
- Difficulty swallowing
- Hearing loss or ringing in the ears
If you or a loved one suspects that you may have a brain tumor, it is essential to seek medical attention promptly. Early detection improves outcomes and guides the best meningioma treatment plan.
Diagnosis and Evaluation
Before recommending surgical resection or radiation, physicians perform advanced imaging studies such as MRI or CT scans to determine tumor grade and location. At PNI’s Pacific Brain Tumor Center, our experts use high-resolution imaging and neuronavigation to evaluate whether an intracranial meningioma is typical, atypical meningioma, or anaplastic meningioma. This precision guides the best individualized treatment strategy and helps predict the likelihood of meningioma recurrence.
What is the best treatment for an intracranial meningioma?
Optimal treatment for intracranial meningiomas is determined by the location. However, in virtually all symptomatic meningiomas, the treatment is surgical removal.
At PNI, our surgeons have extensive experience performing minimally invasive keyhole procedures to remove intracranial meningiomas, preserving healthy brain tissue and reducing recovery time. Surgical approaches include:
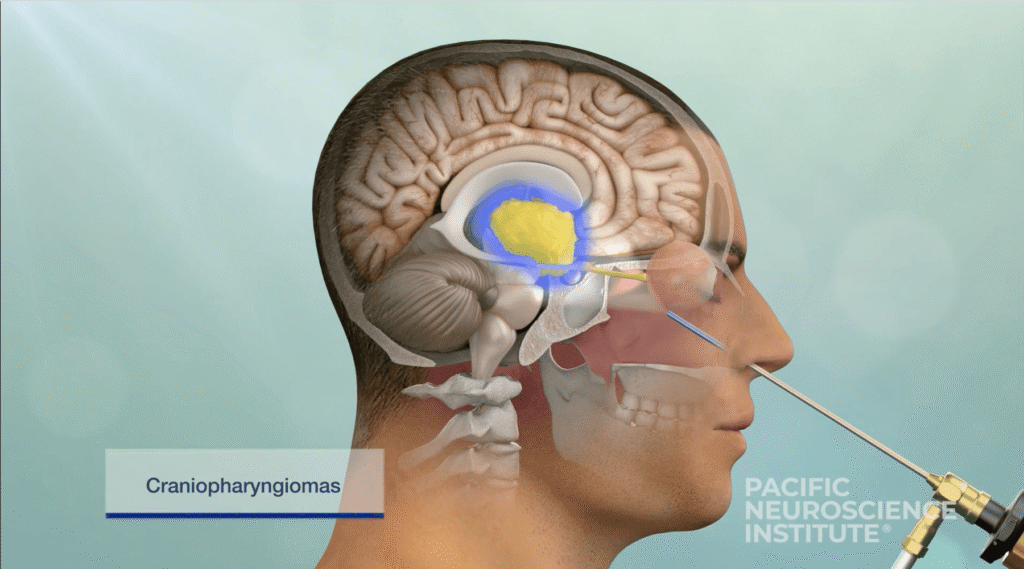
- Endoscopic endonasal approach (through the nostrils)
- Superorbital eyebrow approach (through a small incision through the eyebrow)
- Minipterional approach (an incision just behind the hairline)
- Transorbital approach
Other approaches include behind the ear and along the top of the head, depending upon where the tumor occurs.
What happens if an intracranial meningioma is not entirely removed?
The goal is always maximal safe removal. In some cases, since meningiomas may be very adherent to some of the cranial nerves, the brain itself, or critical blood vessels, we have to leave behind a small amount of the tumor. We do that to ensure that the patient comes out of surgery better than they went in, preserving the quality of life and not with new neurological problems. When a small portion must be left behind, focused radiation therapy may be recommended.
Fortunately, most meningiomas are radiosensitive, meaning that they can respond well to focused radiation treatment. In these cases, stereotactic radiosurgery or fractionated radiation can prevent meningioma recurrence while preserving neurological function.
Overall, the diagnosis of meningioma, although somewhat scary, is one that can be dealt with very effectively in skilled hands using keyhole and minimally invasive approaches. The Pacific Brain Tumor Center specializes in keyhole and minimally invasive approaches that promote faster recovery and excellent long-term outcomes.
About Pacific Brain Tumor Center
At the Pacific Brain Tumor Center at Pacific Neuroscience Institute, our multidisciplinary team offers some of the world’s largest experiences in minimally invasive surgery and non-surgical treatment for brain tumors such as meningiomas, including novel therapies and clinical trials. Our collaborative approach, uniting radiation oncologists, neuro-oncologists, medical oncologists, and neurosurgeons, ensures each patient receives a customized, evidence-based meningioma treatment plan. We emphasize patient education, compassionate care, and ongoing support to improve long-term health and quality of life.
If you, a family member, or a friend have been diagnosed with a brain or skull base tumor, our team of experts is here to provide help and guidance. We provide comprehensive care for these challenging problems as well as patient education and psychosocial support.

