Intraventricular Tumor
What is an Intraventricular Tumor?
Overview
Intraventricular tumors are a diverse group of benign or malignant tumors that originate within the ventricles of the brain, which are fluid-filled spaces responsible for the production and circulation of cerebrospinal fluid (CSF).
The cerebrospinal fluid bathes the brain and spinal cord. It is produced by the choroid plexus and has no “off switch.” Tumors in the ventricles can block flow regionally, resulting in build-up of fluid and pressure.
There are various types of intraventricular tumors, including ependymomas, choroid plexus tumors, central neurocytomas, subependymal giant cell tumors, and others. Each of these tumors arises from different types of cells within the ventricles, leading to distinct clinical presentations, characteristics, and treatment approaches.
Minimally invasive endoscopic keyhole surgery is now possible for most intraventricular tumors. In some cases, small tumors may be safely monitored with regular imaging. In others, a biopsy or surgical removal is needed for diagnosis and treatment.
Types of Intraventricular Tumors
Ependymomas are one of the most common types of intraventricular tumors. They originate from ependymal cells that line the ventricles. Ependymomas can occur at any age but are more frequently diagnosed in children and young adults. These tumors can obstruct CSF flow, leading to increased intracranial pressure and symptoms such as headaches, nausea, vomiting, and visual disturbances. Surgical resection is the primary treatment for ependymomas, often supplemented with radiation therapy.
Choroid plexus tumors arise from specialized cells that produce CSF within the ventricles. They are more commonly found in infants and children. Choroid plexus papillomas are typically benign, whereas choroid plexus carcinomas are malignant. These tumors can cause overproduction of CSF, leading to hydrocephalus and associated symptoms. Surgical resection followed by chemotherapy or radiation therapy is the standard treatment approach.
Central neurocytomas are rare tumors that primarily affect young adults. They arise from neuronal cells within the ventricles. These tumors are usually slow-growing and may cause symptoms such as headaches, seizures, and cognitive changes. Surgical resection is the primary treatment, and adjuvant therapies may be considered in cases with residual or recurrent tumors.
Subependymal giant cell tumors (SEGAs) are benign tumors that often develop in individuals with tuberous sclerosis, a genetic disorder. SEGAs arise from cells lining the walls of the ventricles. These tumors can lead to hydrocephalus and may cause neurological symptoms. Surgical resection or targeted therapy with mTOR inhibitors is typically employed.
Who is Affected?
Intraventricular tumors can occur at any age. Some types, such as choroid plexus tumors, are more common in children, while others, like central neurocytomas, are more frequent in young adults. Genetic conditions such as tuberous sclerosis can increase the risk of specific tumor types like SEGAs.
Intraventricular Tumor Symptomsrn& Causes
Symptoms
Symptoms of these tumors/cysts vary depending on their type and location amongst the ventricular system.
Typical symptoms include:
- Headache
- Vision loss or double vision
- Memory loss
- Imbalance
- Swallowing difficulties
- Hoarse voice
These symptoms can take years to develop, but can worsen suddenly, progressing to altered mental status and coma if left untreated.
Causes
The exact cause depends on the tumor type. Factors can include:
- Genetic mutations affecting cell growth regulation.
- Inherited syndromes such as tuberous sclerosis.
- Sporadic cell changes within the ventricular lining or choroid plexus.
- In rare cases, metastatic spread from cancers elsewhere in the body.
When to See a Doctor
Seek immediate medical attention if you or a loved one experiences:
- Persistent or severe headaches
- Sudden vision changes
- Unexplained balance problems
- Episodes of confusion or memory loss
- Rapidly worsening neurological symptoms
Early diagnosis and treatment can help prevent permanent brain damage and improve outcomes.
Intraventricular Tumor Diagnosis
As the treatment(s) of these lesions vary greatly on the diagnosis, numerous tests may be necessary prior to surgery.
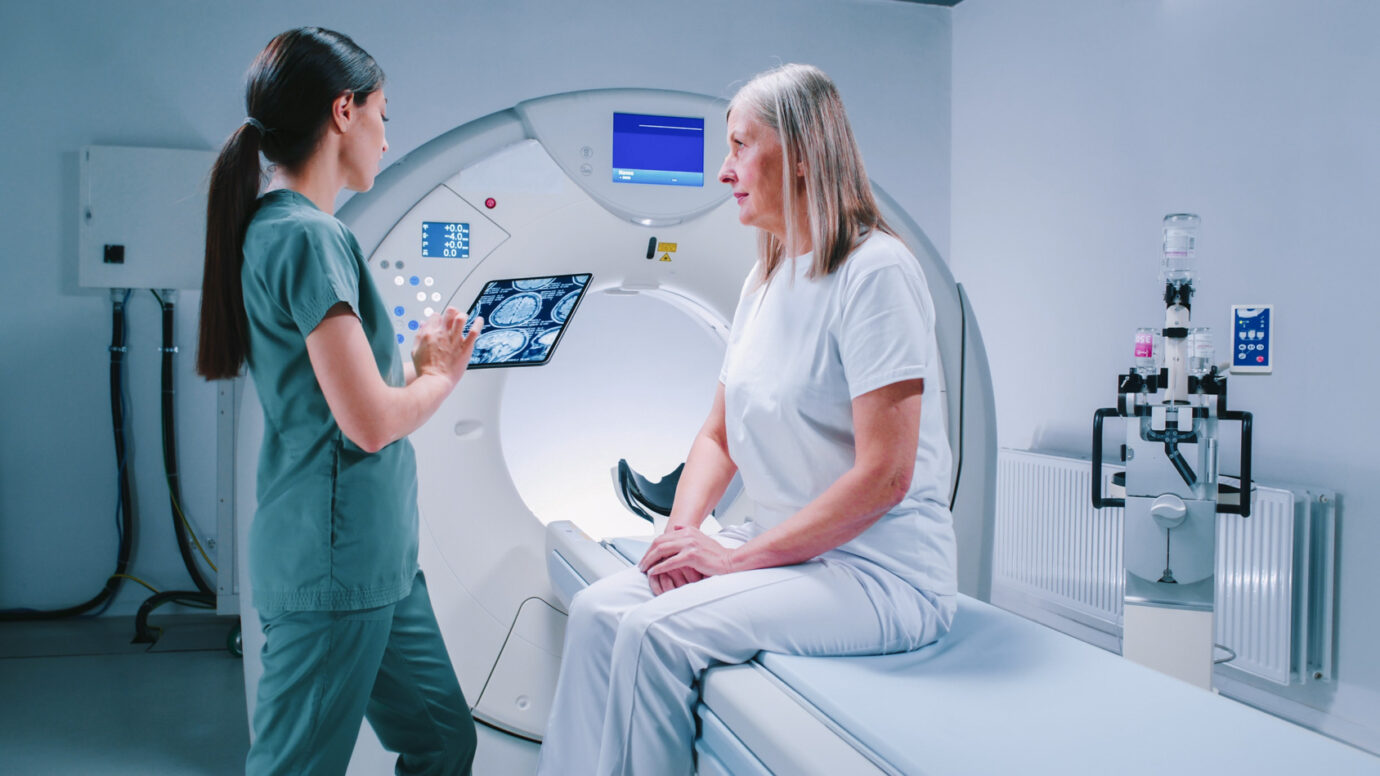
Imaging
Typical imaging studies include magnetic resonance imaging (MRI) or computer tomography (CT) scans of the brain. Fiber tractography MRI (DTI) is helpful to assess key neural fibers as well as surgical approach.
Lumbar Puncture
The cerebrospinal fluid (CSF) may need to be analyzed via a lumbar puncture (spinal tap) if deemed safe.
Surgical Biopsy
In select cases, surgical biopsy to obtain tissue may be necessary prior to definitive therapy.
Intraventricular Tumor Treatmentrn& Outcomes
Treatment Options
Most intraventricular tumors can be treated with minimally invasive surgical approaches. The surgical approach is dependent on the tumor type, size and location specific to the ventricle.
- For small tumors in the lateral and third ventricles, direct endoscopic biopsy and resection is possible.
- For larger tumors, a brain-port is helpful for better tumor access and control.
- For 4th ventricle tumors, a suboccipital approach is utilized, with endoscopic assistance when necessary.
- For hydrocephalus management, occasionally an endoscopic third ventriculostomy is necessary to treat the hydrocephalus while a diagnosis or definitive adjuvant therapy is prepared.
Patient Outcomes
Outcomes vary depending on tumor type, grade, and how completely it can be removed. Many benign tumors have an excellent prognosis when fully resected, while malignant tumors may require ongoing therapy and monitoring. Advances in imaging, navigation, and endoscopic techniques have significantly improved surgical safety and long-term results.
Managing An Intraventricular Tumor
Living with or recovering from an intraventricular tumor may involve:
Follow-Up MRIs
Regular follow-up MRIs to monitor for recurrence.
Rehabilitation Therapy
For speech, balance, or motor function if affected.
Medication
Medication adherence if prescribed targeted therapy or seizure prevention drugs.
Healthy Lifestyle
Maintaining a healthy lifestyle to support recovery, including good sleep, balanced nutrition, and gentle exercise.
Meet our Expert Specialists & Surgeons
Experience Compassionate, Expert Care

At Pacific Neuroscience Institute, we treat the full range of intraventricular tumors including gliomas, metastatic tumors, central neurocytomas, subependymal giant cell astrocytomas (SEGA), meningiomas, ependymomas, subependymomas, germinomas and germ cell tumors, choroid plexus papillomas and carcinomas, and medulloblastomas (PNET).
Our team combines advanced microsurgical and minimally invasive techniques with decades of experience in brain tumor surgery. Using high-definition imaging, precision navigation, and intraoperative monitoring, we strive to make intracranial tumor surgery safer, less invasive, and more effective—while providing the personalized, compassionate care every patient deserves.
Learn More About anrnIntraventricular Tumor
The prognosis depends on tumor type, size, grade, and treatment success. Benign tumors such as central neurocytomas or choroid plexus papillomas often have excellent long-term outcomes after complete removal. Malignant tumors may require additional therapies and closer follow-up but can still be managed effectively in many cases.
Ependymomas and choroid plexus tumors are among the most common intraventricular tumors, though prevalence varies by age group.
Common symptoms include headaches, nausea, vomiting, vision changes, balance problems, memory issues, and in severe cases, altered consciousness due to hydrocephalus.
Survival rates vary greatly by tumor type. Benign tumors have high survival rates—often above 90% after full resection—while malignant tumors have more variable outcomes, typically requiring additional treatment.
Treatment often involves minimally invasive endoscopic surgery to remove the tumor, sometimes combined with chemotherapy or radiation therapy depending on the tumor type.
These tumors are located within the brain’s ventricular system—fluid-filled spaces that produce and circulate CSF.
Resources

Get Expert Care from Leading Specialists
If you’ve been diagnosed with an intraventricular tumor, our expert neurosurgeons at Pacific Neuroscience Institute are here to help. We use advanced imaging and minimally invasive techniques to provide safe, effective treatment with faster recovery times.
Written and reviewed by:
The Pacific Neuroscience medical and editorial team
We are a highly specialized team of medical professionals with extensive neurological and cranial disorder knowledge, expertise and writing experience.
Last Updated:




