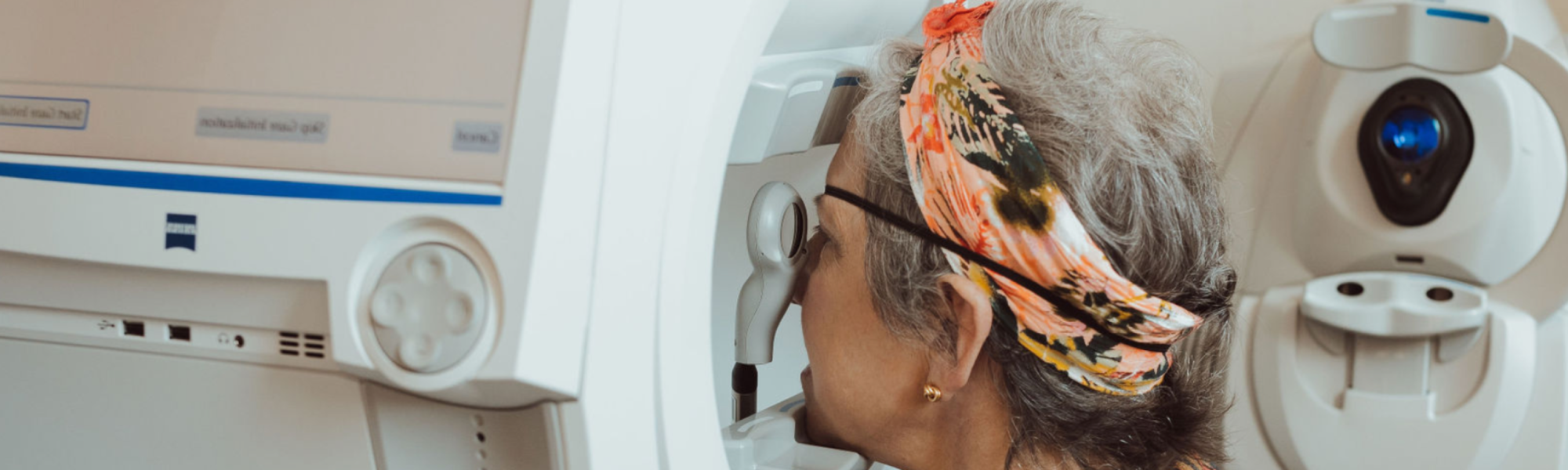
Eye & Vision
Ophthalmologists in Santa Monica
Ophthalmologists and our eye team at the Pacific Eye, Ear & Skull Base Center offer eye and vision treatment for a broad array of ocular issues, with special emphasis and expertise in Neuro ophthalmology, Adult Strabismus Surgery and Orbital Surgery.
Neuro-ophthalmology, in essence, is everything to do with eyes and vision secondary to problems outside the eye, such as eyelid disorders, ocular and orbital pain, double vision, neurologic or brain disorders, circulatory disorders and inflammation, injury and tumors of the eye socket (orbit), or face, head, or brain. We evaluate, diagnose and treat these disorders, often in concert with our PNI colleagues of multiple specialties.
We also offer comprehensive ophthalmic services, as well as the more complex specialty procedures including oculoplastic surgery, adult strabismus surgery and orbital and anterior skull base surgery. Our specialists deliver the best eye care and vision solutions while considering the needs and preferences of our patients.

Vision Conditions We Treat
Our specialists treat a board range of diseases that affect the eye.
Our Team of Ophthalmologists
Clinic Locations
PNI-SANTA MONICA (map)
2125 Arizona Ave
Santa Monica, CA 90404
310-829-8701
PNI-SOUTH BAY (map)
5215 Torrance Blvd #300
Torrance, CA 90503
424-212-5361
Accepted Insurance
Medicare, medicaid and most insurance plans are accepted. Please contact us to confirm coverage.
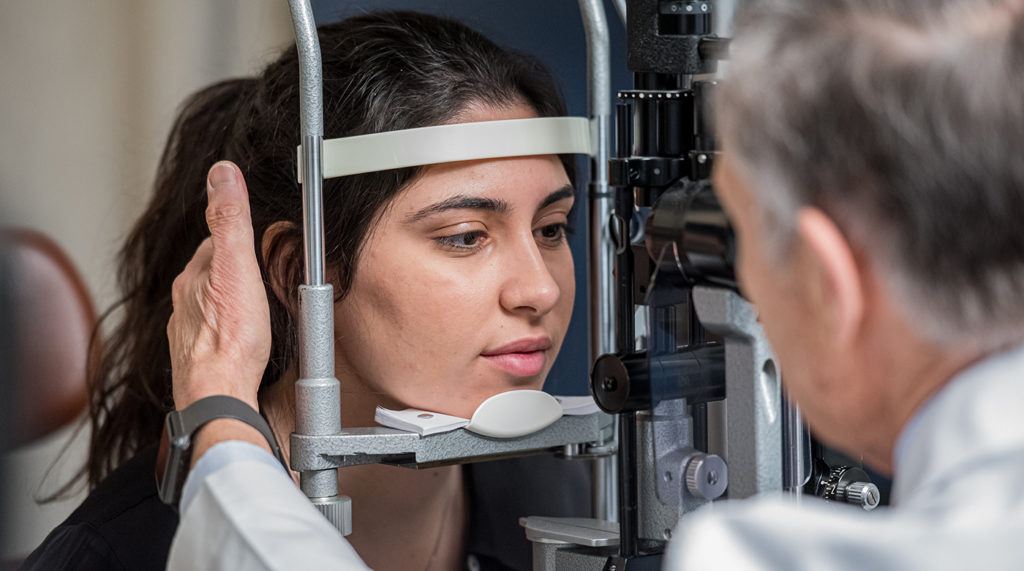
Contact us:
PNI-Santa Monica: 310-829-8701
PNI- South Bay: 424-212-5361





