Synkinesis
What is Synkinesis?
Overview
Facial synkinesis refers to abnormal regrowth of facial nerve fibers which may result in involuntary (unwanted) contraction of certain muscles during other intended facial movement.
Examples of synkinesis include:
- When you smile, the eye on the affected side may close
- When you smile, your neck muscles tighten
- When you blink, or close your eye, the corner of the mouth on the affected side pulls up
- When you chew your eye closes
Facial synkinesis may occur in anyone who has a history of facial nerve paralysis, but it is most often seen in patients with delayed recovery of facial nerve function (i.e. greater than 2-3 months).
It is less common in Bell’s palsy (10%) and more often seen in patients with Ramsay Hunt Syndrome (30%). Synkinesis may also occur if the facial nerve is harmed or injured following removal of a brain tumor, salivary gland tumor, or as a result of trauma to the head or face.
Synkinesis is not typically isolated to one part of the face and usually affects multiple regions such as the eye, mouth and neck. It affects each patient differently.
Some patients with synkinesis do not seek treatment while others require a multidisciplinary approach that includes a facial plastic surgeon, physical/occupational therapists and/or a speech-language pathologist.
Who is Affected?
Synkinesis can affect anyone who has experienced facial nerve paralysis, regardless of the initial cause. It is most commonly seen in individuals recovering from delayed or incomplete facial nerve recovery, particularly following Bell’s palsy, Ramsay Hunt Syndrome, head or facial trauma, or surgical procedures involving the facial nerve, such as removal of a brain or parotid gland tumor. While both men and women can develop synkinesis, it tends to appear months after initial facial weakness, often when nerve fibers regrow abnormally. The condition can affect people of all ages and may cause significant functional and emotional challenges, especially if it interferes with eye closure, speech, or facial expression.
Synkinesis Symptoms & Causes
Symptoms
Synkinesis occurs after complete facial paralysis has resolved and you start to experience recovery and reinnervation of the affected side of your face. It may take 2-3 months after the recovery is completed and patients will begin to notice the involuntary “linking of movements.” In addition to the unwanted linking of movements, patients may also complain of pain or tenderness in these locations as well, with or without movement. In most cases, synkinesis will not resolve completely and will require continued therapy for the remainder of the patients lifetime.
The types of synkinesis that are most often observed are:
- Oral-ocular: when moving the mouth (eg. To smile, lip pucker, chew) the eye on the affected side will partially/fully close. However, the unaffected eye will remain wide open
- Ocular-oral: when elevating the eyebrows or closing the eyes, the corner of the mouth will raise on the affected side
- Midfacial: at rest or with eye/mouth movement the cheek on the affected side will tighten leading to a deeper crease at the nasolabial fold and pain/discomfort in the cheek area
- Mentalis: when initiating eye or mouth movement, the chin will experience a dimpling on the affected side
- Platysma: when moving the mouth, the neck muscles on the affected side will tighten. This can prevent full smile elevation and pull the corner of the mouth downward
Causes
Synkinesis occurs as a result of abnormal regeneration of facial nerve fibers following an episode of facial nerve paralysis. When the facial nerve is damaged—due to viral infection, surgical trauma, tumor removal, or blunt injury—the healing process may lead to misrouting of nerve signals. As a result, fibers that were originally responsible for one function (such as smiling) may unintentionally connect to muscles involved in another function (such as blinking). This creates a “cross-wiring” effect, where voluntary facial movements trigger unintended muscle contractions. Although synkinesis can occur in anyone recovering from facial nerve injury, it is more common in those with delayed or incomplete recovery and may become more noticeable months after initial nerve healing begins.
When to See a Doctor
You should see a doctor if you have experienced facial paralysis and begin to notice involuntary movements, tightness, or facial asymmetry as you recover.
Warning signs that warrant medical attention include:
- Eye closure when smiling or eating
- Facial tightness, pulling, or pain in the cheek, chin, or neck
- Difficulty with eyelid closure or oral movements affecting speech or eating
- Increased facial asymmetry or noticeable facial distortion with expression
- Emotional distress or anxiety related to facial appearance or movement
Early intervention with our facial nerve specialist and multidisciplinary team—including facial plastic surgeons, physical therapists, and speech-language pathologists—can help improve function, reduce discomfort, and prevent worsening of symptoms. If symptoms are affecting your quality of life, seeking care promptly can lead to better long-term outcomes. Contact us at 310-829-8701.
Synkinesis Diagnosis
Synkinesis is a clinical diagnosis, meaning it is identified through a careful history and physical examination by a physician experienced in facial nerve disorders. Because the signs can be subtle or vary in intensity, it’s important to describe the timing, location, and nature of your symptoms in detail.
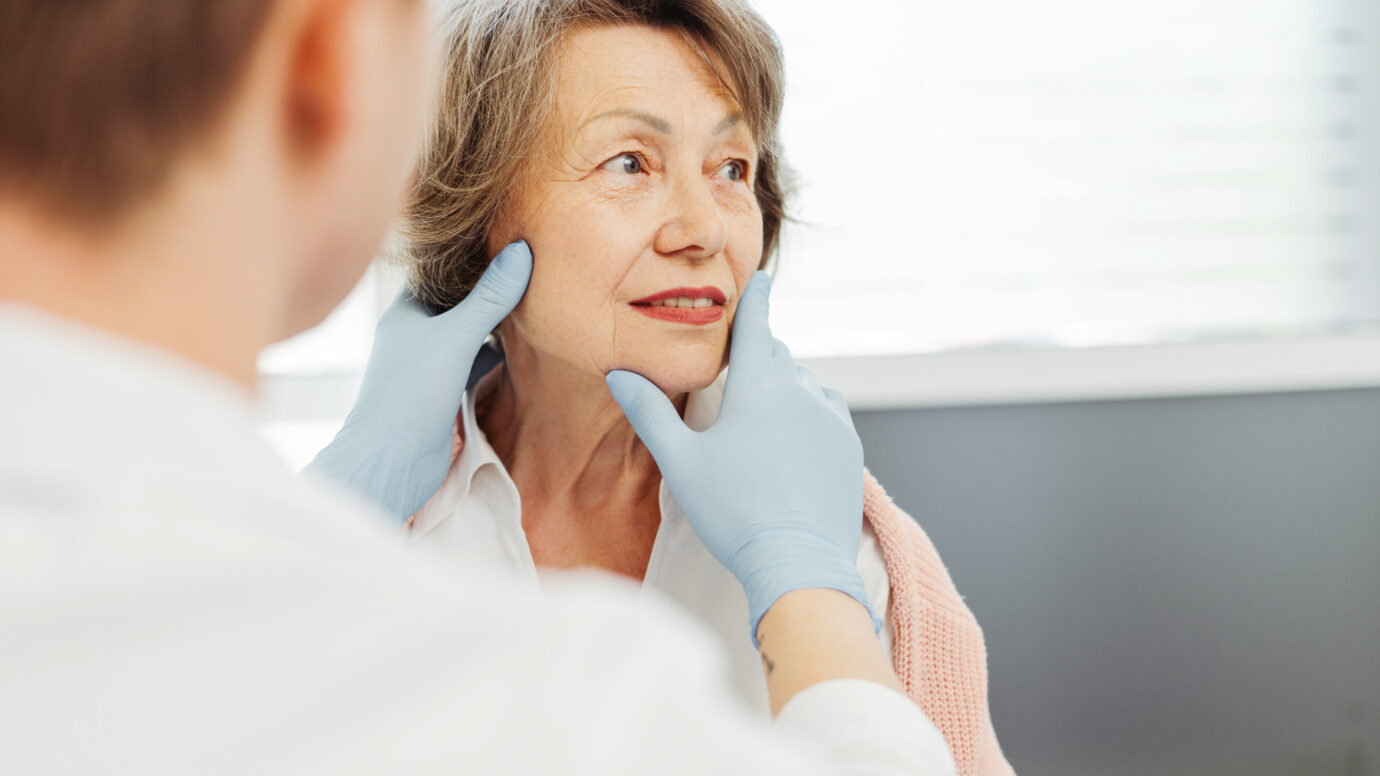
Physical Examination
Your physician will assess facial symmetry at rest and with movement, looking for patterns of involuntary muscle contractions during voluntary facial expressions, such as smiling, blinking, or puckering.

Symptom Documentation
To enhance accuracy, it is often helpful to document symptoms with digital photographs or video recordings, especially if your symptoms change throughout the day or worsen with fatigue.
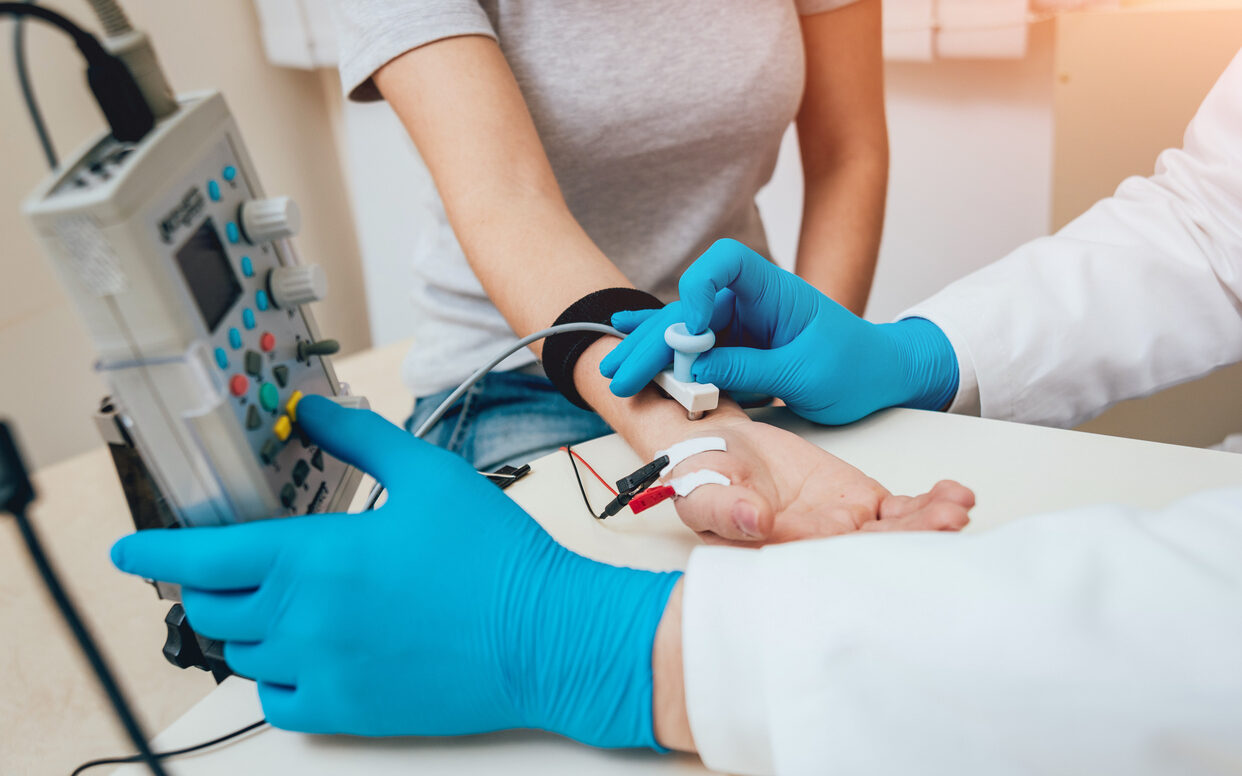
Electromyography (EMG)
In some cases, electromyography (EMG) may be used to study muscle activity and identify abnormal nerve signaling. This can help confirm the presence of synkinetic movements and guide treatment planning.
Since synkinesis typically develops months after facial nerve injury or paralysis, early evaluation by a facial nerve specialist is key to monitoring recovery and identifying signs of misdirected nerve regeneration as they arise.
Synkinesis Treatment & Outcomes
Treatment Options
The goal for treating synkinesis is to reduce the unwanted facial movement and to restore balance to the face. Since each patient has a unique type of synkinesis, the treatment of synkinesis will vary from patient to patient. Most, but not all, patients will benefit from a multidisciplinary approach that includes facial therapy by an expert in facial physical/occupational therapy, speech language pathology, and plastic surgery of the face.
There are several excellent methods used to treat facial synkinesis. Below we have listed these treatments from minimally invasive (facial therapy) to invasive surgery (selective neurolysis).
- Facial retraining therapy
- Mindfulness/Meditation
- Acupuncture
- Chemodenervation with botulinum toxin
- Selective neurolysis surgery
Patient Outcomes
Outcomes for patients with synkinesis can vary depending on the severity of symptoms, the cause of the original facial nerve injury, and the timing of intervention. While synkinesis typically does not resolve entirely on its own, early diagnosis and a comprehensive treatment plan can lead to meaningful improvements in both function and appearance. Many patients experience reduced tightness, improved facial symmetry, and greater control of facial movements with consistent therapy. In some cases, surgical procedures or targeted Botox® injections can further enhance results when conservative measures are not sufficient. Long-term outcomes are best when patients work closely with a multidisciplinary team to monitor progress and adjust care over time.
Managing Synkinesis
Managing synkinesis involves a personalized, long-term approach to reduce unwanted movements, improve facial function, and enhance quality of life. Key strategies may include:
Facial Neuromuscular Retraining Therapy
With a physical or occupational therapist to re-educate facial muscles and improve coordination
Botulinum Toxin (Botox®) Injections
To selectively weaken overactive muscles and reduce involuntary contractions
Massage and Stretching Techniques
To decrease muscle tightness and discomfort
Mindfulness and Relaxation Practices
As stress and fatigue may worsen symptoms
Surgical Intervention
(Such as selective neurolysis or muscle transfer) in advanced or treatment-resistant cases
Regular follow-up with our facial nerve specialist and facial plastic surgeon is important to assess progress and modify treatment as needed. While synkinesis may require ongoing management, many patients achieve significant relief and greater facial control through a combination of therapies.
Experience Compassionate, Expert Care

Through a multidisciplinary approach we care for each patient with a treatment plan tailored to their condition. At the Pacific Facial Disorders Center, our team works together to provide comprehensive diagnosis and definitive treatment options for a wide array of facial nerve disorders and facial pain syndromes. Our doctors and surgeons practice at award winning hospitals throughout Los Angeles.
Facial Nerve Disorders Program Director and otolaryngologist, Dr. Amit Kochhar, has over a decade of experience managing patients with facial paralysis. He treats and is accepting new patients from all over California, Arizona, Nevada, Oregon and Washington.
Learn More About Synkinesis
Synkinesis will not go away completely. However, with continued therapy that may include facial retraining, chemodenervation, and other treatments such as mindfulness, the severity of synkinesis can be reduced.
Most experts that treat patients with facial paralysis use a scoring system to grade severity of synkinesis. The most comprehensive scoring system is the Sunnybrook Facial Grading System which allows for an assessment of facial range of movement, and has a section dedicated to rating the presence of synkinesis.
Another helpful tool is the Synkinesis Assessment Questionnaire (SAQ). The SAQ can provide a reliable measurement of synkinesis and how it affects the patient.
Many clinicians may also use digital photography and video to score a patients facial paralysis and synkinesis. The EFACE scoring system is used to assess patients at rest, with dynamic facial movement and to also assess severity of synkinesis.
Together these tools provide the information your clinicians need to properly evaluate and treat synkinesis.
No. Bell’s palsy is a temporary paralysis or weakness of the facial muscles, usually caused by inflammation of the facial nerve. Synkinesis, on the other hand, often develops as a long-term complication after facial nerve injury or recovery from Bell’s palsy. It happens when nerve signals to the facial muscles become misdirected, causing involuntary movements — for example, the eye closing when you smile.
Synkinesis is not typically classified as a disability in a legal sense, but it can significantly affect daily activities, facial function, and emotional well-being. The severity can vary widely, and for some people, it may interfere with activities like speaking, eating, or expressing emotions. Treatments such as physical therapy, Botox® injections, and in some cases surgery can help improve function and appearance.
Yes, stress can make synkinesis symptoms more noticeable. Emotional stress and fatigue often increase muscle tension and involuntary facial movements, which can make the condition feel worse. Relaxation techniques, good sleep habits, and stress management strategies can help minimize symptom flare-ups alongside medical treatments.
Resources

Get Expert Care from Leading Specialists
At Pacific Neuroscience Institute® (PNI), our specialists in facial reanimation perform a comprehensive evaluation—including a detailed medical history, physical examination, and diagnostic testing—to develop a personalized treatment plan for each patient with synkinesis. Whether you’re seeking a second opinion, a new treatment strategy, or ongoing care, our team of top facial nerve surgeons and facial disorders experts is here to help you achieve the best possible outcome.



