Olfactory Neuroblastoma (Esthesioneuroblastoma)
What is Olfactory Neuroblastoma?
Overview
Olfactory neuroblastoma, also known as esthesioneuroblastoma, is a rare type of malignant tumor that originates from the specialized nerve cells located in the upper part of the nasal cavity.
These cells are responsible for the sense of smell, hence the name “olfactory” neuroblastoma. Olfactory neuroblastomas (ONBs) are locally invasive tumors that grow into the ethmoid and other air sinuses and can extend onto the orbits as well as the brain.
In cases with intracranial (brain) extension, the tumor typically grows through the anterior skull base dura in the area of the cribiform plate and into the brain cavity elevating or infiltrating the frontal lobes. Spread of disease to local lymph nodes and distant metastases occur in some patients.
The most commonly used grading system for esthesioneuroblastoma is the Kadish system which includes grades A, B and C:
- A. Nasal cavity only
- B. Nasal and paranasal sinus involvement
- C. Extension beyond nasal and paranasal sinus with intracranial, orbital, lymph node or distant metastases
The most common presenting symptoms include nasal congestion, epistaxis (nosebleeds), nasal obstruction, and a decreased sense of smell. Other possible symptoms may include facial pain, headache, vision changes, and swelling around the eyes.
Who is Affected?
Olfactory neuroblastoma primarily affects adults, with a peak incidence in the fifth and sixth decades of life. They occur equally in adult men and women and are uncommon in adolescents.
Olfactory Neuroblastoma Symptomsrn& Causes
Symptoms
Olfactory neuroblastomas typically cause loss of sense of smell (anosmia), epistaxis (nasal bleeding), nasal congestion/obstruction, vision loss and headache. If the tumor invades the dura and intracranial space, seizures and/or cognitive changes may occur.
Causes
The exact cause of olfactory neuroblastoma is not well understood. However, genetic mutations and chromosomal abnormalities are believed to play a role in its development. Exposure to certain environmental factors or occupational hazards may also be associated with an increased risk, although this relationship is not fully established.
When to See a Doctor
Early evaluation and diagnosis can significantly improve treatment options and outcomes. Seek immediate medical attention if you experience:
- Persistent or unexplained nasal bleeding
- Worsening nasal congestion or blockage unresponsive to typical treatment
- Changes in sense of smell or vision
- Persistent headaches or facial pain/swelling
- Neurological symptoms such as seizures or cognitive changes
Olfactory Neuroblastoma Diagnosis
Diagnosing olfactory neuroblastoma requires a combination of imaging studies and histological examination.
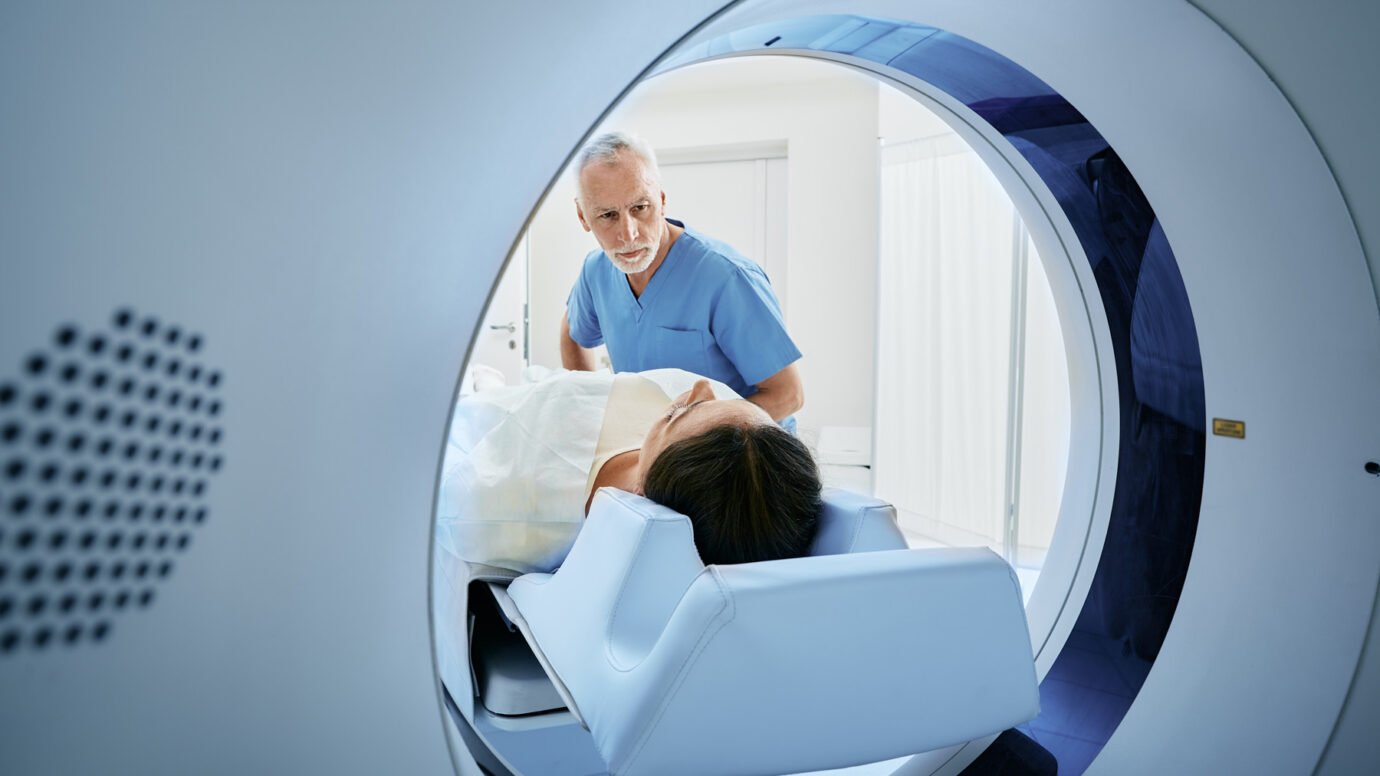
Imaging
Imaging techniques such as magnetic resonance imaging (MRI) and computed tomography (CT) scans are used to visualize the tumor, assess its size, extent, and involvement of adjacent structures.
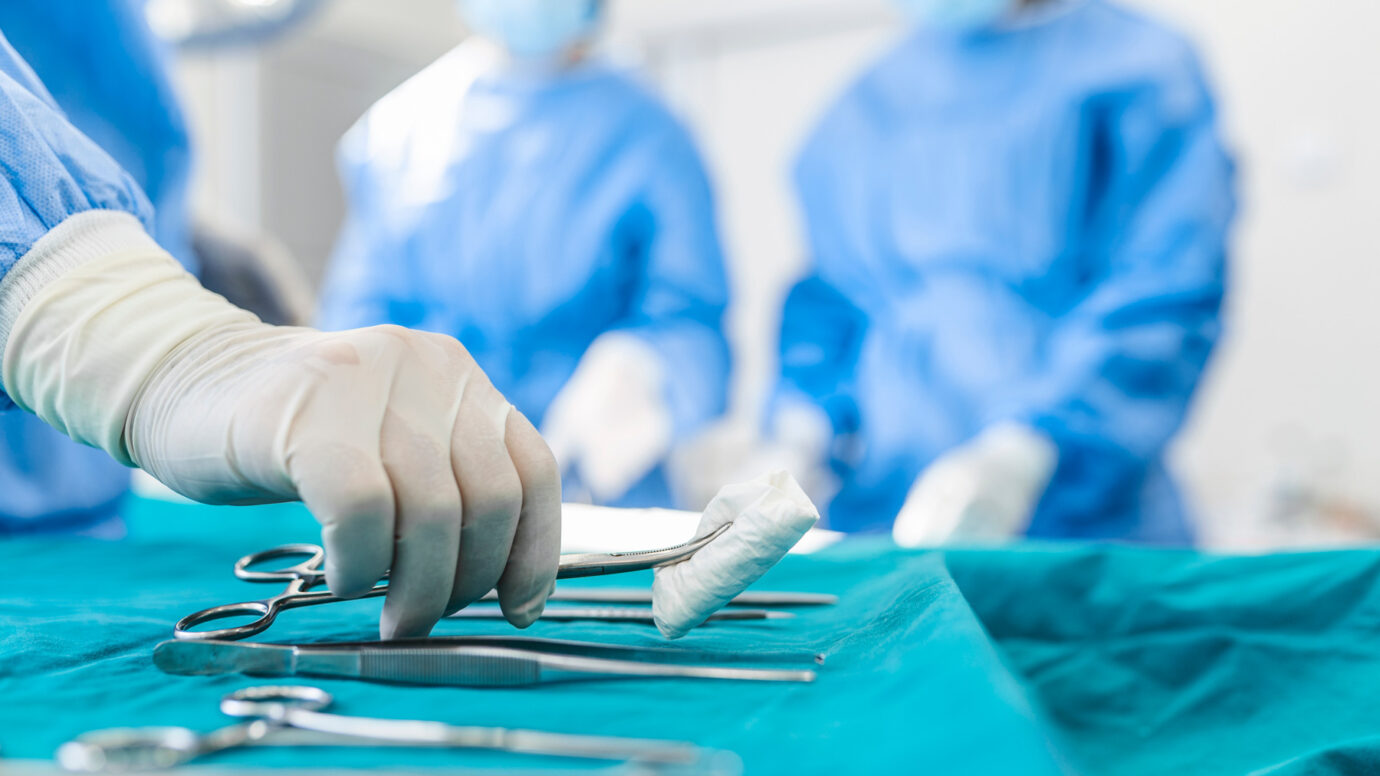
Biopsy
A biopsy is necessary to obtain a tissue sample for microscopic analysis to confirm the diagnosis and determine the tumor grade.
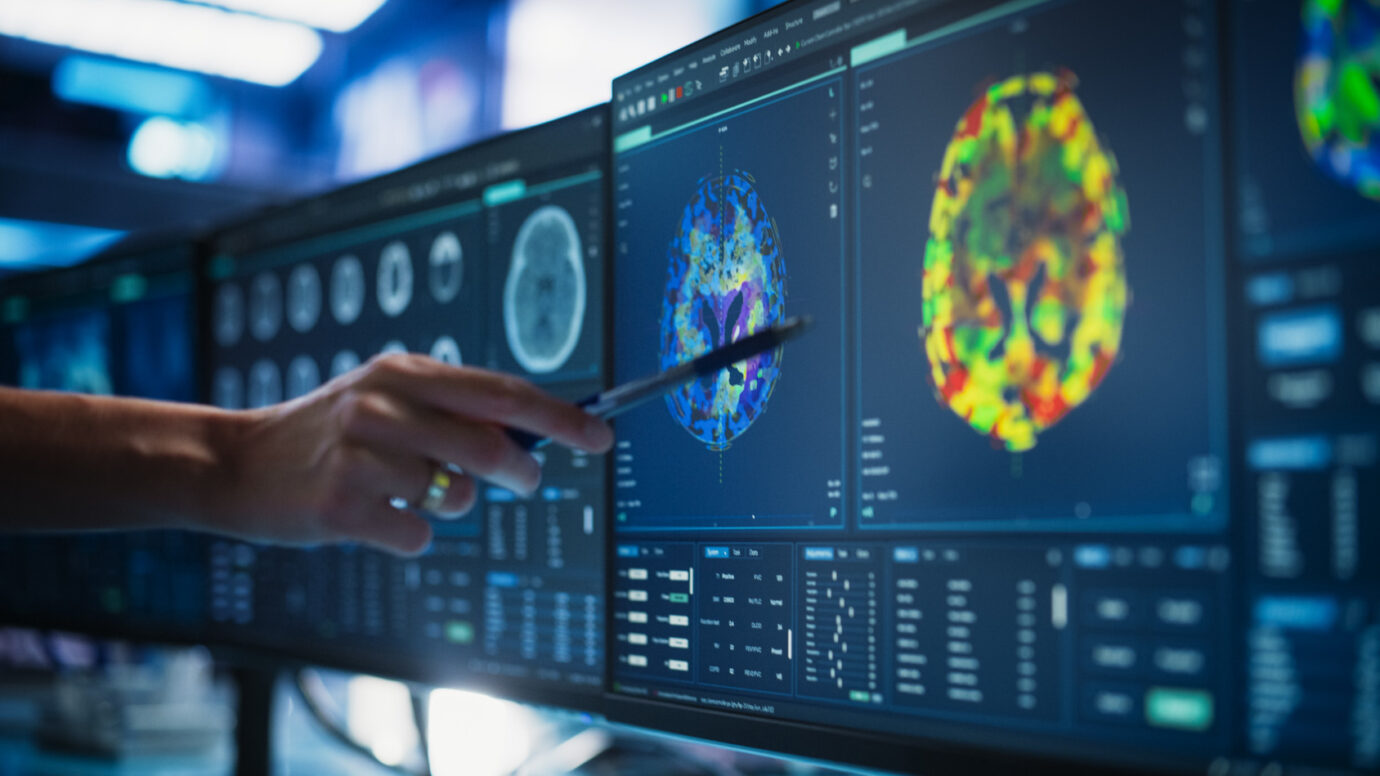
Pre-Operative Angiography and Embolization
For large, highly vascular tumors, pre-operative angiography and tumor embolization is often indicated.
Olfactory Neuroblastoma Treatmentrn& Outcomes
Treatment Options
The aggressive nature of ONB typically warrants multimodality treatment.
The optimal treatment for most patients with olfactory neuroblastomas (ONB) is maximal surgical removal. Fortunately, with advances in endoscopy, instrumentation and anatomical understanding, many if not most olfactory neuroblastomas can be removed via an endoscopic endonasal approach, including those with intradural extension. For some very large tumors with intracranial extension, a combined endonasal and transcranial approach may still be needed.
Typically recommended after surgery to target any residual disease and reduce recurrence risk.
Considered for advanced or metastatic cases or when tumors are not fully resectable.
Patient Outcomes
With prompt diagnosis and comprehensive treatment, many patients achieve good long-term control of their disease. Prognosis depends on tumor stage at diagnosis, completeness of surgical removal, and response to adjuvant therapy. Long-term follow-up is critical, as these tumors can recur years after treatment.
- Early-stage tumors (Kadish A or B) often have excellent outcomes with combined treatment.
- Advanced-stage tumors (Kadish C) may require more intensive therapy but can still achieve durable control with a multidisciplinary approach.
Managing Olfactory Neuroblastoma
Our team provides personalized care plans, ensuring patients receive comprehensive support throughout their treatment and recovery journey. Living with olfactory neuroblastoma often requires:
Regular Follow-Up Visits
With MRI or CT scans to monitor for recurrence.
Supportive Care
To manage treatment side effects (e.g., sinus issues, vision changes, fatigue).
Rehabilitation Services
Such as olfactory training or cognitive therapy, for those with lasting sensory or neurological effects.
Meet our Expert Specialists & Surgeons
Experience Compassionate, Expert Care

By using comprehensive tumor histological subtyping and genomic sequencing, we are able to provide a personalized therapeutic approach for each patient with ONB. We incorporate leading-edge technology and instrumentation with proven surgical experience, making surgery for ONBs and related skull base tumors safer, less invasive and more effective.
Our neurosurgeons work closely with our radiation oncologists, neuro-oncologists and neuropathologists to design the optimal treatment plan that incorporates the latest in radiotherapy techniques. Given advances in personalized and targeted genomic-based therapies, we routinely bank tissue for genetic analysis and detailed tumor biomarker studies. Having such critical biomarker data opens the door for novel therapies and ongoing or future clinical trials.
Learn More About Olfactory Neuroblastoma
Survival rates vary depending on stage and treatment, but with modern multimodality therapy, 5-year survival rates range between 60–90%, with better outcomes for early-stage disease.
Yes. They are two names for the same condition.
Prognosis depends on tumor stage, grade, and treatment response. Early-stage disease has an excellent prognosis with combined therapy.
It can be if untreated or diagnosed at an advanced stage. However, multimodality therapy significantly improves survival and quality of life.
The cause is not fully understood, but genetic mutations likely play a role. Environmental and occupational exposures may also contribute.
With comprehensive treatment, many patients live long, full lives. Lifelong follow-up is recommended, as recurrences can occur even years after treatment.
Resources

Get Expert Care from Leading Specialists
At Pacific Neuroscience Institute we have large experience in treating olfactory neuroblastomas and related sino-nasal tumors. Our team of neurosurgeons and specialists can provide a comprehensive evaluation and personalized treatment plan.






