Shunts
What are Shunts?
Shunts are medical devices used to treat hydrocephalus, a condition in which excess cerebrospinal fluid (CSF) builds up in the brain. A shunt system helps redirect this fluid from the brain’s ventricles to another area of the body—most often the abdominal cavity—where it can be safely absorbed.
This procedure is one of the most common and effective treatments for hydrocephalus. By relieving excess pressure on the brain, shunts help reduce symptoms such as headaches, balance problems, vision changes, and cognitive difficulties, while also protecting against long-term neurological damage.Because hydrocephalus can affect patients of all ages, from infants to older adults, shunts remain a vital treatment option to restore normal CSF flow and improve quality of life.
Types of Shunts
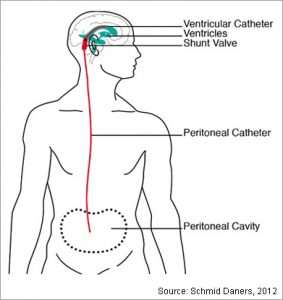
Patients who have communicating hydrocephalus or who have failed an ETV may benefit from the placement of a ventriculoperitoneal shunt (VP Shunt).
This device drains cerebrospinal fluid from the brain to the abdominal cavity with a thin silicone tube. A valve is used to control the amount of fluid drained.
This common procedure is performed with a “GPS” neuronavigation system to ensure accurate catheter placement. There are a variety of valves available, though we prefer one of a few programmable valves. These valves may have an MRI lock system to prevent unwanted shunt adjustments in a magnetic field. Some have “Off” switches to determine the necessity of the shunt without requiring to perform a surgical procedure to tie it off.
The abdominal portion of the catheter is placed laparoscopically with the assistance of a general surgeon, ensuring correct placement of the catheter and minimizing the risk of abdominal organ injury.
Though a common procedure, this device can have some complications during and after placement. These include catheter misplacement, catheter dislodgement, valve obstruction, shunt infection, abdominal organ injury, overdrainage, possible revision surgery or removal surgery and intracranial bleeding (acute or delayed).
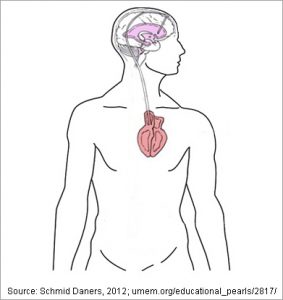
Patients who need a ventriculoperitoneal shunt but have scarring or infections in their abdomen may benefit from placing the drainage catheter directly into the bloodstream.
Additionally, patients who already have VP shunts but need further drainage to achieve symptom relief may need to drain directly into the lower pressure venous vessels. This is achieved with a ventriculoatrial shunt (VA Shunt).
This procedure is also well tolerated and carries similar risks to a VP shunt. Though the risk to the abdominal organs is eliminated, there is a slightly higher risk of bloodstream infections or heart valve infection (endocarditis). Also, there is a higher risk in patients with cardiac arrhythmias as the catheter can irritate the heart rhythm control region.
Placing a new VA shunt requires an inpatient stay. However, converting from a VP to VA shunt can be done on an outpatient basis for some patients.
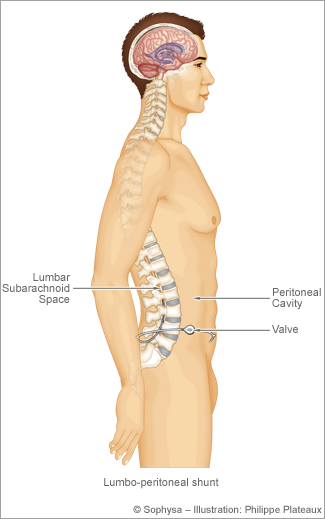
In some patients who have benefited with cerebrospinal fluid drainage via a lumbar drain to treat their condition (for example, CSF leakage or idiopathic intracranial hypertension–IIH), a lumboperitoneal shunt may be helpful.
This procedure connects a tube from the CSF fluid space in the lumbar spine to the abdomen, usually with a fixed valve to prevent overdrainage. We typically use a valve that adjust for patient position (sitting versus standing). The abdominal portion of the catheter is placed laparoscopically with the assistance of a general surgeon, ensuring correct placement of the catheter and minimizing the risk of abdominal organ injury.
This device can have some complications during and after placement. These include catheter misplacement, catheter dislodgement, valve obstruction, shunt infection, overdrainage, possible revision surgery or removal surgery and intracranial bleeding (acute or delayed). These shunts are less durable than VP shunts and can require more frequent revision operations.
Patients who have cysts in their brain or spinal cord may benefit from a direct cystoperitoneal shunt.
Similar to a ventriculoperitoneal shunt, this procedure diverts fluid from the cysts, helping decrease the pressure in the brain. Typically, these cysts are first treated with an endoscopic fenestration procedure. Cystoperitoneal shunts are reserved for patients who do not find benefit with the fenestration alone. Programmable valves are used to help taper fluid drainage.
The abdominal portion of the catheter is placed laparoscopically with the assistance of a general surgeon, ensuring correct placement of the catheter and minimizing the risk of abdominal organ injury.
Though a common procedure, this device can have some complications during and after placement. These include catheter misplacement, catheter dislodgement, valve obstruction, shunt infection, overdrainage, possible revision surgery or removal surgery and intracranial bleeding (acute or delayed).
How Shunt Surgery Works
Pre-Surgical Evaluation and Imaging
Before surgery, patients undergo a thorough evaluation to confirm the diagnosis of hydrocephalus and determine the best treatment approach. This typically includes neuroimaging studies such as MRI or CT scans to visualize cerebrospinal fluid (CSF) flow and measure ventricular size. Doctors also review the patient’s symptoms, overall health, and medical history to ensure shunt placement is the most effective option.
Surgical Procedure: Placement of Catheter and Valve System
Shunt surgery involves placing a thin, flexible catheter into the brain’s ventricles where excess CSF accumulates. This catheter connects to a valve system that regulates fluid flow and prevents over-drainage. Another catheter then routes the fluid to a different part of the body—most commonly the abdominal cavity—where the CSF can be safely absorbed. The procedure is performed under general anesthesia and usually takes a few hours.
Recovery and Post-Operative Care
After surgery, patients are closely monitored in the hospital for several days. Pain is typically mild and managed with medication. Post-operative imaging may be performed to confirm correct shunt placement. Most patients gradually return to their normal activities within a few weeks, although regular follow-up is necessary to ensure the shunt is functioning properly.
Benefits of Shunt Placement
Symptom Relief
By diverting excess CSF, shunts help relieve the pressure inside the brain, which often improves symptoms such as headaches, blurred or double vision, balance problems, and memory or concentration difficulties.
Long-Term Prevention of Brain Damage
Uncontrolled hydrocephalus can lead to progressive brain injury. A properly functioning shunt reduces the risk of long-term complications, preserving neurological function and protecting against further cognitive decline.
Improved Daily Functioning and Quality of Life
Many patients experience significant improvements in mobility, independence, and overall quality of life after shunt placement. For children, this may support developmental progress, while for adults, it often restores confidence in daily activities.
Risks and Potential Complications
Infection
As with any surgical procedure, there is a risk of infection. Shunt infections typically occur within the first few months after surgery and may require antibiotic treatment or shunt revision.
Shunt Blockage or Malfunction
Shunts can sometimes become clogged or stop working properly, leading to a return of hydrocephalus symptoms. This is one of the most common reasons for shunt revision surgery.
Over-Drainage or Under-Drainage of CSF
If the shunt removes too much fluid (over-drainage) or too little (under-drainage), patients may experience headaches, dizziness, or continued symptoms of hydrocephalus. Adjustable valves can help fine-tune CSF drainage as needed.
Need for Revision Surgery
Because shunts are mechanical devices, they may require replacement or adjustment during a patient’s lifetime. Regular monitoring helps detect potential problems early, ensuring timely intervention.
Recovery and Aftercare
Monitoring and Follow-Up Care
Patients with shunts require ongoing follow-up appointments with their neurosurgeon to monitor shunt function. Routine imaging and physical exams are often recommended to ensure proper CSF regulation.
Signs That May Require Medical Attention
Patients and caregivers should watch for warning signs such as severe headaches, nausea, vomiting, fever, drowsiness, or sudden changes in vision or balance. These may indicate a shunt malfunction or infection and require immediate medical evaluation.
Long-Term Outlook for Patients With Shunts
Many individuals with hydrocephalus live full and active lives with a properly functioning shunt. While some may need revision procedures over time, ongoing medical care and advances in shunt technology continue to improve long-term outcomes and quality of life.

Get Expert Care from Leading Specialists
Our multidisciplinary team at Pacific Neuroscience Institute specializes in shunt placement procedures. Our specialists will tailor care to each patient’s needs, ensuring optimal outcomes and safety.
Written and reviewed by:
The Pacific Neuroscience medical and editorial team
We are a highly specialized team of medical professionals with extensive neurological and cranial disorder knowledge, expertise and writing experience.
Last Updated: