Multiple System Atrophy
What is Multiple System Atrophy?
Overview
Multiple System Atrophy (MSA) is a rare and progressive neurodegenerative disorder that affects multiple systems within the nervous system. It is often considered an atypical parkinsonism syndrome.
The autonomic nervous system, which controls involuntary functions like blood pressure, heart rate, digestion, urination, and sweating, is often affected. Symptoms of autonomic dysfunction may include:
- Orthostatic hypotension (blood pressure dropping when standing)
- Urinary urgency, frequency, or incontinence
- Constipation
- Sexual dysfunction
- Impaired sweating
Types of Multiple System Atrophy
Autonomic MSA, previously known as Shy-Drager syndrome. This manifests with the symptoms listed above, in addition to postural instability, falls, stridor (difficulty with breathing in), head tilt (usually forward), dysphagia (trouble swallowing), dysphonia (abnormal quality of voice, often with a quivering component), and emotional variability.
Cerebellar MSA, previously known as Olivopontocerebellar atrophy (OPCA) or olivopontocerebellar degeneration (OPCD). This combines parkinsonism, autonomic dysfunction as above, and cerebellar findings such as imbalance, staggering gait, lack of coordination, and eye movement abnormalities. The cerebellar findings may precede the parkinsonism.
Parkinsonian MSA, previously known as striatonigral degeneration (SND), manifests with parkinsonism (moving slowly, tremor and stiffness) and autonomic dysfunction. Other symptoms associated with MSA include REM sleep behavior disorder (RBD), which is where there is an absence of the usual paralysis during dream sleep (rapid eye movement REM), resulting in acting out dreams; contractures; leaning to one side; depression and anxiety.
Who is Affected?
MSA typically begins between ages 50–60, though it can occur earlier or later. It affects both men and women, though some studies suggest it may be slightly more common in men. MSA is very rare, affecting about 3–5 people per 100,000.
Multiple System Atrophy Symptomsrn& Causes
Symptoms
MSA is characterized by:
- A combination of motor symptoms similar to Parkinson’s disease (such as bradykinesia, muscle rigidity, and tremors).
- Autonomic dysfunction (problems with blood pressure, heart rate, and other bodily functions).
- Cerebellar ataxia (affecting coordination and balance).
Causes
The exact cause of MSA is unknown. It is thought to involve abnormal accumulation of a protein called alpha-synuclein in brain cells, leading to nerve cell damage. Unlike some other neurological diseases, MSA does not appear to be inherited in most cases.
When to See a Doctor
See a neurologist if you experience:
- Repeated fainting or dizziness when standing.
- Unexplained urinary problems or severe constipation.
- Parkinson-like symptoms that progress rapidly or don’t respond to Parkinson’s medications.
- New problems with balance or coordination.
Early evaluation is important to rule out other conditions and begin supportive care.
Multiple System Atrophy Diagnosis
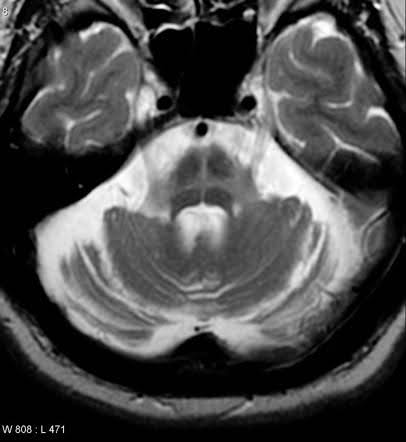
The diagnosis of MSA is often made based on typical findings on MRI, particularly cerebellar atrophy (shrinking in the size of the cerebellum), the “hot-cross bun” sign in the pons (part of the brainstem) or other areas of increased signal in the MRI such as a linear rim adjacent to the putamen. These can be quite subtle at times so our specialists will perform an independent review of all MRIs done on patients with PD or suspected MSA.
Multiple System Atrophy Treatmentrn& Outcomes
Treatment Options
The treatment of MSA is primarily based on alleviating symptoms as no cure exists at this time.
Patients should be monitored closely for severe issues such as breathing problems during sleep, supine hypertension (high blood pressure when lying down) and orthostatic hypotension (low blood pressure upon standing).
An FDA-approved medication for orthostatic hypotension, Northera (droxidopa) acts as a precursor to a brain chemical called norepinephrine. Older medications such as fludricortisone (Florinef) and midodrine all work to boost the blood pressure and reduce lightheadedness upon standing.
Patient Outcomes
MSA is a progressive disease. Most patients experience gradual worsening of symptoms despite treatment. Average survival is about 6–10 years after diagnosis, but this can vary. Early supportive care and symptom management can improve quality of life and safety.
Managing Multiple System Atrophy
Living with MSA requires a multidisciplinary approach that may include:
- Neurologists specializing in movement disorders
- Urologists for bladder symptoms
- Physical, occupational, and speech therapists
- Sleep specialists
- Mental health providers
Caregivers and family support are also crucial in daily management.
Meet our Expert Specialists & Surgeons
Experience Compassionate, Expert Care
At Pacific Neuroscience Institute, our specialists provide personalized, team-based care for patients with MSA. We offer advanced diagnostic tools, expert management of symptoms, and access to clinical trials aimed at slowing disease progression.
Learn More About Multiple System Atrophy
MSA is progressive and currently has no cure. Most patients live 6–10 years after diagnosis, though some live longer with supportive care.
MSA progresses faster, often involves severe autonomic dysfunction, and responds poorly to standard Parkinson’s medications.
Early signs often include dizziness on standing, urinary problems, or balance issues, sometimes before motor symptoms appear.
Rapid progression, early autonomic dysfunction, poor response to Parkinson’s medications, and balance issues are warning signs.
Parkinson’s disease, progressive supranuclear palsy (PSP), or cerebellar ataxias.
Common causes include breathing problems during sleep, infections (such as pneumonia), or complications from immobility.
Typically between 50–60 years old.
Resources

Get Expert Care from Leading Specialists
If you or a loved one has symptoms of MSA, our experts at Pacific Neuroscience Institute are here to help. We provide comprehensive evaluations, advanced treatment options, and compassionate support tailored to your unique needs.
Written and reviewed by:
The Pacific Neuroscience medical and editorial team
We are a highly specialized team of medical professionals with extensive neurological and cranial disorder knowledge, expertise and writing experience.
Last Updated:

