Idiopathic Intracranial Hypertension
What is Idiopathic IntracranialrnHypertension (IIH)?
Overview
Idiopathic intracranial hypertension (IIH) sometimes also called pseudotumor cerebri (PTC), the more general term, is a neurological condition in which the pressure around the brain is elevated without the presence of a tumor or other cause on imaging.
The more general term of pseudotumor cerebri, means “false brain tumor,” as the symptoms can mimic those of elevated intracranial pressure caused by a brain tumor and require careful diagnosis and management.
Naming convention note: “Idiopathic” means that the cause of a condition is unknown. So, in Idiopathic Intracranial Hypertension (IIH), “idiopathic” in the name suggests that the increased pressure inside the skull is happening without a clearly identifiable reason. However, in some cases the underlying cause is actually known—such as when the condition is medication-induced. For that reason, the older, broader term pseudotumor cerebri (PTC) remains more inclusive. Technically, IIH is a subtype of PTC, though the two terms are often used interchangeably in clinical settings. PTC is the older term, but it is still used—often to avoid alarming patients with the word “tumor” in a diagnosis that doesn’t actually involve one.
Idiopathic Intracranial Hypertension Symptoms & Causes
Symptoms
Symptoms can be debilitating and may include:
- Persistent, severe headaches that typically worsen when lying flat
- Visual disturbances (episodic blurred vision, double vision, tunnel vision, or transient or permanent vision loss)
- Pulsatile tinnitus # https://www.pacificneuroscienceinstitute.org/blog/ear-hearing/the-unwanted-beat-of-pulsatile-tinnitus/ # (hearing a rhythmic sound in the ears)
- Nausea and vomiting
- Neck or shoulder pain
One of the most concerning complications is vision loss, which can become permanent if not treated.
Causes
The exact cause of IIH/PTC is unknown, but several factors are associated with increased risk:
- Obesity, especially in women of childbearing age
- Certain medications (such as tetracyclines or excessive vitamin A)
- Hormonal changes
- Blood clotting disorders that affect brain venous drainage
- Narrowing of the venous outflow tracks that can affect brain venous drainage
When to See a Doctor
If you are experiencing persistent headaches, vision changes, or pulsatile tinnitus, it’s essential to seek medical evaluation. Prompt diagnosis and management of IIH/PTC can help prevent permanent vision loss. At Pacific Neuroscience Institute, our team of experts specializes in diagnosing and treating IIH/PTC with individualized care plans. Contact us to schedule a consultation at 310-582-7450.
Idiopathic Intracranial Hypertension Diagnosis
Diagnosis of idiopathic intracranial hypertension involves:
- Ophthalmologic examination to check for swelling of the optic nerves (called papilledema if due to elevated pressure)
- MRI or CT scan to rule out other causes
- Lumbar puncture to measure cerebrospinal fluid (CSF) pressure and confirm elevated intracranial pressure
- Visual field testing to monitor the extent of vision involvement
- Optical coherence tomography to help assess and track the amount of swelling and damage to the optic nerves and retinae
- Angiogram/venogram tests used to look for abnormalities in blood vessels
Idiopathic Intracranial Hypertension Treatment & Outcomes
Treatment Options
The goal of treatment is to reduce intracranial pressure, relieve symptoms, and protect vision.
Even modest weight reduction can significantly improve symptoms.
- Acetazolamide (to reduce CSF production)
- Topiramate (may also aid in weight loss and reduce pressure)
- Steroids (typically only used in severe cases where vision is threatened)
Occasionally used for temporary relief.
For more severe or refractory cases:
- Optic nerve sheath fenestration (to protect vision)
- Ventriculoperitoneal shunting (to divert CSF and lower pressure)
- Venous sinus stenting (in selected cases with venous outflow obstruction)
Patient Outcomes
With early diagnosis and appropriate treatment, many patients with idiopathic intracranial hypertension / pseudotumor cerebri experience significant improvement in symptoms and preservation of vision. Weight loss, medication, and in some cases, surgery can effectively reduce intracranial pressure. Long-term outcomes depend on timely intervention to prevent permanent vision loss. Regular monitoring by a multidisciplinary team — including neurology, neuro-ophthalmology, and neurosurgery specialists — is key to achieving the best results.
Managing Idiopathic Intracranial Hypertension
Managing IIH/PTC involves a combination of medical care and lifestyle changes:
Maintain a Healthy Weight
Even modest weight loss can significantly improve symptoms.
Take Medications as Prescribed
Medications such as acetazolamide can reduce cerebrospinal fluid production and lower pressure.
Monitor Vision Changes
Regular eye exams are critical to protect against vision loss.
Follow a Low-Salt, Balanced Diet
Helps reduce fluid retention.
Avoid Known Triggers
Such as high-sodium foods, certain medications (e.g., high-dose steroids), and rapid weight gain.
Stay Physically Active
Low-impact exercise can improve overall health and support weight management.
Attend Follow-Up Appointments
Routine neurological and ophthalmological evaluations ensure early detection of disease progression.
Experience Compassionate, Expert Care
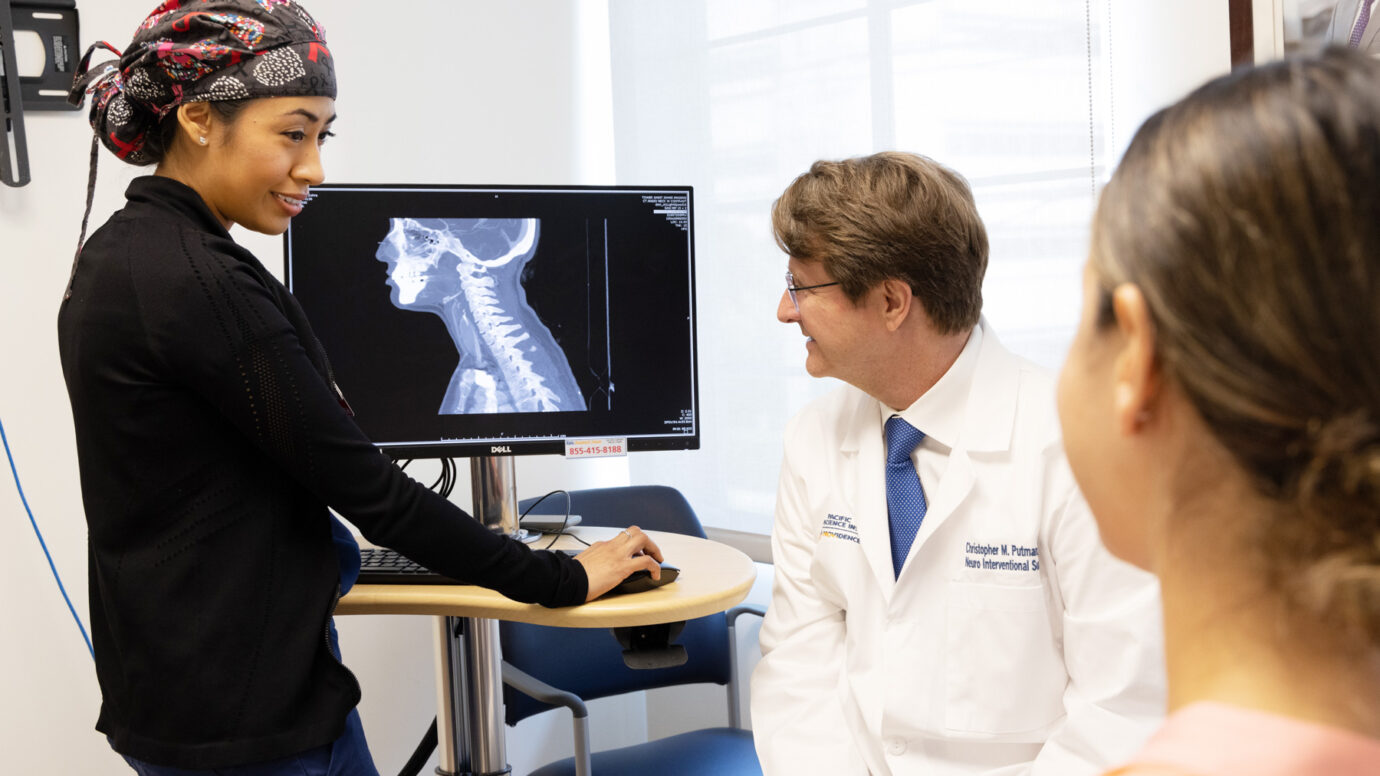
At Pacific Neuroscience Institute, we provide personalized, leading-edge care for patients with IIH/PTC. Our team uses advanced imaging, minimally invasive surgical techniques, and collaborative medical management to deliver the best outcomes. Our program offers:
- Specialized expertise in IIH, vision preservation, and CSF pressure management.
- Minimally invasive procedures such as optic nerve sheath fenestration and CSF shunting when needed.
- Comprehensive evaluations from a team of experts in neurology, neurosurgery, and neuro-ophthalmology.
- State-of-the-art facilities designed for patient comfort and safety.
Learn More About Idiopathic Intracranial Hypertension
IIH is often associated with weight gain, certain hormonal changes, and sometimes medication use (e.g., tetracycline, excessive vitamin A).
Yes. With proper management and regular monitoring, many patients lead full and active lives.
IIH does not typically reduce life expectancy, but untreated disease can cause permanent vision loss.
Rapid weight gain, high-salt diets, certain medications, or hormonal changes may worsen symptoms.
Avoid high-sodium foods, processed snacks, and excessive caffeine, which may increase fluid retention or pressure.
Resources

Get Expert Care from Leading Specialists
If you’ve been diagnosed with IIH or are experiencing concerning symptoms, our team at Pacific Neuroscience Institute is here to help with expert diagnosis and personalized treatment plans.
Written and reviewed by:
The Pacific Neuroscience medical and editorial team
We are a highly specialized team of medical professionals with extensive neurological and cranial disorder knowledge, expertise and writing experience.
Last Updated:
