Brain Aneurysm
What is a brain aneurysm?
A brain aneurysm is also called a cerebral aneurysm or an intracranial aneurysm and refers to the same diagnosis. The cerebrum – which is Latin for “brain” – is the coordinating center of sensation, intellectual and nervous activity. The brain is located within the cranium, which is Latin for “skull.”
Muscular-walled tubes blood vessels called arteries are part of our circulation system. These tubes are how blood is conveyed from the heart to the brain, carrying oxygen and nutrients to support the brain and its functions.
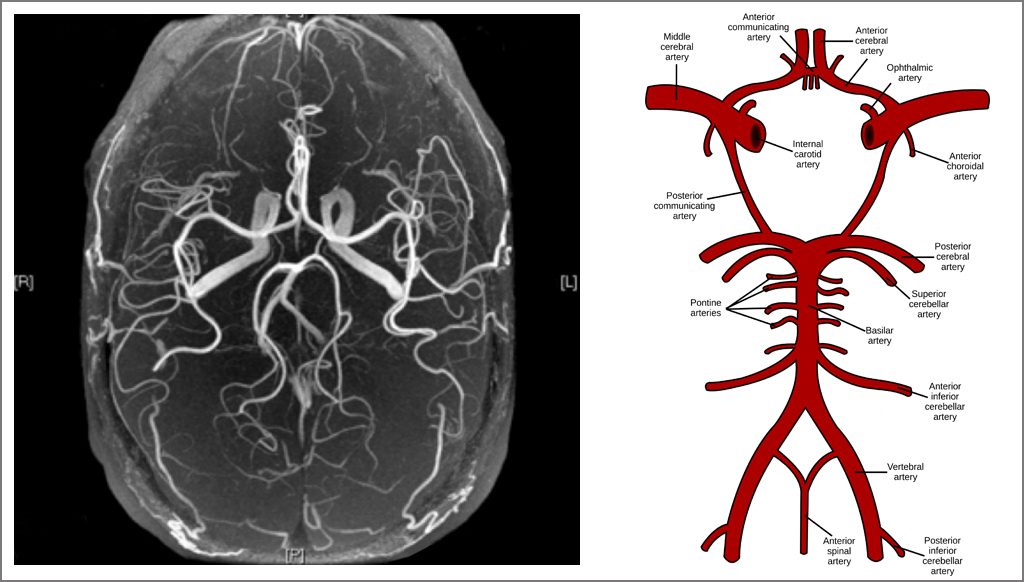
A diagnosis of a brain aneurysm means that a bulging, weak area exists in the wall of one of the arteries that supplies blood to the brain. The most common location for brain aneurysms is in the network of arteries at the base of the brain called the Circle of Willis.
How should I seek treatment for an aneurysm?
The first and most important step in seeking treatment for a brain aneurysm is to get an expert consultation from an advanced treatment center with expertise in all types of aneurysm treatments, including endovascular therapies and minimally-invasive microsurgical clipping.
Our experts in stroke neurology, interventional neuroradiology, and vascular neurosurgery work together using a team-based approach to personalize treatment decisions for each specific aneurysm based on the location, size and shape of the aneurysm as well as the patient’s age, overall health, and additional risk factors.

Causes of Aneurysm
When a brain aneurysm is diagnosed, the exact reasons that led to the development of the brain aneurysm are not currently known. Some risk factors that can lead to brain aneurysms can be controlled, and others can’t.
- Sometimes a person can inherit a tendency to form aneurysms due to weaknesses in the structure of arterial walls and/or heightened inflammatory responses.
- Aneurysms may also develop because of hardening of the arteries (atherosclerosis) and aging.
- People who have a family history of brain aneurysms are more likely to have an aneurysm than those who don’t.
- The risk of an aneurysm rupture is greater in people who have a history of high blood pressure as well as people who smoke.
- Other factors associated with heart disease and vascular disease also likely increase the risk of brain aneurysm formation and rupture, including poor diet and exercise, high cholesterol and diabetes.
Symptoms of Brain Aneurysm
In many cases, a brain aneurysm causes no symptoms and can go unnoticed.
Sometimes an unruptured aneurysm will cause problems by pressing on areas in the brain. When this happens, it can cause severe headaches, blurry vision or changes in speech.
In other cases, the brain aneurysm ruptures, releasing blood into the brain and causing a stroke. When a brain aneurysm ruptures, it is called a subarachnoid hemorrhage. Depending on the severity of the hemorrhage, brain damage or death may result.
Symptoms of a ruptured brain aneurysm often come on suddenly and include a sudden, severe headache (“worst headache of my life”) that is different from past headaches, nausea and vomiting, sensitivity to light, weakness, confusion, fainting or loss of consciousness, and seizures.
Diagnosis of Brain Aneurysm
Because unruptured brain aneurysms often do not cause any symptoms, many are discovered in people who are being evaluated for a different reason. If your doctor believes that you are at risk for having a brain aneurysm, you may undergo one of the following tests:
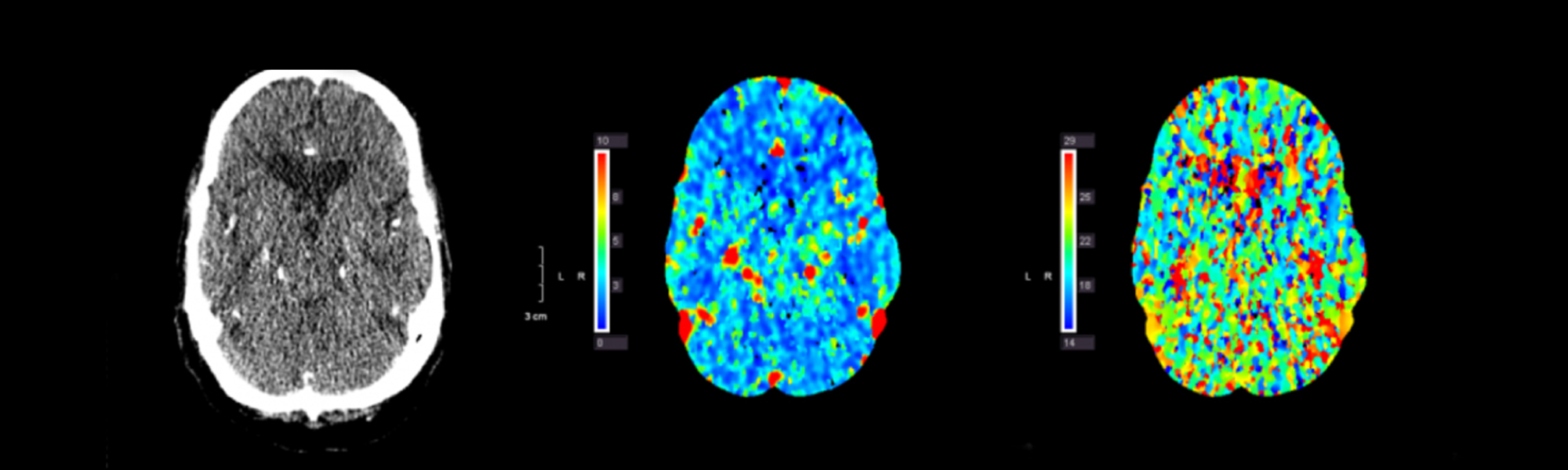
- Computed tomography (CT) scan.
A CT scan is a very quick test that can identify bleeding in the brain. Sometimes a lumbar puncture (“spinal tap”), which uses a needle to extract spinal fluid from your lower back, may be necessary if the CT scan does not clearly show bleeding but your doctor still suspects that you have a ruptured cerebral aneurysm with a subarachnoid hemorrhage.
- Computed tomography angiogram (CTA) scan.
CTA is a more precise method of evaluating blood vessels than a standard CT scan. CTA uses a combination of CT scanning, special computer techniques, and contrast material (dye) injected into the blood to produce images of blood vessels.
- Magnetic resonance angiography (MRA).
Similar to a CTA, MRA uses a magnetic field and pulses of radio wave energy to provide pictures of blood vessels inside the body. As with CTA, a dye is used during MRA to make blood vessels show up more clearly.
- Cerebral angiogram.
Cerebral angiogramThis is the “gold standard” test for the clearest images of the blood vessels. This procedure takes place in a catheterization lab, while you are under sedation, a tiny catheter is inserted through a blood vessel in the groin and moved up from the inside of the blood vessel into the brain. A dye is then injected into the cerebral artery. As with the above tests, the dye allows any problems in the artery, including aneurysms, to be seen clearly using specialized X-rays. Although this test is more invasive and carries more risk than the above tests, it is the best way to locate small brain aneurysms and to clearly visualize the shape of the aneurysm to guide treatment decision-making.
Treatment of Aneurysm
Aneurysms that have bled are very serious and considered a medical emergency that requires immediate treatment. In many cases, aneurysm rupture leads to death or severe disability. For those fortunate to survive the initial bleeding event, management includes emergent hospitalization to the intensive care unit (ICU) to maintain breathing and vital functions (such as blood pressure) and treatment to reduce brain swelling and to secure the aneurysm to prevent further bleeding.
For patients with an unruptured aneurysm, the risk of a future rupture occurring can be estimated using published data derived from studying a large numbers of patients. If the risk of rupture is greater than the risk of intervention, treatment is recommended in order to prevent rupture and the possible outcomes of death or severe disability.
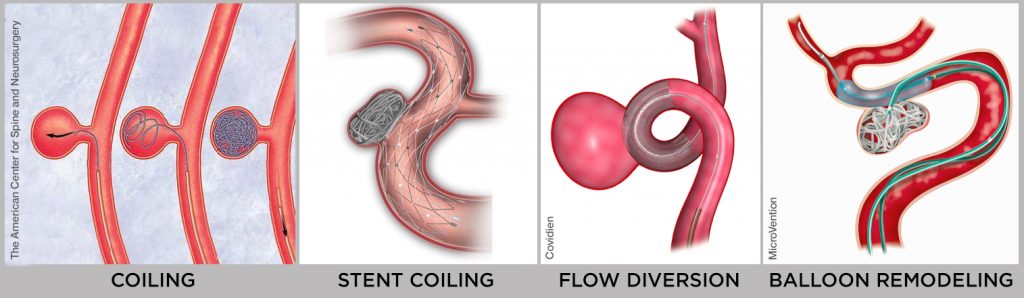
- Endovascular aneurysm treatment
During these procedures, a small tube is inserted into the affected artery and positioned near the aneurysm. In aneurysm coiling, specialized metal coils are then moved through the tube into the aneurysm, filling the aneurysm to prevent blood flow into the aneurysm to protect against the risk of rupture. Sometimes the use of a special metal cage called a “stent” can be used to assist the coiling. Other times aneurysms can be treated with a specially-designed stent that diverts flow away from the aneurysm (called a flow-diverting stent). While endovascular aneurysm treatment is less invasive than microsurgery, whether this is the optimal method to treat an aneurysm depends on the location of the aneurysm, its size and shape, and the patient’s general health.
- Minimally-invasive microsurgical aneurysm clipping.
This surgery involves the use of an operating microscope to perform a microsurgery that involves placing a specialized metal clip around the aneurysm to completely isolate it from blood flow in order to protect against the risk of rupture. While microsurgical clipping is thought to be a more durable treatment with less risk of recurrence than endovascular coiling, whether this is the optimal treatment option also depends on the location of the aneurysm, its size and shape, and the patient’s general health.

 Lyn’s Story – Aneurysm
Immediate treatment of a brain aneurysm saved Lyn’s life.
Lyn’s Story – Aneurysm
Immediate treatment of a brain aneurysm saved Lyn’s life.
 Meet Dr. Jason Tarpley
Meet Dr. Jason Tarpley
 Meet Dr. Hou
Meet Dr. Hou
 Meet Dr. Christopher Putman
Meet Dr. Christopher M. Putman, a board-certified interventional neuroradiologist with over 20 years of experience. He treats a variety of complex intracranial, head and neck, and spine vascular conditions including…
Meet Dr. Christopher Putman
Meet Dr. Christopher M. Putman, a board-certified interventional neuroradiologist with over 20 years of experience. He treats a variety of complex intracranial, head and neck, and spine vascular conditions including…
 Meet Dr. Walavan Sivakumar
Dr. Walavan Sivakumar is a fellowship-trained neurosurgeon with a focus on skull base and minimally invasive and endoscopic neursosurgery. Selected as a multiple year recipient of the SuperDoctor Rising Stars…
Meet Dr. Walavan Sivakumar
Dr. Walavan Sivakumar is a fellowship-trained neurosurgeon with a focus on skull base and minimally invasive and endoscopic neursosurgery. Selected as a multiple year recipient of the SuperDoctor Rising Stars…
 Meet Dr. Adi Iyer
Meet Dr. Adi Iyer
 Ron’s Story – Brain Aneurysm
Experience an actual account of a Brain Aneurysm.
Ron’s Story – Brain Aneurysm
Experience an actual account of a Brain Aneurysm.

Lyn’s Story

Meet Dr. Jason Tarpley

Meet Dr. Samuel Hou

Meet Dr. Christopher Putman

Meet Dr. Walavan Sivakumar

Meet Dr. Adi Iyer

Ron’s Story
Contact Us
The Pacific Stroke and Neurovascular Center’s state-of-the-art facilities are located at:
Providence Saint John’s Health Center
2125 Arizona Ave., Santa Monica, CA 90404
310-829-8319
Providence Little Company of Mary Medical Center Torrance
4201 Torrance Blvd., Suite 520, Torrance, CA 90503
424-212-5340
Providence Saint Joseph Medical Center
501 S. Buena Vista Ave., Burbank, CA 90505
818-847-6049
Providence Holy Cross Medical Center
15031 Rinaldi St, Mission Hills, CA 91345
818-847-6570