Deep Brain Stimulation
What is Deep Brain Stimulation?
The goal of deep brain stimulation (DBS) surgery is to modulate the activity of a specific brain region. In Parkinson’s disease, essential tremor, and dystonia, normal function can be restored to the circuitry of the brain, resulting in significant improvement in function and quality of life.
In DBS, thin electrodes are placed in the disruptive areas of the brain and small electrical pulses normalize or eliminate the irregular signals. DBS is the non-permanent suppression of overactivity in the autopilot structure of the brain called the basal ganglia.

Like a pacemaker for the brain, the battery (pulse generator) is implanted under the skin of the chest, and leads (wires) are tunneled under the skin via the deep part of the brain through a quarter-sized opening in the skull. The system is fully implanted under the skin, so there are no external wires or devices. The stimulator is fully programmable and therefore adjustable over time, as the disease changes. Patients can use a simple hand-held device to turn the DBS on or off, and adjust various other parameters if needed.
The 3 Steps of Deep Brain Stimulation
During this procedure, patients are mildly sedated and given local anesthetic to numb the skin. Because the brain tissue itself has no pain receptors, the leads can be placed with patients awake. This allows our team to determine the benefits of the stimulation. Patients typically stay one night in the hospital and are discharged the following day.
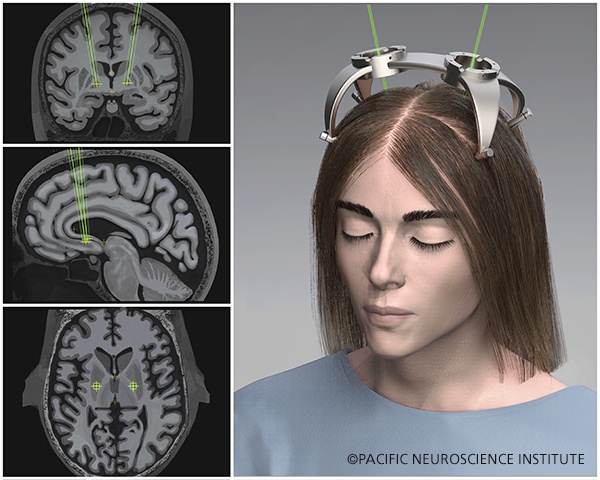
This procedure can be done with a frame (frame-based) or without a frame (frameless). Although we can perform a frame-based approach, the use of the frameless option provides a significantly more comfortable experience for the patient. Instead of having to wear a rigid frame that gets screwed into the operating table, immobilizing the head and neck, the frameless system is attached to the skull via previously placed fiducial markers, allowing the head and neck to remain mobile. The system employs a custom-made mini frame fitted to the patient’s head which reduces the time required for the surgery therefore optimizing recovery, without compromising precision.
This is done under general anesthesia, and typically 1-2 weeks after lead implantation. The pulse generator needs to be replaced about every 3-4 years. A rechargeable option exists that lasts 9 years but requires regular charging. At the post-operative visit, the battery is turned on and DBS programming begins. While it may take a few weeks for maximal benefit, patients soon experience relaxation of symptoms. The DBS program is customized for each patient based on maximizing symptom reduction.
About 3 weeks after the battery implantation, patients come to the office for activation of the DBS system. The settings are adjusted gradually and several configurations are tested to find the optimal settings at the first visit. It may require weeks of adjustments to medications and DBS settings to achieve the maximum benefit of both.
Considerations for Candidates of Deep Brain Stimulation
How Can DBS Help Me?
In patients with PD who have motor complications, dyskinesias, or tremor not improved with medication, DBS improves ON time, reduces dyskinesias and reduces tremor.
In patients with ET who have tremor interfering with activities of daily living such as pouring liquids, drinking from a cup, or writing, DBS dramatically reduces tremor and improves quality of life.
DBS reduces dystonia, improves quality of life and improves ability to perform activities of daily living in patients with medication-refractory dystonia, including both generalized dystonia and cervical dystonia.
Benefits of DBS
For patients with Parkinson’s disease, one of the main advantages of this kind of therapy is that medication fluctuates over time while DBS remains constant throughout the day. DBS is always on and complements an optimized medication regimen. Because DBS remains active between medication doses, it helps patients sustain longer periods of symptom-free activity even after the medication’s effect has worn off. On average, patients gain four to five hours of productive time in a typical day with DBS. It improves the main symptoms of Parkinson’s disease including tremor, rigidity and slowness and has been shown to improve quality of life. DBS is a mainstream treatment methodology that is FDA-approved and covered by health insurance plans.
DBS can have a transformative effect on quality of life for patients with essential tremor because of the high rate of symptom control. The vast majority of patients experience a significant improvement in tremor allowing them to perform their work or their hobbies. Our patients tell us they are finally able to enjoy meals with family and friends again as tremor symptoms remains under control.
The use of DBS for patients with dystonia improves objective scores of dystonia movement and disability, but more importantly, it greatly improves quality of life including physical function, pain, general health and depression scores.
Potential Risks of DBS
- DBS surgery is highly successful and as with any surgical procedure, there are some considerations. Post-operative headache and pain is possible which typically resolves gradually within a few weeks of the procedure. Neck pain may manifest in the short term. Infection of the leads, extension or battery is very low risk. Hemorrhage is extremely low risk but when it occurs may lead to stroke-like symptoms which alleviate and do not result in permanent complications. Lead fracture or migration, also very low risk, may require repeat surgery.
- Problems with speech, language and mood, muscle tightness, slurred speech and vision symptoms can be related to the stimulation and thus can usually be reduced or eliminated by adjusting the stimulation.
Preparing for Deep Brain Stimulation Surgery
In preparation for the surgery, we recommend that you focus on eating well and exercising regularly. If you have diabetes, it is important to keep your blood glucose under control in the weeks surrounding the surgery. Similarly, if you have high blood pressure, it is important to take your medications regularly and monitor your blood pressure frequently. These steps will help reduce the risks of complications at and around the time of surgery.
If you have a specific medical problem, we may recommend that you obtain clearance or recommendations from your physician before the surgery.
If you use a blood thinner (aspirin, Plavix, Coumadin, Pradaxa, Xarelto, Eliquis, etc.) the medication will need to be stopped prior to the surgery. Your physician and Dr. Langevin will determine the specific timing for stopping the medication as it will vary based on the specific blood thinner received and the condition which is treated by the blood thinner. If you consume alcohol regularly, it is also recommended to stop a few weeks before the surgery to reduce the risk of bleeding and facilitate the post-operative recovery.
On the day of the surgery, we recommend that you hold your Parkinson’s disease or tremor medication. The presence of symptoms can help us test the position of the electrode intra-operatively. However, blood pressure medications should generally be taken with a sip of water.
Recovering from Surgery
The hospitalization after DBS placement is typically brief and most patients can return home the day after surgery. Once at home, it is important to continue taking your medications for Parkinson’s disease and tremor. The DBS is not ON after the surgery and the generator (battery) is implanted one week after the electrodes are inserted.
The battery insertion is done under general anesthesia and does not require a hospital stay. We also recommend to continue following a healthy diet and gentle exercise, especially frequent walks. More strenuous activity or lifting more than 10 lbs is not recommend during the first month after surgery since the incisions are still healing and your energy level is likely not back to its baseline. After the first month, most activities can be resumed gradually.
Deep Brain Stimulation Surgery Specialist
Deep Brain Stimulation Surgery Resources
The incisions are small, about 2 inches on the top of the head, 1 inch behind the ear, and 2.5 inches below the collarbone. Typically only a small area near the incision on the top of the head requires shaving.
3-4 years depending on the settings required. A rechargeable option is also available which will last 9 years, but requires the patient to regularly charge the battery.
Once the electrodes are placed, a neurological exam is done to ensure that therapeutic benefit has been achieved. During this examination, the patient is awake. During the procedure, the anesthesia is tailored to the patient’s needs to make sure that pain and anxiety are properly relieved.
Patients typically go home after 1 or 2 days. Most patients feel they are back to their baseline level of energy after 2 weeks. The sutures are removed one week after surgery and DBS programming can be done at this visit. We recommend avoiding strenuous activity for the first month post-operatively. It can take several weeks, up to a couple months, to find the optimal settings for DBS programming and adjust medications.
Patients are given a patient controller which allows them to turn the DBS on and off (typically it’s left on the entire time); and depending on the patient we may allow for adjustment of one parameter of programming to a certain degree. Initial programming and major readjustments are done by our expert team.
After the recovery period, it is fine to fly. We will provide paperwork so the TSA is aware that you have a medical device and it is preferable to avoid going through airport scanners. However, there is only a very low risk of scanners turning off the device. When flying, patients should take their patient controller device with them to be able to verify whether the DBS is on or off.
MRIs, of the head or the body, may be considered if medically necessary, but the type of MRI machine may be restricted to a lower magnetic field (1.5 T), and certain types of MRI may require special equipment. Always tell the radiology technician of any implanted devices. Typically, the DBS is turned off during the MRI and turned on afterwards. We work closely with you to coordinate pre- and post-MRI management.
Yes. Medicare and most private insurances cover DBS because it is standard therapy for PD, ET and dystonia. DBS is FDA approved for PD. Our office would obtain prior approval from your insurance company.
Five-year and ten-year follow-up studies show sustained improvement in symptoms of PD, ET and dystonia over time. However, DBS is not a cure of PD, which typically continues to progress.
In the first few weeks, weekly visits are typical to fine-tune the adjustment of the DBS. Following that, visits are scheduled on an as-needed basis. At minimum, DBS patients follow up every 6 months to verify the battery level and ensure stability of treatment.
The leads and battery are all internalized, but in a slender person, there may be a slight bump visible under the skin of the neck and upper chest below the collarbone. In a person whose hairline is receding, the scalp incision scar may be visible and there may be two small bumps, about the size of a quarter, which can be felt or sometimes seen. The battery looks and feels very similar to a pacemaker battery.
Be sure to tell all providers that you have a DBS system in place. Of course, your referring physician and primary care physician will receive notes from our clinic. Dental care can be undertaken but with various precautions, such as avoiding dental drills and ultrasonic probes over the implant site and using antibiotics prior to invasive procedures such as root canals and implants.
Let your surgeon and the DBS team know prior to surgery. The DBS system should be turned off for the procedure or for CT scans. Electrocautery, electrolysis and radiation therapy should not be used over the implant site. There is no problem with X-ray or ultrasound.
The decision regarding driving is complex and should be determined by your providers who are well familiar with your case. In some cases, patients can resume driving as soon as they are no longer using sedating pain medications. In other cases, drivers’ evaluation testing may be advised to ensure that the reaction timing is intact.
No. Deep-heat treatments, also known as diathermy, deliver energy to treat specific parts of the body, and can result in severe injury or death in patients who have DBS in place. This includes microwave diathermy, ultrasound therapeutic diathermy and shortwave diathermy.
No.
Yes, but tell your doctor so they are aware of the DBS to avoid interference with the system.
Limited exposure (10-15 minutes) to heat equal or less than 100 degrees Fahrenheit should not cause any trouble, but hot tubs and tanning beds often result in heat exposure above the acceptable range, and therefore are best avoided.
Most household appliances will not harm the DBS, including radios, microwaves, computers. Older generation DBS systems were susceptible to accidentally being turned off or on by nearby magnets including those on refrigerators, but does not to occur with newer generation DBS. Still, you should always carry your patient programmer so you can check your system if you are not sure if it is on or off.
You can be around industrial equipment and use power tools but always carry your patient programmer so you can check to make sure your system is working properly after use. You should not arc weld.
Ask your DBS team prior to scuba diving. The device should function normally down to 33 feet of seawater. Skydiving should be avoiding because of the dramatic forces put on the head and neck which can damage the leads and connections of the DBS system.
Resources

Get Expert Care from Leading Specialists
Written and reviewed by:
The Pacific Neuroscience medical and editorial team
We are a highly specialized team of medical professionals with extensive neurological and cranial disorder knowledge, expertise and writing experience.
Last Updated:

