Shunt Removal
When is Shunt Removal Considered?
Many patients with ventriculoperitoneal (VP) shunts require them for life. However, in some cases, patients may eventually outgrow the need for a shunt. This can happen when the underlying condition that caused hydrocephalus improves, or when alternative procedures successfully restore normal cerebrospinal fluid (CSF) circulation.
Shunt removal is not taken lightly. It is only considered after careful evaluation by an experienced hydrocephalus specialist to ensure that the patient can safely live without the device.
Evaluation Before Shunt Removal
Before shunt removal, a series of comprehensive diagnostic tests are performed to determine whether the shunt is still necessary. These may include:
- High-Resolution MRI Imaging – to assess brain structure, CSF flow, and any residual hydrocephalus.
- Shunt Reprogramming – in patients with programmable shunts, the valve may be adjusted to a higher or “off” setting to test tolerance.
- Shunt Ligation (Tying Off the Shunt) – a temporary step that blocks shunt flow, allowing doctors to monitor whether symptoms return.
- Endoscopic Procedures – including endoscopic fenestration of cysts or endoscopic third ventriculostomy (ETV), which may provide long-term CSF diversion without the need for a shunt.
This stepwise approach ensures that only appropriate candidates undergo shunt removal.
The Shunt Removal Procedure
Once testing confirms that the shunt is unnecessary, surgical removal can be performed. In most cases, this is done as an outpatient procedure, meaning patients return home the same day. The surgery involves:
- Removing the shunt hardware (valve, tubing, and catheters)
- Ensuring no infection or scar tissue is present
- Closing the incision sites with minimal discomfort
Recovery is usually straightforward, with most patients resuming normal activities within a few days.
Long-Term Follow-Up After Shunt Removal
Even after a successful removal, careful long-term follow-up is essential. Regular check-ups and imaging help ensure that hydrocephalus does not recur. In rare cases, some patients may require shunt replacement if symptoms return.
Benefits of Shunt Removal
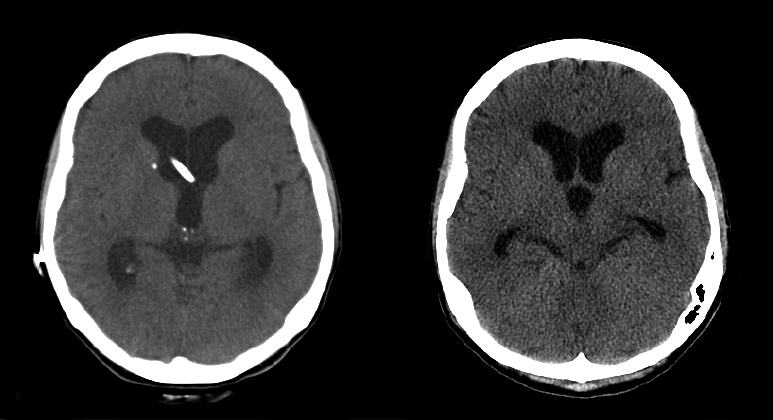
For properly selected patients, shunt removal can offer significant advantages, including:
- Freedom from lifelong device dependence
- Reduced risk of shunt infections or malfunctions
- Improved quality of life without the need for shunt revisions
