Brain Vascular Malformation
What is a brain vascular malformation?
Brain vascular malformations are localized collections of abnormal blood vessels that lead to altered blood flow. While these vascular masses are not cancerous tumors, they can sometimes grow and cause various symptoms. While in many cases a vascular malformation causes no symptoms and can go unnoticed, some cases of unruptured brain vascular malformations will cause problems by pressing on areas in the brain, irritating the brain tissue with inflammation and leakage of abnormal substances into the brain, and/or altering the blood flow from regions of normal brain (called “steal” phenomena, for stealing blood flow from where it is otherwise needed). In these cases the unruptured vascular malformation can cause symptoms that include headaches, seizures, or stroke-like symptoms, such as changes in ability to think clearly, changes in vision or speech, changes in motor function, or numbness and tingling sensations.
The word “vascular” is the Latin term for a hollow container used to transport liquids.
In medicine, the word “vascular” refers to blood vessels, or the tubes that contain and transport our blood, making up our circulation system. This system of blood vessels is how blood is conveyed from the heart to the brain, carrying oxygen and nutrients to support the brain and all its functions.
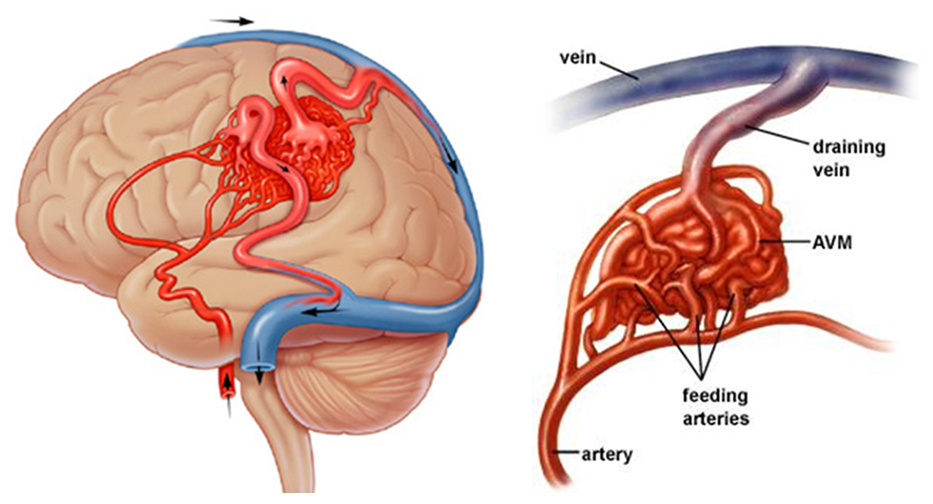
Brain vascular malformations can also become unstable and rupture, releasing blood into the brain and causing a stroke. When a vascular malformation ruptures, the result is called a hemorrhage. Depending on the severity of the hemorrhage, brain damage or death may result. Symptoms of a ruptured vascular malformation often come on suddenly and include a sudden, severe headache (“worst headache of my life”) different from past headaches, nausea and vomiting, sensitivity to light, weakness, confusion, fainting or loss of consciousness, and seizures.
Vascular malformations are typically classified by size, location, and type of blood vessels involved, with the four most common being:
- Cavernomas (cavernous angioma)
- Arteriovenous malformations (AVMs)
- Capillary telangiectasias (CTSs)
- Venous malformations (developmental venous angiomas – DVAs)
Cavernomas and AVMs in particular can be more serious diagnoses as they have the potential to cause debilitating symptoms, including the risk of rupture and bleeding into the brain. Capillary telangiectasias (CTSs) are small areas of abnormally dilated capillaries within otherwise normal brain tissue. Although CTSs most commonly occur in the pons, they have been described throughout the brain. DVAs are unusual radial vascular structures that are fully integrated with the body’s venous system and provide the brain with normal blood drainage function.
Our center specializes in the following brain vascular malformations:
Arteriovenous malformations (AVMs)
Cavernomas (cavernous angioma)
Dural arteriovenous fistula (DAVF)
When a brain vascular malformation, such as cavernoma or AVM, is diagnosed, the exact reasons that led to the development of the lesion are not currently known. Although a small number of AVMs are discovered at or shortly after birth, most of them present later in life, and therefore these masses may form and progress during the later years of life. Sometimes a person can inherit a tendency to form these vascular lesions due to abnormalities in the structure of blood vessels or altered inflammatory responses. It is thought that the same risk factors that lead other vascular lesions (like brain aneurysms) to rupture, are likely to also be associated with increased rupture risk in vascular malformations, although this is often more difficult to study because of a smaller number of patients with these diagnoses. Other risk factors can include high blood pressure and smoking. One thing that has been clearly shown is that symptomatic vascular masses that have bled in the past are at higher risk of bleeding again in the future.
Not all people who have AVMs will bleed during their lifetime. The risk is estimated to be about 4-6% per year. This means that 4-6 out of every 100 people with an AVM will have a bleed during any given year. The collective risk over one’s lifetime may be extremely high especially in a young person. For instance, in a 50 year old with an AVM who has a life expectancy of 30 years, the risk of bleeding in his/her lifetime is >70%.
If your doctor believes that you are at risk for having a vascular malformation, you may undergo one or more of the following tests in our state-of-the-art facility:
- Computed tomography angiogram (CTA) scan.
CTA is a very good method for evaluating blood vessels and can be especially useful in evaluating AVMs for the presence of aneurysms, which can be associated with AVMs. CTA uses a combination of CT scanning, special computer techniques, and contrast material (dye) injected into the blood to produce images of blood vessels. A CTA, however, is not the preferred method for evaluating cavernomas or venous malformations. - Magnetic resonance angiography (MRA).
Similar to a CTA, MRA uses a magnetic field and pulses of radio wave energy to provide pictures of blood vessels inside the body. As with CTA, a dye is often used during MRA to make blood vessels show up more clearly. MRA can be useful in evaluating both AVMs and cavernomas. - Cerebral angiogram.
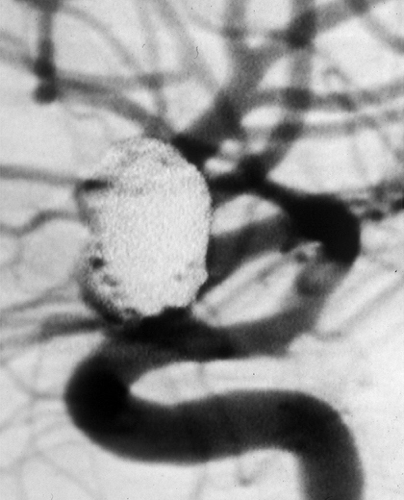
This is the “gold standard” test for the clearest images of the blood vessels. This procedure takes place in a catheterization lab, under general anesthesia, where a tiny catheter is inserted through a blood vessel in the groin and moved up from the inside of the blood vessel into the brain. A dye is then injected into the cerebral artery. As with the above tests, the dye allows any problems in the artery, including aneurysms and AVMs, to be seen clearly using specialized X-rays. Although this test is more invasive and carries more risk than the above tests, it is the best way to locate small brain aneurysms and to clearly visualize the shape and morphology of AVMs to guide treatment decision-making. While very useful in aneurysms and AVMs, a cerebral angiogram is not useful for evaluating cavernomas and most venous malformations.
The first and most important step in seeking treatment for a vascular malformation is to get an expert consultation from an advanced treatment center with expertise in all types of neurovascular treatments, including endovascular therapies and minimally-invasive microvascular neurosurgery. The Pacific Stroke and Aneurysm Center at Providence Saint John’s is certified with the Gold Seal distinction as an Advanced Primary Stroke Center by The Joint Commission, which recognizes the most advanced, comprehensive services for neurovascular patients.
Our experts in stroke neurology, interventional neuroradiology, and vascular neurosurgery work together using a team-based approach to personalize treatment decisions for each specific vascular malformation based on the location, size and shape of the lesion, the patient’s age, overall health, and additional risk factors. Sometimes multiple different treatment options are required to fully cure a vascular malformation, this is called “combination treatment.” Treatment options used to treat these lesions include:
- Minimally-invasive microvascular neurosurgery.
This minimally-invasive surgical technique involves the use of an operating microscope to perform a microsurgery with computer-assisted navigation with the aim of completely removing the vascular malformation and protecting against the risk of rupture. If the entire malformation can be safely removed surgically this technique has the advantage of offering a definitive cure. Whether microsurgery is the optimal method to treat a vascular malformation depends on the location of the lesion, its size and shape, and the patient’s general health.
- Endovascular embolization and coiling.
For AVMs and AVM-associated aneurysms endovascular therapy can be an important part of treatment. During this procedure, a small tube is inserted into the affected artery and positioned at the vascular malformation. Specialized metal coils or surgical glue are then used to close off blood flow to the AVM and/or aneurysm. Preventing blood flow into the lesion can protect against the risk of rupture. In vascular malformations such as AVMs, this is usually done as part of a combination treatment plan to reduce the size of the lesion and help prepare it for further definitive treatments.
- Non-invasive stereotactic radiation therapy or radiosurgery.
Stereotactic radiotherapy is a non-surgical procedure that can be used in the treatment of some AVMs, but does not work on cavernomas, aneurysms and other vascular malformations. This treatment is also known as radiosurgery or stereotactic radiosurgery, but overall refers to essentially the same thing. In this treatment, narrow X-ray beams are focused very precisely at the AVM such that a high dose is concentrated on the AVM itself, with a much lower and safer amount being exposed to the rest of the head. These focused beams of radiation cause the AVM to close off. The radiation delivered to the AVM works by inducing changes in the walls of the blood vessels forming the AVM. As these walls thicken, the vessels gradually close off. But it can take as long as a period of 2-3 years for this to occur, and while this can happen in up to 80% of patients, there are still those who will not respond. Until the AVM is closed off, the risk of bleeding still persists. Whether radiosurgery is the optimal method to treat an AVM depends on the location of the lesion, its size and shape, and the patient’s general health.
Contact Us
The Pacific Stroke and Neurovascular Center’s state-of-the-art facilities are located at:
Providence Saint John’s Health Center
2125 Arizona Ave., Santa Monica, CA 90404
310-829-8319
Providence Little Company of Mary Medical Center Torrance
4201 Torrance Blvd., Suite 520, Torrance, CA 90503
424-212-5340
Providence Saint Joseph Medical Center
501 S. Buena Vista Ave., Burbank, CA 90505
818-847-6049
Providence Holy Cross Medical Center
15031 Rinaldi St, Mission Hills, CA 91345
818-847-6570