
Glossopharyngeal Neuralgia
Glossopharyngeal neuralgia refers to a pain syndrome in the deep throat area related to irritation of this nerve from a blood vessel.
The glossopharyngeal nerve (cranial nerve IX or 9th nerve) supplies sensation to the deep throat. This region has significant overlap with the vagus nerve (cranial nerve X or 10th nerve), which is also responsible for swallowing. Compression of the glossopharyngeal and vagus nerves most often occurs directly at the level of the brainstem where it emerges into the fluid space. This is commonly not recognized by inexperienced surgeons. These nerves are located under and deep to the hearing and balance nerve making access particularly challenging. A blood vessel(s) could cause the compression or possibly a vein maybe responsible.
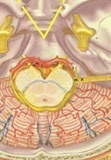
Figure 1: Demonstrates the relationship of the glossopharyngeal and vagus nerves with the brainstem.

Figure 2: A small artery is seen (circled area) causing compression of the glossopharyngeal (IX) and vagus(X) nerves at their origin at the brainstem.
Diagnosis
When small vessels cause compression at the origin of glossopharyngeal nerve and the vagus nerve, it results in a severe pain syndrome creating electrical shocks or “knife like stabbing pain” in the deep throat.
The pain may radiate and travel into the deep ear as well. The pain is aggravated by swallowing, especially cold liquids and spicy food. The pain may also come and go with periods of remission but often will progress over time.
Treatment
There are many forms of treatment recommended but in general they fall into 3 categories:
- Medical therapy
Drugs similar to that for trigeminal neuralgia have been tried for glossopharyngeal neuralgia with little success. These medications are intended to calm or improve the function of the nerve. In general, these are medications often used for seizures of the brain (Tegretol, Dilantin and Lamictal). Unfortunately, these rarely provide consistent relief and may create unwanted side-effects, such as, sedation, lethargy, cognitive impairment amongst others. Under these circumstances patients may wish to consider other therapies. - Microvascular decompression
This procedure is intended to move the offending vessel and create a cushion or pad between the glossopharyngeal nerve and the upper two branches (fascicles) of the Vagus nerve and the offending vessel(s). The decompression addresses the root cause of glossopharyngeal neuralgia by dealing with vessel that is irritating the nerve.This minimally invasive, endoscope assisted surgery involves a keyhole retromastoid craniotomy made through a small incision behind the ear. Through this small bony opening and using a high-definition endoscope and microscope, small pads of Teflon are placed between the nerve and vessel to “decompress” the nerve and allow it to function normally. Using this technique, there is little or no need for brain retraction or nerve manipulation. Occasionally also treating the nervus intermedius (part of the facial nerve – causing otic neuralgia) may improve the outcome. - Ablative therapy
These therapies are designed to ablate or selectively destroy specific fibers of the glossopharyngeal nerve. The procedure consists of a variety of approaches of cutting or sectioning the nerve. In our experience these are unsuccessful, may close the door for subsequent definitive therapy and should be kept as a last resort.
